Search
-
SOGI – The Most Important Terms to Know
SOGI stands for sexual orientation and gender identity. Being a SOGI-inclusive medical facility means regardless of our differences, we treat others with dignity and respect. Sean Savoy, Renown Health Manager of Spiritual Care, explains SOGI terms and their importance in a healthcare setting below. SOGI History Although the UN passed a historic resolution on SOGI in 2016, it is still a relatively new term for some. Above all, an inclusive environment where every patient feels safe and valued, improves the quality of care in our community. In reality, defining gender and sexuality can be confusing. However, the terms we use to define gender and sexuality are an important influence on how we relate to each other. Generally, "sex" refers to the biological differences between males and females. Still the term “sex” doesn’t fully capture the complex biological, anatomical and chromosomal variations that can occur. Accordingly, having only two (binary) options – biological male or biological female – might not describe what’s going on inside a person’s body. In essence, assigned sex (also called "biological sex) is given at birth based on medical factors. These include your hormones, chromosomes and genitals. Most people are assigned male or female, and this is what’s put on their birth certificate. When someone’s sexual and reproductive anatomy isn’t clearly female or male, that person may be described as “intersex.” However, a person’s biological or assigned sex may be different from a person’s actual or perceived gender identity or expression. The word “gender,” therefore, is more difficult to define. It could refer to the gender or sex role society determines is acceptable, desirable or appropriate based on a person’s perceived sex. Likewise, it could refer to an individual’s own gender identity or preferred gender expression. What is Gender Identity? To summarize, gender identity is one's innermost concept of self as male, female, a blend of both or neither. To clarify - how individuals perceive themselves and what they call themselves. Of course sometimes a person's genetically assigned sex does not line up with their gender identity. These individuals might refer to themselves as transgender, non-binary, or gender-nonconforming, for example. Another key point is the process of gender transition. This specifically refers to more closely aligning your internal knowledge of gender with your outward appearance. According to the American Psychiatric Association's Diagnostic and Statistical Manual of Mental Disorders (DSM), the term – which replaces Gender Identity Disorder – "is intended to better capture the experiences of affected children, adolescents, and adults." What is Sexual Orientation? Sexual orientation is an internal or enduring emotional, romantic or sexual attraction to other people. For example, you could be heterosexual (straight), gay, lesbian, bisexual or even pansexual. SOGI Terms to Know Below are some common SOGI terms according to the National LGBT Health Education Center and the Human Rights Campaign. The following list is not meant to represent every term (or definition) used by the LGBTQ+ community. LGBTQ+ Stands for lesbian, gay, bisexual, transgender and queer (or questioning). The plus encompasses other identities that fall under the queer umbrella with one common theme: they are not strictly straight or cisgender. Queer An umbrella term used by some to describe people who think of their sexual orientation or gender identity as outside of societal norms. Some people view the term “queer” as more fluid and inclusive than traditional SOGI identities. Due to its history as a derogatory term, the term is not always embraced or used by all members of the LGBTQ+ community. Sexual Orientation Terms Asexual (adj.) – Describes a person who experiences little or no sexual attraction to others. Asexuality is not the same as celibacy. Bisexual (adj.) – A sexual orientation that describes a person who is emotionally and sexually attracted to people of their own gender and people of other genders. Gay (adj.) – A sexual orientation that describes a person who is emotionally and sexually attracted to people of their own gender. It can be used regardless of gender identity, but is more commonly used to describe men attracted to other men. Heterosexual or Straight (adj.) – A sexual orientation that describes a person whose sexual or emotional attractions and behaviors focus exclusively or mainly on members of the opposite sex or gender identity. Lesbian (adj., noun) – A sexual orientation that describes a woman who is emotionally and sexually attracted to other women. Pansexual or Omnisexual (adj.) – A sexual orientation that describes a person who is sexually and emotionally attracted to people of any sex or gender identity. Pansexual people may refer to themselves as gender-blind, asserting that gender and sex are insignificant or irrelevant in determining whether they will be sexually attracted to others. Gender Identity Terms Bigender or Binary (adj.) – Describes a person whose gender identity is a combination of two genders. Cisgender (adj.) – A person whose gender identity aligns with the assigned sex at birth or biological sex. Gender non-conforming (adj.) – Describes a gender expression that differs from a given society’s norms for males and females. Gender transition (noun) - The process by which some people strive to more closely align their internal knowledge of gender with its outward appearance. Some people socially transition, whereby they might begin dressing, using names and pronouns and/or be socially recognized as another gender. Others undergo physical transitions in which they modify their bodies through medical interventions. Intersex (adj.) - A variation in sex characteristics including chromosomes, gonads, or genitals that do not allow an individual to be distinctly identified as male or female. Non-binary Alternate terms are gender queer and gender non-conforming. Transgender (adj.) – Describes a person whose gender identity and assigned sex at birth do not correspond. Also used as an umbrella term to include gender identities outside of male and female. Sometimes abbreviated as trans. SOGI Awareness Again, not all people use the above terms in the same way, so respect and sensitivity are key. And the healthcare setting is an especially vulnerable one. Maintaining the dignity and humanity of every individual during a medical interaction is essential. The U.S. Department of Health and Human Services requires all Electronic Health Record (EHR) systems be able to collect SOGI information from patients. This promotes better understanding of health treatment outcome disparities in order to reduce them. Renown Health’s mission is to make a genuine difference in the health and well-being of the people and communities we serve.
