Search
-
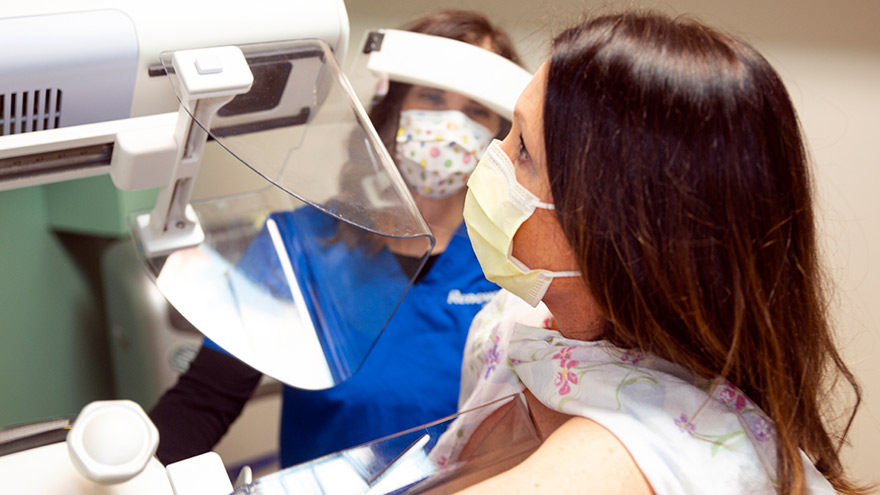
3D vs Whole Breast Ultrasound Which is Right for You
Breast cancer is the leading cause of cancer deaths in women in the U.S. That’s why early detection is so important. Dr. George Krakora, a radiologist with Renown Institute for Cancer, explains what to watch for and how new technology can lead to early detection. Most women know the importance of breast health and staying current with annual breast exams, but may not know that both screening guidelines and technology is evolving. So we asked George Krakora, MD, a radiologist for the Renown Institute for Cancer, what every woman should know about breast cancer detection and which screening method is right for them. First off, when should women start getting breast exams? Generally, women should start getting breast exams using mammography or ultrasound after they turn 40 years old. But we also want women ages 18 to 39 to talk to their primary care provider and ask for what’s called a formal risk assessment to see if screening is needed sooner. And you want to make sure your care provider is giving you a breast exam starting at age 25. It’s also a good idea to be familiar with how your breasts look and feel so you can report any changes to your care provider. What are the risk factors for breast cancer? Are there any preventive steps women can take? There a few risk factors you can’t control, like your age, family history of breast or other cancers, and if you have dense breast tissue. Your risk for breast cancer increases as you get older, and most breast cancers are diagnosed after age 50. Knowing your family history is important because a history of cancer and shared lifestyle can raise your risk. Your breast density can also increase your risk: Women with high breast density are four-to-five times more likely to get breast cancer than women with low breast density. But the good news is there are quite a few things you can do to prevent breast cancer, like not smoking, watching your alcohol intake, and maintaining a healthy weight with good diet and exercise. There are a lot of newer screenings out today. What is the difference between 2-D and 3-D mammography? In a 2-D mammogram, the tech takes X-rays of the breast. These pictures can show the radiologist if there are any lumps or tumors you might not be able to feel. In 3-D mammography, the process is largely the same but more X-rays are taken and it takes a few seconds longer for each image. This kind of exam detects 41 percent more cancers and reduces the number of false-positive results given to patients. This improvement in technology is great for both patients and their care providers. 3-D mammography provides better images of the breast, which allow doctors to more clearly diagnose and avoid false positives, especially in women with dense breast tissue. And what about a whole breast ultrasound. What is that? A whole breast ultrasound uses sound waves to detect cancerous tumors in the breast without using any radiation — it’s an ultrasound just like pregnant women get to check up on their baby. And the exam only takes about 20 minutes. We recommend these exams for patients whose mammograms have shown that they have dense breast tissue. Dense breast tissue can make it harder for doctors to see any abnormalities, lumps or tumors in a mammogram, so this technology ensures better early detection.
