Search
-
Use Caution: Mixing Over-the-Counter Medications Can Be Harmful
With allergy season’s extended stay and cold and flu season having just begun, you may soon find yourself seeking relief through several different kinds of over-the-counter medications. Know what precautions you need to take when fighting multiple symptoms with multiple medications. When you’re too sick to go to work but not sick enough for a doctor’s visit, over-the-counter medicines are a welcome relief to help alleviate that fever, runny nose or allergies. But because those medicines aren’t signed off on or managed by your doctor and pharmacist, it’s crucial that you’re especially mindful of what you put into your body. Whenever you pop a pill, you want to make sure you’re taking the right dosage, waiting the right amount of time before taking another dose and not mixing certain medicines together. Recent stories like this one detail dangerous over-the-counter medicine combinations, and we’re following suit: Here is a quick go-to guide about potentially harmful over-the-counter combinations. Too Much Tylenol/Acetaminophen Tylenol — or acetaminophen — is a popular pain reliever for many, but too much can be bad for your liver. “Our bodies have a finite ability to metabolize Tylenol,” says Andy Wright, clinical pharmacist at Renown Rehabilitation Hospital. “When too much builds up in the liver, it becomes toxic. In patients with medical conditions like cirrhosis of the liver or hepatitis, this could be disastrous.” Remember, acetaminophen is in more than just Tylenol and generic pain relievers. You may also see acetaminophen in flu, cold and cough medicines, like Nyquil, and some prescription medications including Norco and Percocet. Keep a list of the medications you take, and limit daily acetaminophen use to 3,000 mg per day. When you’re scanning medicine bottle contents, remember acetaminophen is also referred to as APAP, AC, acetam or paracetamol. Mixing Painkillers When you’re dealing with pain and not getting any relief, taking a different medication may seem like the easy solution. Maybe you take some Aleve — a form of naproxen — for a headache, but it isn’t working, so you switch to Motrin, an over-the-counter form of ibuprofen. Not a smart idea. Ibuprofen and naproxen along with aspirin are known as nonsteroidal anti-inflammatory drugs (NSAIDS). Because these medicines work in similar ways, they should never be combined or used in larger doses or more frequently than directed. Otherwise your risk of side effects can increase, which range from mild nausea to severe gastrointestinal bleeding. It’s also important to consider your family history when taking NSAIDs because, “recent studies have shown NSAIDs may have greater cardiovascular risks for people taking blood thinners or those with hypertension,” explains Andy. “A good example is ibuprofen: It has a relatively low gastrointestinal bleed risk while it has a moderate to high cardiovascular risk. The opposite is true for naproxen.” Rather than experimenting with multiple medicines, figure out which drug works best for you. You may find muscle soreness improves with aspirin, whereas when a headache hits, naproxen is best. Keep in mind that these medications aren’t always best for everyone in the family. “Aspirin in children and teens is not recommended unless under the supervision of a doctor,” Andy says. And pregnant and lactating women should generally avoid NSAIDS due to risk of birth defects and bleeding. “In both of these cases, acetaminophen or Tylenol are preferred but only if approved by an OB/GYN.” Fighting Allergies Over-the-counter antihistamines like Claritin, Zyrtec and Allegra have made fighting itchy eyes and runny noses a little easier. But these daily medicines — when taken inappropriately or in the wrong combinations — can also have an adverse effect. Similar to acetaminophen, you need to watch for antihistamines in other products. Sleep aids — like Tylenol PM and Unisom — commonly use an antihistamine known as diphenhydramine, which may increase your risk of overdose. “Combining antihistamines, or overdosing, can cause many adverse effects including dry mouth, blurred vision — even arrhythmias,” Andy says. “Only take these medications on their own.” If you’re still struggling with symptoms, you can talk to your doctor about adding an over-the-counter nasal steroid. Andy confirms the importance of closely following the directions listed on antihistamine (and all medicine) bottles. He has seen extended release nasal decongestants cause significant arrhythmias requiring medical care after a patient took the medicine with warm fluids. “The decongestant in question is designed to slowly release, but it can dissolve suddenly in the presence of warm liquids like coffee,” Andy explains. “This can cause the pill to deliver 12 to 24 hours of medication all at once.” Taking an Antidiarrheal with Calcium Calcium supplements and antidiarrheal medicines are another harmful combination. Calcium firms up your stool, but if taken with an antidiarrheal, can cause severe constipation. If you need to take an antidiarrheal, take a break from your calcium for a few days until you’re back to normal. Another consideration when taking calcium supplements or calcium-based antacids is gas. “I’ve had several patients report cases of excessive gas using Tums or calcium carbonate-based supplements.” Andy suggests instead “trying Maalox or Mylanta for indigestion and Citracal as a supplement.” Talk with Your Doctor or Pharmacist About Your Medications If over-the-counter drugs aren’t providing the relief you need, it’s time to see your doctor. And remember, for your safety it is important to keep your doctor and pharmacist up-to-date with any medications — prescribed or over-the-counter — that you are taking.