-
11 Tips Caregivers Need to Know
Becoming a caregiver or playing a more active role in another’s healthcare is a big responsibility. At some point, almost all adults will support an aging parent or a loved one in need. Keeping track of their needs and wellbeing, while also prioritizing your own can become overwhelming. It’s important to know: you are not alone, and help is available. Read on for 11 tips to help you manage your time, your own wellbeing and your loved one’s care. Self-care comes first. When your main priority is the person in your life who needs care, it’s easy for your own needs to take the backseat. Give yourself time each day to focus on your personal wellbeing. It’s hard to give a loved one the care they need if your own needs are not met. Prioritize the Activities of Daily Living (ADL). Make a note of what ADLs your loved one can do alone, what they need help with and what activities require the most help. This will help you work through the day with them, as well as plan out how the day’s activities will go. Do a home safety audit. Do showers, bathtubs and steps have safety grab bars? Look around the house for additional tripping hazards, like rugs or electrical cords. If your loved one struggles with day-to-day navigation of the home, consider scheduling an occupational therapy appointment. This type of therapy helps a person develop or maintain the motions required to accomplish daily tasks. You might also qualify for a referral to in-home healthcare, such as Home Care. Have the hard conversation. The best time to discuss views about end of life care and to learn what choices are available is before a life-limiting illness or crisis occurs. With advance care planning, you can help reduce the doubt and anxiety related to decision making at the end of life. Completing an Advance Directive is a great tool to sort out all these decisions before they’re needed. Attend a free workshop to learn more and complete this important document. Identify when you need respite. Respite care involves receiving a short-term break from caregiving. Organizing in-home care for your loved one will allow you to step away and tend to your needs. By identifying what kind of respite care you are seeking, you can find the right person to provide you with that much-needed break. Don’t wait until you feel overwhelmed, plan ahead. Write down insurance contact information. Have a direct connection to the right insurance professional for support and advice. If your loved one is eligible Medicare, this is a good opportunity to review their current selections and if they would benefit from a Medicare Advantage Plan or Medicare Supplement Insurance. Seeking out expert advice or information on Medicare options is a great way to navigate this. Consider calling a broker, or attend a free educational seminar with Senior Care Plus. Gather legal and financial information. Make a list of all existing legal documents and financial accounts that your loved one has. These might include a will, advance directive, power of attorney, bank accounts or investment accounts. If you have questions about how to manage them, or need assistance in setting up additional framework, reach out to a lawyer, legal service, financial adviser or bank representative. Create an inventory of medical information. Identify where all of your loved one’s medical records are, as well as a list of providers or healthcare practices where they have received care. Consider if you should have your loved one give you Proxy Access in MyChart, which allows you to access all the features in MyChart on their behalf, including viewing upcoming appointments, viewing test results and emailing a doctor on their behalf. Make a list of what others can do. Think about all the little (and big) things that need to happen, and write down tasks that others could take care of you. When someone says “let me know what I can do” you’ll be ready with a pre-written list of items they may be able to assist with. Tasks could include tackling around-the-house repairs, scheduling lawn work, helping to walk the dog, taking a car for an oil change and cleaning. Find programs and events for social enjoyment. If and when possible, seek an activity outside of the home. Look for community centers that have programs for seniors, recreational activities or meals that you can patriciate in together. If leaving the home is not an option, arrange for visits or in-home activities, such as movie nights, card games or time to visit with family. Research long-term options. If you will be considering a nursing home or assisted living, make a list of amenities that you and the person you are caring for would like. Take this list with you when visiting potential locations to make sure you don’t forget to ask about each item.