Read More About 3D vs Whole Breast Ultrasound Which is Right for You
-
Cervical Cancer Screenings Can Reduce Risk of Cancer
According to the American Cancer Society, approximately 14,100 new cases of invasive cervical cancer will be diagnosed, and 4,280 women will die from cervical cancer. However, cervical cancer is preventable with regular screening tests and the HPV vaccine. It’s important to note that medical advances have allowed progress in diagnosing and treating cervical cancer. While it used to be one of the most common causes of cancer death for American women, the incidence of death has significantly declined. What to Know About the HPV Vaccine HPV vaccination is the best way to prevent cervical cancer and is recommended for all youth starting as early as age 9, or for teens and adults up to age 45 who didn’t start or finish the series. In Nevada, only 50.1% of teens ages 13-17 have been vaccinated for HPV. There are 13 types of HPV, and the vaccine Gardasil 9 protects against 9 of those HPV strains, greatly reducing the incidence of cervical cancer among vaccinated individuals. What to Know About Cervical Cancer Screenings The CDC says the most important thing you can do to help prevent cervical cancer is to have regular screening tests starting at age 21. And there are two common tests that can detect early stages of cervical cancer (or precancer) and improve health outcomes. The pap test (or pap smear). This screening looks for precancers. Women should begin getting pap smears when they’re 21. The human papillomavirus (HPV) test looks for the virus that can cause these cell changes. Cervical Cancer Screening Schedule The American Cancer Society offers the following guidelines for screenings: All women should begin cervical cancer screening at 21. Women between 21 and 29 should have a pap test every three years. Beginning at 30, the preferred way to screen is with a pap test combined with an HPV test every five years. This is called co-testing and should continue until age 65. A pap test (or pap smear) is performed during a regular screening appointment to look for precancers, cell changes on the cervix that might become cervical cancer if they are not evaluated or appropriately treated. Typically outpatient procedures can reduce the risk of long-term health impacts that prevent pre-cancerous cells from becoming cancer cells. Women over 65 who have had regular screenings in the previous ten years should stop cervical cancer screening as long as they haven’t had any severe precancers found in the last 20 years. How to Get Screened Request an appointment with your primary care physician or OBGYN to schedule a screening.
Read More About Cervical Cancer Screenings Can Reduce Risk of Cancer
-
Department Spotlight: Surgical Preadmission
Heading into surgery of any kind can bring along feelings of intimidation. With a best-in-class surgery team at Renown Health, patients rest assured that they are in the most capable hands for their entire procedure from start to finish – and while the physical preparation is vital, mental and emotional preparation is equally as important to ensure each patient has a smooth and comfortable experience. The Surgical Preadmission department (a.k.a. “preadmit”) at Renown Regional Medical Center and Renown South Meadows Medical Center is a dynamic and compassionate group of nurses, case managers, chart managers and more who are dedicated to guiding each patient through the surgical process. With extensive knowledge and expertise under their belt, the teams are equipped to make a genuine difference in the health and well-being of all patients, for all surgeries, at all times of the year. Surgery Starting Ground The Surgical Preadmission teams are crucial aspects in the successful outcome of every surgical procedure. Comprised of skilled healthcare professionals, this department is dedicated to providing comprehensive support and care before heading into the pre-operating room. “Our job is to prepare every patient for surgery, make sure all their pre-surgery testing is done, ensure they understand their fasting and medication instructions, have had their questions answered, have a ride home and know what to expect during surgery and after so their recovery can go smoothly and without complications,” said Debra Bennett, RN, Supervisor of Surgical Preadmission at Renown Regional. “Each patient is unique, so each experience is different.” Our preadmit nurses are the masters of communication, directing thorough assessments – including medications, tests and clearances – and addressing any questions or concerns patients may have, never missing the opportunity to inform them of exactly what they will expect in surgery. “I do a complete