Read More About Use Caution: Mixing Over-the-Counter Medications Can Be Harmful
-
Get to Know the Types of Car Seats
Parents often struggle with installing and choosing car seats for their children. Picking out a car seat for your child is a never-ending battle. Safe Kids Washoe County has made it simple for you to understand the types of car seats that will work for your child. Types of Car Seats Rear-Facing Only Seat. Your baby's first car seat is often used from 5 to 40 pounds. People usually buy this type of seat because it is portable. Convertible Car Seat. This seat is larger and stays in the car; it may be rear-facing until your child is two years or more. After that, it can change to a forward-facing seat. Forward-facing-only car seat. This type of seat is used in one direction and has a 5-point harness and top tether. Combination seat. This is a forward-facing seat with a 5-point harness and top tether and can change into a booster seat when you remove the harness. 3-in-1 car seat. This seat also stays in the car. You can use it rear-facing, forward-facing, and then later, as a booster seat. Booster seat. It boosts the child for a safer and more comfortable fit of the adult seat belt. Make sure your child has outgrown the weight or height limits allowed in the forward-facing car seat. The seat belt must lie flat across your child's chest, on the bony part of the shoulder, and low on the hips or upper thighs. Most children will be between the ages of 8 to 12 years old before they are ready for the seat belt alone. Have a trained car seat technician check your installation Why: 3 out of 4 car seats are installed improperly, with some studies show that the misuse rate is 90%, with the average car seat having three mistakes. Solution: Ensuring that your child's car seat is installed correctly by a certified car seat technician will ensure your child's safety.
-
Transitioning Your Child Out of Their Car Seat
Car seat technicians often find parents are moving their child to their next car seat stage too soon, as they get older. Here are a few reminders of when to transition your child from their booster seat to a seat belt. Moving to a booster seat too soon According to Safe Kids Worldwide, nearly 9 in 10 parents remove children from their booster before they’ve reached the recommended height, weight, or age of their car seat recommendations, which leaves the seat belt in a position on the child that could injure them. If the child is not the proper height, the seat belt can rise up on the belly, instead of the hips where it’s supposed to sit, which can lead to spinal cord damage or whiplash in the event of a car crash. Solution: You can switch from a car seat to a booster seat when your child has topped the weight allowed by the car seat manufacturer; typically 40 to 80 pounds (18 to 36 kilograms). Remember, however, that your child is safest remaining in a car seat with a harness for as long as possible. Booster seats must always be used with a lap and shoulder belt — never a lap-only belt. Transitioning to a safety belt too soon Older children need booster seats to help ensure the seat belt stays properly positioned on their body. The lap belt should lie low across the child's hips and pelvis with the shoulder belt crosses the middle of the child's chest and shoulder, so that in the event of a crash, the forces are applied to the hip bones and not the abdomen. If the lap belt is not positioned properly then it could lead to injuries to the spinal cord and abdominal organs. Solution: Most kids can safely use an adult seat belt sometime between ages 8 and 12. Always use a booster seat until the child passes the 6-step test Your child reaches a height of 4 feet, 9 inches (nearly 1.5 meters) Their back is flat against the seat back. Knees bend over the edge of the seat and feet are flat on the floor. The shoulder belt sits on their shoulder and chest (not face or neck.) The lap belt sits low on their hips and touches their upper thighs (not on their stomach.) Your child can sit comfortably this way for the entire trip. The American Academy of Pediatrics reminds us that the back seat is the safest place for children younger than age 13.