-
Cancer Nutrition - Helpful Tips to Support Your Loved One to Eat Healthy
Eating healthy is a daily challenge for many, but for those with cancer it is an even harder struggle. A cancer diagnosis not only impacts those diagnosed, but family members and friends too. One key area of concern is making sure your loved one stays well by eating healthy food every day. Here are some essential cancer nutrition tips from Renown Health registered dietitians Jessica Blauenstein and Amy Laster. Help to Prepare Meals and Snacks for Daily Cancer Nutrition Make it grab and go. Easy-to-make meals help reduce the burden of having to cook and prepare food. Having easy to grab snacks on the counter or in the fridge can help ensure your loved one has access to those nutrients when needed. Sit outside of the kitchen. This allows your loved one to avoid cooking smells which can make them feel sick as a side effect of cancer treatments. Also try serving them cold foods such as sandwiches, cheese and crackers, or shakes which have a mild scent. Try drinkable meals. Some people with cancer find it easier to sip their calories over the course of 30 minutes to an hour. Consider smoothies or supplemental shakes such as Ensure Enlive or Boost Plus as snacks not meal replacements. A great foundation for a smoothie is a protein source (Greek yogurt, protein powder, nut butters or milk) with a carbohydrate (fruits, juice or berries). Add other ingredients as desired, such as spinach, kale, and ground flaxseed or chia seeds to give it more vitamins, minerals, and fiber. Snack Ideas for Those Undergoing Cancer Treatment The following ideas are both quick and easy to make for your loved one. Chicken or tuna salad with whole grain crackers or as a sandwich on whole grain bread Greek yogurt mixed with cereal, fruit and/or nuts Cottage cheese with banana, cinnamon and/or peanut butter Favorite fruit with 100% natural peanut or almond butter spread - Try peanut butter with bananas, apples, or even celery Their favorite veggies dipped in a salad dressing of your choice - For example, carrots with hummus or ranch dressing Cheese and whole grain crackers - Add tomato slices with a dash of oregano on top for more flavor Eggs scrambled with cheese, vegetables and/or salsa Peanut butter and jelly sandwich on whole grain bread A baked sweet potato with some favorite toppings Hard boiled eggs and/or egg salad with whole grain crackers, or as a sandwich on whole grain bread Oatmeal or cream of wheat prepared with milk, fruit and/or nuts Sometimes your loved one may not feel like eating or refuse to eat. If treatment side effects are impacting your loved one’s ability to eat, please visit the websites below containing recipes tailored to treat side effects. Cook for Your Life ELLICSR Of course you may also consult a registered dietitian and/or the patients care team, if you have more cancer nutrition concerns. No Appetite? Assisting with Cancer Taste Changes Taste changes are common during cancer treatment. Patients experiencing these changes may not feel like eating, which can negatively impact their nutrition. Help your loved one overcome taste changes with these cancer nutrition strategies: Metallic or bitter taste in food - add something sweet such as maple syrup, honey or jelly. You may also try adding fat, such as a nut butter, avocado or regular butter. Pickles or vinegar could help with this too. A taste like cardboard - try adding salt and extra flavor to foods with seasonings and spices. Some examples are onion, garlic, chili powder, basil, oregano, rosemary, tarragon, barbecue sauce, mustard, ketchup, or mint. Lemon juice, citrus, vinegar, or pickles may also help with this as well Food tastes too sweet - try adding six drops of lemon or lime juice. Add small amounts until the sweetness is gone. Very salty taste - try adding ¼ teaspoon of lemon juice. Try plastic utensils instead of metal, especially if your loved one is struggling with foods tasting metallic. Dipping small bites of food into either lemon juice or vinegar can have a “palate cleansing” feel and may improve taste perception. This helps avoid getting tired of the flavor after a few bites. Try marinating food or meats in sweet fruit juices, salad dressings, or sweet-and-sour sauce. Other “palate cleansing” foods are lime juice, orange juice, mangos, lemongrass, parsley, cilantro, mint, ginger, basil, and pickled foods. Use aroma to make foods appealing, avoiding any smells that may cause nausea. In particular, cinnamon, nutmeg, cloves, coriander, cumin, ginger, and black pepper can add an aromatic flavor. Also include herbs such as oregano, rosemary and thyme. Think texture. Consider trying wafers, crunchy nut butters, carrots, celery, cucumbers, chips, rice crispies, corn flakes, crackers, panko crumbs, nuts, or seeds if you are able to chew and swallow them safely. Remember that patience with your loved one's changing appetite and tastes can be the strongest form of support you can provide. Nutrition Tips for Cancer Survivorship and Beyond If eating large meals is difficult for your loved one, encourage them to snack throughout the day. Aim for 4-6 snacks or small meals per day. Focus on consuming 2-3 protein-rich foods each day such as lean animal meats, fish, eggs, soy or a protein supplement with 20-30 grams of protein per serving. Eat a variety of brightly colored fruits and veggies. Aim to make half of each meal fruits and vegetables. Eat less than 18 oz. (cooked weight) of red meat per week. Limit cold cuts, bacon, sausage, and hot dogs. Avoid excess salt and saturated fats. Cut back on simple carbs. (i.e. desserts, candies, white bread/pastas, french fries, packaged foods, chips) Drink in moderation- if at all- one drink per day for women, two for men. Get enough vitamin D (through diet and/or supplement) Avoid tobacco of any kind. Keep a healthy weight and stay up on exercise. Other Ways to Help a Loved One with Cancer Assist with Chores Allow your loved one to relax as you help take care of chores around the house, such as cleaning, cooking and grocery shopping. This may reduce overall stress and can be helpful for those that get tired after their treatments. Physical activity can still be beneficial, so be sure to do an activity together that they enjoy and is approved by their doctor. Be Patient It can be very difficult to see a loved one go through cancer treatment. Remember to be patient with your loved one. There may be things we want them to do or eat that we know would be good for them, however, meet your loved one with grace and understanding. It is ultimately their decision on what to do, just be there to support and assist them as they go through this challenging time. Additionally, Renown hosts free “Eating Well After Cancer Treatment” nutrition classes for cancer survivors. Our next cancer nutrition class series starts Thursday, June 3, 2021, and will be hosted virtually. It is open to anyone in the community. For more information or to register please click here.