history on every patient while giving them detailed pre-operating instructions and helping them answer any questions to the best of my ability,” said Nancy Hilts, Surgical Preadmission RN at Renown Regional. “I am proud to be able to help allay their fears and concerns using my 30 years of pre-op experience. I offer an avenue for them to feel comfortable opening up to me.” “We always tell patients that they have great surgeons and a fantastic team that will be watching over them and taking care of them every step of the way,” added Jon Capallupo, Surgical Preadmission RN at Renown South Meadows. “We also give them plenty of educational handouts and video content, in addition to verbal instruction, to ensure they are as prepared as possible.” The nurses then pass the reigns onto the chart managers, who prepare the charts for surgery and ensure all documentation is up-to-date before sending them to the pre-operative team. The expert surgical case managers also step in to prepare a thorough discharge plan, along with reviewing pre-operation orders for status, consent, codes and more. The team does several of these initial visits virtually, and they are looking forward to soon phasing all preadmit case manager preliminary visits into a virtual model. From assisting the pre-op and post-anesthesia care unit (PACU) teams with discharge planning concerns to helping on the outpatient side with anything from oxygen equipment and catheters to transportation issues and those experiencing homelessness, our pre-admit case managers are always up to the challenge. "We are true patient advocates, alleviating concerns and fears along the way,” said Mary Carl, RN, Case Manager at Renown Regional. “Just to name a few things we do on a daily basis, we see our total joint and non-weight bearing patients during their preadmission appointment, so they are aware of the medical equipment they need and if it is covered by insurance; provide education for Aspira catheters and gastrostomy tubes; advocate to ensure tube feeding and dressing changes are set up for hospice and home health patients; and escalate concerns of patient safety to ensure a safe discharge.” In the midst of it all, there is never a dull moment in the preadmit teams. At Renown Regional alone, the preadmit professionals see more than 1,600 patients a month – and each one has a hyper-personalized experience with their very own preadmit team. “Many times, we are the first impression a patient has on our organization; after all, we touch more than 97 percent of patients that are scheduled for surgery, cardiac catheterization lab procedures or interventional radiology,” said Amy Schler, Surgical Preadmission RN at Renown Regional. “We also collaborate with many other departments in the hospital as well, from surgeons and anesthesiologists to case managers and nurse navigators. Our work in preadmit impacts the entire surgical process.” Holding a diverse array of experiences, our preadmit department plays an integral role in our commitment to providing the highest quality of care to every patient. Knowledge is Power Heading into surgery feeling fearful and worried is normal for any patient. However, how would you feel knowing that each individual member on your preadmit team has, on average, 23-25 years of experience in the field? This is the reality for our Surgical Preadmission department – and they put that vast knowledge to great use to bring a sense of calm to patients. “Our team members have worked in various departments within our organization, and they bring a wealth of knowledge that we share with each other, and most importantly, with our patients,” said Amy Schler, RN. “If you have hundreds of years of nursing experience, you can speak not only as a nurse but also as a patient. It allows you to give a more personal perspective on what patients can expect in their recovery. Being able to assess their emotions and provide feedback to our pre-op and PACU teams help the patient have a better experience.” “Many of our nurses have close to 40 years of experience each, and they have an extremely large knowledge base since we see patients from newborn to geriatric and from easy procedures to complex surgeries,” added Debra Bennett, RN. “Another great aspect of our team is the varied nursing backgrounds we all hold – surgery, pre- and post-op, labor and delivery, pediatric intensive care, cardiology, gastroenterology, urology, cardiac cath lab, home health and everything in between. Communication between departments is so important!” All members in this department, regardless of which clinical area they came from, surgical or non-surgical, can easily translate their skills into the work they do in preadmit – and they