Read More About Transitioning Your Child Out of Their Car Seat
-
Pool Safety: Things To Know About Drowning
The warm weather is here and pools are open. Swimming is a great way to keep your kids cool, occupied and exercised throughout summer, however pools come with their fair share of risks. Before you take your children swimming, check out these pool safety tips. Pool safety is something every parent needs to take more seriously. Why? Because drownings of young children ages one to four have increased in recent years. Unfortunately, drownings are the number one cause of death in this age group - we lose the equivalent of 10 school buses full of children to fatal drownings in the U.S. each year. With warmer temps and hopes of cooling off in a local pool, you can’t be too careful when it comes to protecting your children from the risk of drowning. Children are naturally drawn to water, so parents must be extra aware in order to protect their kids from diving in headfirst. Kris Deeter, MD, pediatric intensive care physician at Renown Children’s Hospital, offers tips to keep your littles safe in the water. Preparing Your Child for the Pool People aren’t born knowing how to swim. This means parents must teach their children about swimming and pool safety if they want them to be safe and confident around water. It can take years to develop these skills, so the key is to start when your children are very young. Here are some ground rules: Teach your child to swim starting at age one. We recommend enrolling your toddler in swim classes; there are several organizations in the Reno-Tahoe area that offer baby and toddler swim classes. Keep your kids away from plastic and inflatable pools - they’re easy for children to fall or climb into and drown. They’re also a breeding ground for bacteria. Floaties and water wings are not safe! They are not a safe substitute or “crutch” for learning how to swim and they can lead to drowning if the child is using them incorrectly or while unsupervised. Stay within arm’s reach of babies and toddlers when at the pool. Supervision alone is not enough – you must be within arm’s reach in case they fall in and need to be rescued quickly. Learn child and infant CPR. If a drowning does occur, the best course of action is to call 911, get the child onto dry land and conduct CPR until breathing is restored or the EMTs arrive. Pool Parties: A Risk for Drowning? Surprisingly, pool parties, a common summer pastime, actually increase the risk of drowning incidents. Although responsible adults are usually at pool parties, distractions ranging from alcohol to pool toys can actually make it easier for drownings to occur unnoticed. Does this mean you should RSVP “no” to the next pool party your child is invited to? Not if you follow the pool safety tips below: Attend the party with your child so you can supervise them while they swim. Remove unused floaties and toys from the pool. They can obscure visibility, making it difficult to see a child in the pool. Don’t drink alcohol while supervising a pool party. Assign an adult “water watcher” to pay constant attention to children in the pool. Pool Safety Precautions for Homeowners If you own a pool, there are several more precautions to ensure the safety of your children. Even if your kids are strong swimmers who have mastered the rules of pool safety, there may be neighbors or friends who are younger and more vulnerable to drowning. You must undertake precautions for these children too. Some of these may seem time-consuming or expensive, but they are worth it to prevent a child from a fatal drowning. To keep your pool or spa safe, please: Cover your pool or spa when not in use. Choose a pool or spa cover with safety features like locks, safety sensors or alarms. Fence in your pool or spa area. The fence should be locked and at least four feet tall. Do not leave toys in the pool area as these may attract children.