Read More About Cancer Nutrition - Helpful Tips to Support Your Loved One to Eat Healthy
-
COVID-19 Booster Shots, What You Need to Know
Getting the COVID-19 booster is the best way to protect yourself from severe illness or death due to COVID-19, and both the CDC and the FDA have approved booster shots for people ages 18 and older. So, with the holidays right around the corner and infection rates on the rise both in Nevada and nationally, the best thing you can do to prevent the continued spread of this deadly virus is to get boosted today. The Basics: Who: It is recommended that everyone 18 years or older get a COVID-19 booster shot. When: At least 6 months after completing your primary COVID-19 vaccination series. What: Any of the COVID-19 vaccines authorized in the United States. The CDC allows for mix and match dosing for booster shots. How: To make an appointment for your COVID-19 vaccine booster, please visit vaccines.gov today. Appointment Reminders: Don’t forget to bring your CDC vaccination record card to your appointment. Refresh yourself on the potential side effects and remember that these are normal signs your body is building up protection. Commonly Asked Questions: Q: Does anything change if I received the Johnson & Johnson as my first COVID-19 vaccine? A: If you received the Johnson & Johnson COVID-19 vaccine, you are elidable for a booster two months after completing your primary vaccine. Q: Is the formula the same for the boosters as it was for the primary vaccine? A: COVID-19 booster shots are the same formulation as the current COVID-19 vaccines. However, in the case of the Moderna COVID-19 vaccine booster shot, it is half the dose of the vaccine people get for their primary series. Q: Am I still considered “fully vaccinated” if I don’t receive a COVID-19 booster shot. A: Yes, everyone is still considered fully vaccinated two weeks after their second dose in a two-shot series, such as the Pfizer-BioNTech or Moderna vaccines, or two weeks after a single-dose vaccine, such as the J&J/Janssen vaccine. All information courtesy of the Center for Disease Control and Prevention. All information courtesy of the Center for Disease Control and Prevention
Read More About COVID-19 Booster Shots, What You Need to Know
-
Fall Recovery Gets Patient Back to Life and Movement
Standing at the top of the stairs to the basement Sharon Sturtevant was chatting with her grandson in the kitchen. Suddenly, Sharon stumbled and fell down the stairs. “The last thing I remember was my head hitting the floor before everything went black,” she recalls. Her grandson, Oliver, quickly called 911 and paramedics arrived on the scene, taking her by ambulance to Renown Regional Medical Center where she was diagnosed with a broken collarbone and a neck fracture that would require complex surgery involving fusion of her neck. Fall Recovery Begins After her surgery, Sharon was transported to the Renown Rehabilitation Hospital and her recovery process began. Sharon smiles as she describes the rehab hospital team “They are fabulous here, I learned so much about how my body moves, and the proper way to move it. At home I wouldn’t have known what to do,” she confesses. “They set me up for success to return home and not get injured again.” At Renown Rehabilitation Hospital, different therapists coordinated a custom plan to help Sharon recover from her injuries. Ultimately, the goal of her physical therapy was to help restore and improve her strength, reduce pain and increase her mobility for stamina and balance. Physical Therapy Key to Successful Treatment of Falls “My recovery after the operation was an eye-opener,” Sharon declares. “I had no idea how much went into regaining everyday moment.” During her rehabilitation hospital stay, she had to re-learn how to swallow, go up and down stairs, as well as successfully get in and out of a wheelchair, which involved transferring her body