only continue to grow. “As a surgical preadmission nurse, I have used my years of experience as a nurse in surgical services,” said Terri Delatorre, Surgical Preadmission RN at Renown Regional. “I started as a floor nurse with orthopedics for 12 years, and then I worked with the PACU for 11 years. This has helped me give great understanding and care to our surgical patients.” “Because we have staff with such a vast knowledge base, we can rely on our years of working within our organization to help alleviate fears that the patient may have,” added Amy Schler, RN. We can prepare them for what to expect in pre-op and PACU and educate them on what to expect post-op, including any barriers they may face. For example, mastectomy patients may not realize they will not be able to raise their arms for 7-10 days post-op, and total knee patients have to navigate stairs and housing access. Helping patients think about barriers at home that they may not have thought about helps them prepare prior to surgery, enhances their healing and provides a better surgical experience.” The preadmit team works closely with our best-in-class surgeons and anesthesiologists, continuing to grow their expertise along the way while learning alongside our talented providers. For instance, when it comes to our Renown South Meadows preadmit department, anesthesiologist Nariman Rahimzadeh, MD provides excellent guidance for the entire team on state-of-the-art anesthesiology practices. “I am very proud of the work we do with Dr. Rahimzadeh,” said Lisa Closson, Surgical Preadmission RN at Renown South Meadows. “Together, we ensure patients are safe for both surgery and anesthesia.” Despite the challenges that come their way – whether it be changes to process and workflow to navigating support for patients after they leave the surgery floor – the preadmit team cleverly uses their collective wealth of knowledge to bring hope and comfort to all patients. “Our nurses are such warm, caring and compassionate humans that do their best to ease any fears and anxieties patients may have,” said Debra Bennett, RN. The Pride of Preadmission The pride of our preadmit team lies in their ability to make a positive impact on all patients they serve. To them, their work is not just a job – it's a calling. And they do it all while working together to elevate their team and performance. “Our team is most proud of the quality of care we provide to our patients and our abilities to troubleshoot difficult situations to ensure they have a great surgical experience here at Renown,” said Mary Carl, RN. The entire department supports each other by working collaboratively and relying on each other’s expertise to provide the best possible care for patients. They understand that their success as a team depends on their abilities to support and help each other. “Our team is awesome here at South Meadows,” said Jon Capallupo, RN. “We can turn to each other for support, and we all work very well with each other. I am glad to be a part of this team.” “I am proud of how well all of us in preadmit works with each other every day,” added Lisa Closson, RN. “We try to make patients feel comfortable from the moment they arrive to the time they leave the department.” The pride that our preadmit team expends goes beyond their departmental limits – these team members are also trusted teachers. They work closely with cancer nurse navigators to teach weekly classes for patients who have been newly diagnosed with breast cancer, coupled with lymphedema prevention and education classes. The team also encourages participation in Renown’s free smoking cessation programs to help their patients learn the risks and benefits of quitting smoking. When not serving patients or teaching classes, you can find many of these team members taking charge of multidisciplinary committees within our health system, including breast leadership, gastroenterology leadership, shared governance, infection control and recruitment and retention. On top of it all, this team certainly knows how to celebrate, with several of their members being a part of their own department-wide Celebration Committee, where they gather for retirement parties, baby showers and team get-togethers. Always active and never passing up a challenge, our preadmit department are shining examples of Renown’s Culture Commitments, especially Caring and Collaboration, and the pride in the vital work they do every day is limitless. “I am so happy my position in preadmit opened up for me at a time when I was really feeling challenged in my career,” said Nancy Hilts, RN. “The team that we have here is amazing. I am so grateful and thankful every day for the opportunity. It is an amazing place to work!”