-
2 Dangerous Car Seat Mistakes and Solutions
Car seat mistakes can have very serious consequences. Misuse of a car seat can injure your child, or fail to keep them safe in the event of a crash. A lot goes into finding the right car seat for your child. With so many factors to consider (including age, weight and height of the child, type and brand of a car seat, cost of the car seat, etc.) it can be easy to forget critical factors. Here are two common mistakes that certified technicians often find when speaking with parents. Mistake #1: Getting a used car seat without knowing its history Why: A used or secondhand car seat can pose several factors that can compromise its safety in a crash. First, car seats expire six to ten years after their date of manufacture, so refer to the car seat's manual for recommended car seat longevity. The safety mechanisms can be compromised if a car seat has been in a crash. So it's crucial to replace your car seat following a collision. Solution: Only use a car seat if you know its history. A new car seat is your best bet, as they are up to date on the latest safety guidelines, and safety mechanisms are up to standard. However, if you are considering a used car seat for your child, please ensure the following: The car seat has never been in a car crash. The car seat isn't expired or outside the manufacturer's recommended longevity. It comes with the car seat manual and has all safety labels, including manufacture date, model number, and use instructions and restrictions. The car seat or any of its parts have not been recalled. The overall state and integrity of the car seat and its parts are undamaged. The carseat or any of its parts have not been recalled and are present and in working order.
-
Stroke Survival as a Warrior – Kimi's Story
It seemed like a normal Wednesday, except Kimi Woolsey was feeling really stressed. On Sept. 4, 2019 she was rushing to get ready for an appointment when suddenly, she could not feel her legs. Kimi immediately knew something was wrong and called out to her fiancé, Paul, for help. After seeing a bright light in her right eye, she felt a severe, sharp pain in her head traveling down into her leg. Paul quickly called 911, the EMT’s arrived and her stroke survival journey began. At first the medical team thought she had a complicated migraine, but one of them suspected a stroke. On the way to the hospital Kimi felt numbness and her face drooping, then instantly, no pain. For a moment she thought she was dying, going from pain to numbness and realizing she couldn’t move or speak. Kimi didn’t know she was having another massive stroke in transit. Each year nearly 800,000 people in the U.S. suffer a stroke, or “brain attack” – that’s one every 40 seconds. Of those, about 75% occur in people over age 65. However, at only 45 years old, Kimi is proof that a stroke can happen at any age. Stroke Survival Begins for Kimi Upon arriving at the emergency department of Renown Regional Medical Center the Certified Comprehensive Stroke Center team went into action. Kimi received a brain MRI, then was wheeled into surgery for a thrombectomy (clot removal). She was in the intensive care unit for 11 days. She remembers someone telling her, “Generally people don’t survive this magnitude of stroke.” And a doctor saying, “You are here for a reason.” Kimi’s comeback journey began with the comprehensive care team at Renown Rehabilitation Hospital. “Literally I had the best day of my life that first day there…I was so happy because I couldn’t imagine being in a safer place with people that literally live for you,” she recalls. During her 41 days there, her biggest milestone was being able to get out of bed and walk. For Kimi the support she felt at the rehab hospital was key to her progress, ”I still feel loved and appreciated and they’re rooting for me still and I can feel it.” Although she left the rehab hospital on Oct. 18, 2019, she is still working on improving the left side of her body. Currently Kimi works with therapists in outpatient physical rehabilitation sessions, continuing to see improvement in both her hand and leg. Her advice to those currently in a rehab hospital setting