weight safely. Due to hormonal changes after menopause women are 50% more at risk for falls than men, according to research. Sharon now has a greater awareness of how to move her body and is significantly stronger than before entering her physical rehabilitation sessions. Not everyone knows that everyday mobility is impacted by four basic skills: stepping, trunk flexibility, upright posture and weight shifting. “I don’t know how I could have gotten this far without the wonderful therapists here,” she shares. “They are so thorough. Proper alignment was encouraged helping me to walk and stand correctly. They were all so nice and patient with me,” she states. “I actually had less pain because I didn’t hurt myself moving the wrong way.” Falls Are Common Among Aging Adults As we age balance becomes more important. Unfortunately falls are common among older adults with negative quality of life effects, even fatalities. According to the Centers for Disease Control and Prevention (CDC), one in four seniors fall each year in the U.S. A comprehensive physical therapy plan for sudden falls or chronic conditions is a safe, effective alternative treatment to medication such as opioids. Today Sharon is back at home with a new banister installed on the basement stairs. As a music lover she is enjoying her musical grandchildren Oliver and Eliana who play instruments. She looks forward to attending their upcoming school concerts. Sharon remembers the staff at Renown Rehabilitation Hospital fondly, “They were unfailingly patient, supportive, informative and understanding.” Her advice to those unexpectedly finding themselves in the rehabilitation hospital is, “Listen to your therapists carefully and follow their instructions.”
Read More About Fall Recovery Gets Patient Back to Life and Movement
-
Pharmacists Answer Questions about the COVID-19 Vaccines
Vaccines that provide protection against the COVID-19 virus are bringing us closer to the end of this deadly pandemic. Two different COVID-19 vaccines are currently available in the U.S. today: one from Pfizer and the other from Moderna. Kate Ward, PharmD, BCPS, Director of Clinical Pharmacy at Renown Health and Adam Porath, PharmD, Vice President of Pharmacy at Renown, share what you need to know about these vaccines. When two COVID-19 vaccines were approved by the U.S. Food & Drug Administration (FDA) in December 2020, it was cause for celebration. Why? Because according to the CDC, the vaccines are 94 percent or more effective in providing protection against the COVID-19 virus! Many people are seeking information about the new Moderna and Pfizer vaccines. Below, our pharmacy leaders provide answers to some commonly asked questions. How do the COVID-19 Vaccines Work? The Pfizer and Moderna vaccines are both mRNA vaccines that help your immune system develop antibodies against the COVID-19 virus. The vaccines use messenger RNA, or mRNA, to show our bodies’ protein-making cells how to make the spike proteins of the COVID-19 virus. Our immune system reacts to these spike proteins by creating antibodies that can recognize and destroy them. So when a person is exposed to the virus in the future, they will be less likely to get sick. What are the Differences between the Pfizer and Moderna Vaccines? The Pfizer and Moderna COVID-19 vaccines are very similar, with just a few small differences worth noting. The main difference between the two vaccines is when you should receive your follow-up dose. Patients who receive a first dose of Pfizer should receive their second dose about three weeks later. Those who receive a first dose of Moderna should receive their follow-up vaccination roughly four weeks after their first dose. People 18 years and older can receive the Moderna vaccine while people 16 years and older can receive the Pfizer vaccine. Dosage for the Moderna vaccine is 0.5 ml (100 mcg). Dosage for the Pfizer vaccine is 0.3 ml (30 mcg).