-
8 Important Health Screenings for Men
Unfortunately, men are less likely to visit their doctor for exams, screenings, and consults than women. So with the help of Bonnie Ferrara, MD of Renown Health, we've put together a list of eight screenings to help men stay on top of their health game. 1. Blood Pressure Tests Ages 20+ Blood Pressure tests measure the pressure in your arteries as your heart pumps. Biennial (every two years) checks are recommended if you have normal blood pressure or more frequently if you have high blood pressure (hypertension) or low blood pressure (hypotension). The United States Preventative Services Taskforce cites normal blood pressure below 120 systolic (top number) and 80 diastolic (bottom number). 2. Cholesterol Screening Ages 20+ High levels of cholesterol increase your risk of stroke and heart disease. A simple blood test will help your healthcare provider determine your numbers and if you're at risk. If you have a family history of diabetes or heart disease, you may need yearly screenings. But, again, your doctor can provide the best course of action.
-
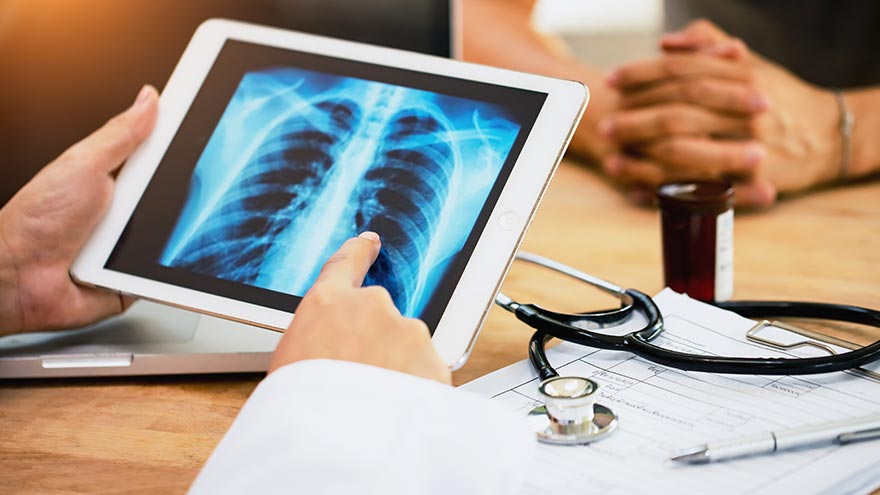
Lung Cancer Screening and Early Detection
Lung cancer is the leading cause of cancer deaths in both men and women in the U.S. The good news is the five-year survival rate increases dramatically if lung cancer is treated before spreading to other parts of the body. Julie Locken, MD, of Renown Health Imaging, explains more. What are the signs and symptoms of lung cancer? As you might expect, most lung cancer symptoms appear in the chest and can affect your breathing. Watch for signs such as: Persistent cough Constant chest pain Shortness of breath Wheezing Bloody or rust-colored phlegm Hoarseness Swelling of the neck Pain or weakness in the shoulder, arm or hand Recurring pneumonia, bronchitis or other lung infections Loss of appetite and loss of weight can also be signs of lung cancer That said, there are usually no symptoms in the early stages of lung cancer, which means getting screened can truly be a lifesaver. If you have a history of smoking, you should get screened as a precaution. What are the risk factors of lung cancer? Around 80% of lung cancer cases stem from a history of smoking tobacco. But there are other known causes, such as secondhand smoke, radon, asbestos and diesel exhaust. It’s important to do what you can to eliminate exposure to all of these to reduce your lung cancer risk. People with an immediate relative – a parent, sibling or child – diagnosed with lung cancer and people between 50 and 80 years old are also at higher risk and may need to consider screening. People who are at the highest risk are those with a history of smoking tobacco, particularly smokers who averaged one pack of cigarettes per day for 20 years or more, as well as former heavy smokers who quit in the last 15 years.
-
Ladies! Get Screened for Breast Cancer
Early detection is a significant piece of the breast cancer puzzle. Susan Cox, Renown Health Director of Cancer Operations, discusses what you need to watch for and how the latest technology can help detect potential cancer sooner. When should women start getting breast exams? It depends on risk factors: Average-risk women: Most medical organizations recommend the first mammogram between 40 and 44. Higher-risk women: Dependent on their high risk, which will dictate when they start screening, but generally around the age of 30 and not before 25 years old.