is, “Stay as long as you can to get the most out of it and push, push, push.” Kimi’s Stroke Survival as a Warrior “Having a stroke is not for the faint of heart,” says Kimi. She experienced despair and felt discouraged. Many days she would ask herself, “Why am I here?” Today she proudly calls herself a stroke warrior and refuses to be a victim of her stroke. Alongside her tenacious spirit, Kimi actively helps others on their stroke survival journey. Before her stroke she never dreamed of starting a non-profit foundation. Now, each day you’ll find her texting inspiration to others, offering advice and connecting with other struggling stroke survivors on her Facebook page, Stroke Warrior Recovery Coach. Her goal is to become the person she needed to talk to after her stroke; she currently coaches several stroke survivors. “Stroke survivors need to know that they aren’t alone. Mental support and encouragement are so important for each person’s stroke journey,” Kimi said. Along with the physical changes, Kimi feels the stroke magnified her empathy. “I was always in a hurry in my life. People didn’t go fast enough for me – on the road, at the grocery store, in a line. Now I have more patience with myself and others." Kimi realizes most people cannot wrap their brain around the concept of a stroke. In fact, the brain fog, physical challenges and frustration are hard to explain… unless you’ve experienced them. “You need to find your tribe,” she explains. “I have a passion for helping people through this process.” Most of all, she encourages people to keep going and never stop. After her stroke, Kimi has a greater appreciation for her family, health and life. She is one of the patients featured in the current “Fight The Good Fight” trauma and physical rehab advertising campaign. “I wake up every day and fight,” she asserts. “Each day you have to fight for your recovery and fight for yourself.”
-
Heart Attack Survivor Fights the Good Fight
Something wasn’t right. Even though it was the holiday season, on December 23, 2018, Mondo Corona didn’t feel good…not to mention his sudden earache. Although Christmas was a happy celebration with his family. He still felt tired. Was it the flu? And that darn earache wouldn’t go away. On that cool winter day, Mondo could not imagine he was near death. Or that he would become a heart attack survivor. Know Your Heart A few days later, on December 27, he wasn’t feeling any better. He decided to go to the emergency room at Renown Regional Medical Center. That’s when a simple blood test revealed shocking results. “I thought about death a lot. I was calling people to ask them to help take care of my family if I wasn’t going to be here anymore,” he emotionally confesses. Although Mondo loves his job as a railroad engineer, it involves on-call shifts and an erratic sleep schedule. At that time his exercise and eating habits weren’t the best either. Yet he never imagined he would have a massive, often lethal, type of heart attack called ‘the widowmaker.’ In fact, his family had been concerned about his health for awhile. “He worked so much and he didn’t take care of himself and he didn’t exercise – he was burning the candle at both ends,” shares his wife, Alison. His daughter Justice, an avid exerciser, was always encouraging him to join her at the gym, but could never quite convince him. Mondo remembers the time before he became a heart attack survivor. “I didn’t have any exercise whatsoever in my life. At that point my eating habits were just terrible,” he shares. He went to the emergency room due to his earache, but nothing was found until one of the doctors ordered some tests. Specifically blood work showed high troponin levels. Troponin is a blood protein often released in large amounts when the heart muscle has damage, sometimes by a heart attack. Heart Attack Survivor “My surgeon came in and told us that it was going to be a triple bypass – that three of the four…major arteries were clogged 100 percent,” Mondo explains. Amazingly his heart was pumping on only 10 percent blood flow. Heart surgeon, Joseph Brandl, MD, told him he survived a widowmaker heart attack. This type of heart attack happens