Read More About Pharmacists Answer Questions about the COVID-19 Vaccines
-
Reno Widow Inspires New Visitor Policy for Renown
Renown Health is one of the country’s first health systems to lift visitor restrictions for patients with COVID-19 and encourage the family to be at the patient’s bedside. Read Darlene and Dave’s story to understand why we’re updating our visitor policy. Dave and Darlene Randolph found joy in exploring antique shops and garage sales to find damaged or discarded vintage pieces. Dave would spend many hours scraping, cleaning, sanding, and refinishing items, transforming them into functional, beautiful pieces of furniture. Every piece in their home rekindles a memory and has a story to tell. On Thanksgiving, when Dave was too ill to gather around their antique dining room table, Darlene called the ambulance. Ailing with COVID-19 for two weeks, Dave had not been improving. When the EMTs reached her home and asked Darlene what underlying conditions he had, she said, “all of them.” David was seriously ill. Hospitalized for COVID-19, their communications options were limited. The only way Darlene could communicate with Dave was on a video call or by telephone. Dave spent 17 days hospitalized at Renown Regional Medical Center in Reno. Darlene spent 17 days waiting by the phone for more information on his condition. Darlene said he had “up days and down days,” but thought he might be home, sitting at their antique dinner table for Christmas. Sadly, Dr. David Randolph lost his battle with COVID-19 on December 13, 2020, and died as he slept in a hospital bed. When Darlene wrote his obituary for the newspaper, she gave thanks to the “tremendous nurses and doctors at Renown Regional Medical Center, for providing his care during a time when the family could not be with him.” Taking Action to Inspire Change Darlene wished she could have been there. Over their 45-year marriage, she had always been there. Darlene said, “I had always been at his bedside, as his advocate, to help communicate and straighten things out.” As a registered dietician, she worked in hospitals, knew the protocol, and knew that Renown had a restricted visitor policy to stop the virus’s spread- to other patients, staff, and their family members. Still, she wished she could have spent more time with him. On Christmas Eve, she sat down and wrote to Renown leadership. “As the wife of a COVID patient who recently passed away in your hospital, I want to express my thanks to you and your staff for the care he received in the last days of his life. I am aware that the nurses and staff are working under dangerous conditions and risking their health and lives by caring for multiple COVID patients. The staff is gracious, concerned, and doing everything they can.” She continued, “I know procedures are changing every hour to try to stay ahead of this dangerous virus, and I am sharing my experiences, hoping they will be helpful when establishing policies that impact families.” Darlene explained that despite receiving assurances that Dave’s nurse or a doctor would call daily, sometimes they would forget. She explains in her letter, “how important it is, in these times when the family cannot visit, and has only infrequent communication and is anxiously waiting at home for information about their loved one, how much it means to get a call from someone caring for him at the hospital. If there is a way you can help assure nurses have time to make calls or assist patients in making calls because it is an important part of patient care.” A Person-Centered Visitor Policy After receiving her letter, Renown leadership called Mrs. David Randolph to thank her, offer his sympathies and ask if Renown could help in any way. Darlene asked if he might reconsider allowing families to visit hospital patients during treatment for COVID-19. As the COVID-19 situation has evolved, the policy has as well. Renown hospitals and medical practices now encourage limited visitors for all patients, including those diagnosed with COVID-19. Renown also has extra safety measures to protect the health of patients, visitors and healthcare employees. Darlene is very pleased that her letter inspired this shift in visitor policies for patients with COVID-19. She says, “I have always tried to think of ways I could help other families. Especially those senior couples where one has been hospitalized and the other is home. My wish is to help others.” Renown Health Visitor Policy Renown Health patients may identify two healthy adult “patient supporters” to accompany them on their hospital stay. For more details, visit our Patient Supporter Guidelines page.
Read More About Reno Widow Inspires New Visitor Policy for Renown
-
COVID-19 Vaccine Expert Advice
With front-line workers receiving the first COVID-19 vaccinations, many of us are feeling hope, but also worry. As a result, we are joining with the Ad Council, the COVID Collaborative, HHS, CDC and NIAID (along with top health and medical organizations) to address your vaccine concerns and questions. Will the vaccine be available to everyone in Nevada? The Nevada Department of Health and Human Services (DHHS) is collaborating with health systems about the use of initially available, limited supplies of COVID-19 vaccines. They will provide guidance on the prioritization order of who will receive the vaccine. This will be based on available quantities, high-risk locations of work and certain other risk factors, and recommendations and guidance for public health agencies. The CDC has provided guidance to initially focus on the following groups: Healthcare personnel likely to be exposed to or treat people with COVID-19, nursing home residents and others in institutional settings; People at risk for severe illness from COVID-19 due to underlying medical conditions; People 65 years of age and older; Other essential workers. I worry the vaccine has been rushed The U.S. national vaccine safety system ensures that all vaccines are as safe as possible, and because vaccines are given to millions of healthy people to prevent serious diseases, they’re held to very high safety standards. COVID-19 vaccines are undergoing a rigorous development process that includes vaccinating tens of thousands of people who participate in a study to generate the needed clinical data. These clinical trials generate scientific data for the FDA to determine the safety and