when there is a 100 percent blockage in the critical left anterior descending artery (LAD) of the heart. Frequently the symptoms can often be mistaken for the flu. According to the Centers for Disease Control and Prevention (CDC), every 40 seconds a person in the U.S. has a heart attack. And 1 in 5 heart attacks are “silent” – meaning you can be a heart attack survivor, but not know it. For Mondo’s children, seeing their strong father struggle after heart surgery was difficult. Justice tearfully shares, “It was really hard seeing him so vulnerable. He really needed anybody’s and everybody’s help at that point.” A Heart Attack Survivor Program After leaving the hospital on January 5, 2019, he was extremely weak. On February 12, Mondo began Renown Health’s Intensive Cardiac Rehabilitation (ICR) Program called the Healthy Heart Program. This program, requiring a doctor referral, includes 12 weeks of supervised exercise along with nutrition education and stress management skills. In spite of heart disease being the leading cause of death in the U.S. – more than all cancers combined, the risk can be lessened with daily lifestyle habits. Mondo credits the ICR program with motivating him and getting his focus back on his health. He saw the team members setting an example and also caring about his health. He describes one of his favorite recipes, “In ICR Sara showed us how to make this incredible fruit salad, with jicama, watermelon, grapes, oranges, red onion, and ginger!” Of course, the recovery process was not overnight. “It did take a long time to really realize that he was going to be back to normal, that he was going to be okay and that he was going to be that strong provider for me and my children,” Alison reflects. “Mondo’s had an amazing outcome and he’s not limited in his activities at all and should hopefully have a life that’s not limited at all from heart disease as we’re monitoring everything and everything’s looking good,” reports his heart doctor Jayson Morgan, MD. Mondo describes his care experience being a heart attack survivor as life-changing. “The care teams at both Renown and ICR were incredible. There wasn’t a single person we came across who didn’t immediately become a part of the family. They truly cared for us, all of us, including the extended family that came to visit. They were informative and supportive. I felt like I created lasting bonds with so many of them, especially the gang in ICR. What amazing people.” Lynice Anderson, Director of Intensive Cardiac Rehab, Healthy Heart Program, shares,” Mondo is one of the most genuine, thoughtful and humble people I have ever met. His love for his family is palpable. His impact on me personally and our team is forever.” She acknowledges family support is key to his success, “Mondo’s family is his rock and they are his. I have never met a family that was so ‘all in’ in the support of their loved one. His new heart healthy lifestyle is modeled through his family every day.” Fighting The Good Fight Of course, Mondo may look familiar to you. That’s because he is featured in Renown Health’s “Fight The Good Fight” brand campaign. For this reason, you may have seen him in advertising working out on a treadmill, shirtless, with his open heart surgery scar in full view. When asked how he feels about showing his scar he confidently says, “I don’t mind showing it to people. I don’t. I earned that scar.” He is a proud heart attack survivor. Today, he’s grateful to be alive and takes his health commitment seriously. “Things have a different feel now. The skies and lakes are bluer and the trees greener. My family is so much more a part of my day. We go on so many more outdoor adventures, trying to incorporate a little exercise into our fun. We watch what we eat more and are trying to teach our children and loved ones about healthy choices. And I think with a few we’ve even been successful!” he observes. “Don’t take life for granted.” “Unconditional love. I get nothing but support from my family without them I wouldn’t be where I’m at. What happened to me definitely makes me a fighter for sure. I’m fighting for my life – the good fight – I think life is good,” he adds.