efficacy of each vaccine. It’s worth noting that the clinical studies to establish the safety and efficacy of the Covid-19 vaccines were as big and thorough as recent studies for other licensed vaccines (for example, the shingles vaccine). I'm concerned about the vaccine's side effects The most common side effects are very similar to those seen with most vaccines, such as: sore arms, fevers, and tiredness within 72 hours after the vaccine. These side effects usually mean that the vaccine is generating an immune response, indicating it is working. Short-term side effects observed in the leading COVID-19 vaccine trials include: Injection site pain and redness Fatigue Muscle aches and pains Joint pain Headache I’m afraid I’ll get COVID-19 from the vaccine None of the authorized and recommended COVID-19 vaccines, or COVID-19 vaccines currently in development in the United States, contain the live virus that causes COVID-19. This means that a COVID-19 vaccine cannot make you sick with COVID-19. Can children receive the COVID-19 vaccine? Not at the moment. In early clinical trials for various COVID-19 vaccines, only non-pregnant adults at least 18 years of age participated. However, clinical trials continue to expand those recruited to participate. The groups recommended to receive the vaccines could change in the future. As of now, it is recommended that children do not receive the vaccine. More information will be available from the vaccine manufacturers. I do not believe vaccines are effective Both this disease and the vaccine are new. We don’t know how long protection lasts for those who get infected or those who are vaccinated. What we do know is that COVID-19 has caused very serious illness and death for a lot of people. If you get COVID-19, you also risk giving it to loved ones who may get very sick. Getting a COVID-19 vaccine is a safer choice. The FDA is responsible for making sure that, just like any other medications, any FDA-authorized or approved COVID-19 vaccines are safe and they work. The EUA (Emergency Use Authorization) will not be provided if the FDA feels that the vaccine is unsafe. I can't get vaccines to due to a medical condition Adults of any age with certain underlying medical conditions are at increased risk for severe illness from the virus that causes COVID-19. mRNA COVID-19 vaccines may be administered to people with underlying medical conditions provided they have not had a severe allergic reaction to any of the ingredients in the vaccine. The following information aims to help people in the groups listed below make an informed decision about receiving the mRNA COVID-19 vaccine. It is extremely important to speak with your doctor regarding your specific medical condition, and always follow their strict advice regarding the COVID-19 vaccine, or any other vaccines. Sources: Renown COVID-19 Ad Council COVID Collaborative U.S. Department of Health & Human Services Centers for Disease Control and Prevention National Institute of Allergy and Infectious Disease
-
Don’t Put Your Bladder Health on Hold
Millions suffer from urinary incontinence (urine leakage). Often people feel as if their bladders control their lives. But this doesn't have to be your story. Bladder control issues are treatable and you can take steps to help control your bladder. What is urinary incontinence? Men and women of all ages can have difficulty controlling their bladders. Urinary incontinence occurs when the muscles in the bladder that control the flow of urine contract or relax involuntarily. Is there more than one type of urinary incontinence? Yes, there are three main types: Stress incontinence is when the bladder leaks small amounts of urine as a result of physical stress or pressure on the muscles supporting the bladder caused by coughing, sneezing, laughing, lifting or any sudden physical exercise such as running or jumping. Urge incontinence is the inability to control a strong urge to go without advance warning, limiting the time needed to get to the bathroom. Overflow incontinence occurs when the bladder does not empty properly. As a result, over time, large quantities of urine are stored, causing the bladder to overflow (this is more common in men and is often the result of an enlarged prostate blocking the bladder opening). Are there any tests that can determine the cause and type of incontinence? Your doctor may have you track your fluid intake and output in a Bladder Diary. A urinalysis can be checked for infection, traces of blood, or other abnormalities. Blood tests can look for chemicals or substances that may relate to contributing causes. Other testing may be an ultrasound, cystogram or post voiding residual measurement. How is urinary incontinence treated? Exercises to strengthen the pelvic floor muscles or restrain the bladder to hold on for longer. Medication can relieve and control the troublesome symptoms. If there is an infection an antibiotic is used. Surgery can repair weakened muscles or remove blockage. Special products such as pants, pads, collection devices, and chair and bed protection may be needed if the problem cannot be controlled. How do you strengthen your pelvic floor muscles? To make your pelvic floor muscles stronger, alternate between squeezing and relaxing them. Following the steps below may help: Squeeze your muscles for one second and hold. Relax your muscles for two seconds. Each time you squeeze and relax, it counts as one set. Complete five sets. When you can do the exercises easily, increase to doing them 10 times per day. When that gets easy, try to squeeze and hold the muscles for three seconds and then relax the muscles for three seconds. As your pelvic muscles get stronger, you can progress to longer squeezes for about 10 seconds. Be sure to relax between squeezes so that your muscles can rest before squeezing again. You should do these exercises in three different positions. Do 10 sets lying down, 10 sitting and 10 standing. It is important that you develop the habit of doing the exercises every day. You may want to exercise just after you get up in the morning and right before you go to bed at night. What can I do to help control incontinence? Watch your weight, practice pelvic floor muscle exercises, eat plenty of fresh fruits, vegetables and fiber to prevent constipation. Most importantly, talk to your doctor regarding incontinence issues, don’t be embarrassed!