-
The Risks of Vaping and E cigarettes
In this article reprinted with permission from the Galena Times, Dr. Max J Coppes, Physician-in-Chief, Renown Children’s Hospital, and Nell J. Redfield, Chair of Pediatrics, UNR Med, talk about adolescents vaping, and how an estimated additional 10 million teens are at risk to start using e-cigarettes. What are E-cigarettes? E-cigarettes are battery-operated devices heating a liquid (e-juice) into an aerosol to be inhaled. Breathing in this flavor vapor, which usually contains nicotine, anti-freeze or other cancer-causing chemicals is called ‘vaping.’ There are many forms of these electronic nicotine delivery devices - and they're not always obvious. They not only appear to be cigarettes, cigars, or pipes, but also pass for everyday items, such as flashlights, flash drives or pens. The Effects of Vaping and E-cigarettes Regardless of the nicotine delivery, vaping is addictive and is quickly becoming a public health concern. Nicotine levels in e-cigarettes vary greatly, and they may also contain toxic chemicals. Currently there is a wide range of variability among vaping products. In other words - they deliver different ingredients, hardware, levels of nicotine, and possible toxic chemicals to the user. This makes it challenging to create an overall public health recommendation on their use. Nevertheless, there is no confusion about the harmful effects of the chemicals used in e-cigarettes to the young brain, which develops until age 25. Studies show e-cigarette use serves as an introductory product for teens to go on using ‘regular’ tobacco products. The American Academy of Pediatrics has several recommendations on their use. Such as increasing the minimum age to buy tobacco products, including e-cigarettes, to age 21 nationwide. (Update: nationwide the age as of January 2, 2020 is now 21.) A common misunderstanding with teenagers is the belief e-cigarettes are less harmful than other tobacco products. Moreover, there is a wide range of flavor choices, from mint, mango, crème brûlée to cucumber to attract users. As of September 6, 2019, The Centers for Disease Control and Prevention is reporting over 450 possible cases of lung illness associated with the use of e-cigarette products in 33 states. What Should Parents Know about Vaping? Parents and teachers should know JUUL is a very popular e-cigarette among teenagers, capturing about 68% of the market. JUUL is sleek, small, hides easily, and resembles a flash drive. Surprisingly it charges in an USB port, and can also instantly be mistaken for a real flash drive. One JUUL cartridge contains twice the nicotine found in other e-cigarette cartridges. This roughly equals the amount of nicotine in an entire pack of cigarettes. To repeat, the use of JUUL in young people continues to grow, and this is why parents and teachers need to be aware. Be alert, teach, communicate, and talk to your child about the serious risks of smoking in all forms, whether at home or parties. Tell them how difficult it is to quit and why they should not start. Loving your children is caring; caring for their current and future health and well-being.
-
Generic Drugs – What You Need to Know About Them
Without a doubt, taking medications can not only be expensive, but also confusing. In the United States, generic prescriptions are widely used, with 9 out of 10 people choosing them over a name brand. Pharmacists are a great resource to help us understand the benefits and side effects of any medication. We asked Adam Porath, PharmD, Vice President of Pharmacy at Renown Health, to answer some common questions about generic drugs. What is a generic drug? A generic drug has the same active ingredients of brand-name drugs. Brand-name drugs have a patent (special license) protecting them from competition to help the drug company recover research and development costs. When the patent expires other manufacturers are able to seek approval for a generic drug. However, the color, shape and inactive elements may be different. Per the U.S. Food & Drug Administration (FDA), a generic medicine works in the same way and provides the same clinical benefit as its brand-name version. Why do they cost less? Generic drug makers do not have the expense of costly development, research, animal and human clinical trials, marketing and advertising. This savings is passed on to the public. Also after a patent expires, several companies will compete on a generic version of a drug, further driving down prices.
Read More About Generic Drugs – What You Need to Know About Them
-
From Cancer Survivor to Caregiver
Meet Haley Carroll Being a new nurse comes with many challenges and gaining experience is a journey, but Haley Carroll’s first day on the job was far from her first day in a hospital. Haley was diagnosed with lymphoma right before her senior year of high school, and she was declared cancer-free on December 2, 2015. Inspired by the incredible care she received during her cancer treatments and during her time at Renown Children’s Hospital, Haley enrolled in nursing school at the University of Nevada, Reno. She graduated in December 2020, just five years after beating cancer. “I’ve always been interested in nursing,” Haley says. “But once I was diagnosed and began to see everything that my nurses did for me, I knew that that’s what I wanted to do for patients, too.”
-
The Road to Recovery Close to Home
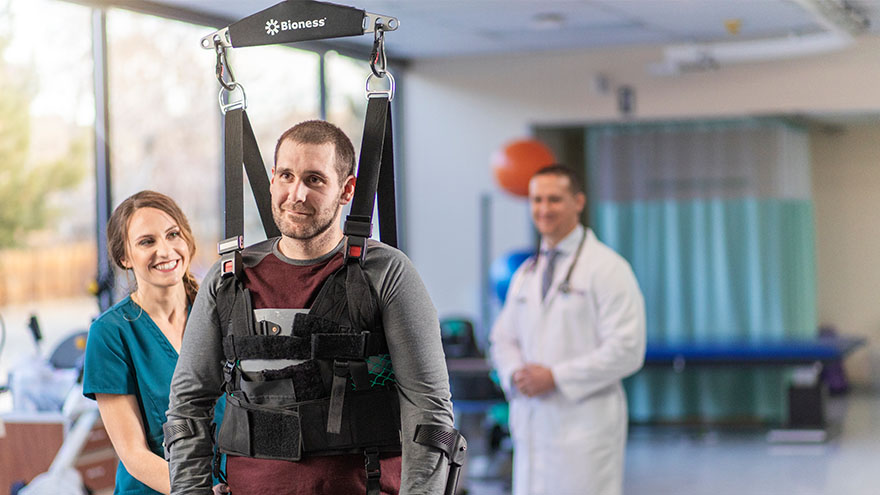
Meet Connor Smith Life was hectic for Connor Smith. He had just finished at the top of his class at both the fire academy and paramedic school and was looking forward to starting work in northern Nevada. It was winter 2019, and he was ready to have some fun. The plan was to ride ATVs at Sand Mountain with his brother Cody, dad Lance and some friends, but a jump would change everything. Connor’s ATV took off but landed awkwardly, and he remembers immediately knowing he was paralyzed. Connor’s mom, Dana Shugar, was at home when she received the upsetting call from Cody, who told her he had an accident. Connor was flown to Renown Regional Medical Center, the area’s only Level II Trauma Center. After a seven-hour emergency surgery, Dana learned that Connor would live but only had a slight chance of walking again due to a spinal fracture. “The surgeon saved his life. It’s amazing how your life can change in a matter of seconds,” she said. Once his condition stabilized, Connor moved to the Renown Rehabilitation Hospital and began physical rehabilitation. “Thank God for the people at rehab,” Dana said. “Dr. Pence, the therapists, nurses and all the employees were a wonderful support system, explaining everything and answering all our questions. The kindness they showed got me through.” Connor agrees, calling the Renown rehab team nothing short of amazing.
-
A Family's Legacy
Dr. Derek Beenfeldt first joined the Renown family in 2014 as a family medicine physician after graduating from University of Nevada, Reno, School of Medicine (UNR Med) in 2011. His son Davis was only 10 years old when Dr. Beenfeldt decided to change careers and attend medical school. Ten years later, Davis is following in his dad’s footsteps as a third year student at UNR Med. “I am proud of Davis for taking on the challenges and the commitment that I know goes along with attending medical school,” Dr. Beenfeldt said. “I also feel lucky that we have a medical school with such a great reputation and resources close to home.” The affiliation is a great source of pride for Dr. Beenfeldt. Not just because two important organizations in his life are joining forces, but he also sees it as both entities taking on an immense responsibility – the challenge to be better for incoming students, and subsequently to improve healthcare in Nevada. Davis is currently going through his rotations and spending countless hours a week at Renown Regional. His dad is right there by his side supporting him along the way. “It has been really interesting to have discussions about the UNR medical school with Davis, I recognize the names of many of the professors and courses from when I was a student,” Dr. Beenfeldt said. “I tried to be empathetic, as I can relate to how difficult and stressful this time is for him. Dr. Beenfeldt currently works as chief medical officer for Renown’s insurance arm Hometown Health, and Davis is still browsing specialties. “I don’t know what kind of medicine I want to focus on yet, but I feel lucky that I can attend medical school so close to home and have the option to continue helping my fellow Nevadans after I graduate.” UNR Med at a Glance UNR’s Medical School was established in 1969 Over the last 50 years, UNR Med has educated 3,900+ physicians More than 30% of UNR Med physician graduates continue to practice in Nevada UNR Med is the state’s oldest medical school