-
Your 9-Step Guide to Prevent Falls
According to the Centers for Disease Control and Prevention (CDC), one out of four adults aged 65 or older, fall each year. But less than half of those who fall talk to their healthcare provider about it. What’s more, among older adults, falls are the leading cause of both fatal and nonfatal injuries. Senior Care Plus, a Medicare Advantage Plan by Hometown Health, and Renown Health Nurse Educator, Nicholas Mannering, worked together to provide a list with simple tips to help you prevent falls. 1. Exercise Exercise strengthens both your muscles and bones and improves balance which is a key factor to preventing falls. The stronger you are, the less likely you are to fall. And, if you do fall, you are less likely to be injured. 2. Vision Check Vision is an import part of fall prevention, have your eyes check by an eye doctor at least once a year. Update your vision prescription and replace your eyeglasses as needed. 3. Install Safety Equipment in Your Bathroom Installing grab bars in your home bathroom provides a way for you to help yourself in and out of challenging situations. It also provides support if you suddenly feel week or unstable. Having a grab bar to lean on or hold onto when you feel yourself falling or slipping can help prevent falls. Rubber mats eliminate slick surfaces that increase your risk of falling. 4. Helpful Items in Your Bedroom A light within reaching distance is an important item to have in your bedroom. One reason adults fall is because they wander through a dark room, often to get to the bathroom at night, and can’t see where they are walking. Having a light within reach that is quick and easy to turn on before walking around a room can make it safer and decrease your risk of falling. Having a bedroom that is organized and furnished in a way that is easy to navigate is also important. If your bedroom is cluttered and hard to walk around without tripping or running into things, it might be worth reorganizing the area to define a clear walking path. 5. Helpful Items in Your Living Room Similar to your bedroom, your living room should have a light that is easily accessible. Sofas with armrests are helpful for support when getting up and sitting down. Avoiding clutter in your walkways, rugs that are not secured down and unstable furniture are important to consider when preventing falls. 6. Actions to Avoid in Your Home There are other ways to fall besides slipping or tripping while walking. Never stand on chairs, boxes or other unstable items in your home. Walkways should be tidy and free of objects that you could trip on. Spills should be cleaned up right away to prevent slipping. 7. Wear Appropriate Footwear Wearing shoes with non-slip soles and closed toes can help prevent you from falling. Having shoes that fit properly, are made from hard rubber (like tennis shoes) and provide good support help prevent tripping and falling. Shoes with a collar that support the ankle and a well-padded tongue for the top of your foot can also help prevent injury to your feet. 8. Review Your Health & Medications at your Annual Health Check-Up It is important to review your health and medications with your healthcare provider so they can assess if you are at risk for falls. You should discuss your vision, heart health and blood pressure at your annual health check-up. These things can play a role in the risk of falling. Reviewing your current medications is also important. If medications are making you dizzy, talk to your provider about adjusting the dosage so you can feel more stable and balanced. When talking to your doctor about medications be sure to include your vitamins and supplements. Finally, Have your healthcare provider check your feet and discuss proper footwear yearly. 9. Avoid Smoking and Alcohol Balance is important in preventing falls. Alcohol consumption negatively affects balance and increases your risk for falls and fractures. It also increases your risk for cancer, liver damage, osteoporosis, high blood pressure and strokes. Smoking is connected to frailty in older adults. It prevents the development of muscle tissue and breaks down healthy muscle tissue due to the lack of oxygen in your body.
-
Monkeypox: A Renown Expert Weighs In
Renown Health is closely following the national outbreak of the monkeypox virus and urging healthcare providers to be alert for patients with illnesses associated with a rash. In working with the Washoe County Health District (WCHD), Renown is closely monitoring the spread of monkeypox in the community and looking to prevent and reduce the spread of monkeypox. To help to ease worries, we consulted with Paul De Leon, Infection Preventionist at Renown Health. What Exactly is Monkeypox? Monkeypox is a rare viral illness caused by the monkeypox virus — the same family of viruses that causes Smallpox. Although symptoms are similar to Smallpox, monkeypox symptoms are milder and rarely fatal. However, it's important to mention that this virus can be more severe for these susceptible groups: Immunocompromised Pregnant women A fetus or newborn baby Women who are breastfeeding Young children Those with severe skin diseases such as eczema How is Monkeypox Transmitted? The monkeypox virus is not easily transmitted but occurs through sustained person to person close contact with an infected individual. Monkeypox can also be transmitted through direct contact with infectious rash, scabs, or body fluids. Monkeypox can also be spread through prolonged intimate physical contact, such as kissing, cuddling or sex. Lastly, monkeypox can be spread through contaminated linens or bedding. Transmission through respiratory secretions is uncommon but has been reported after prolonged face-to-face contact with symptomatic individuals. In addition, pregnant women can spread the virus to their fetuses through the placenta. Monkeypox Testing If you think you have monkeypox, contact your primary care physician or other medical providers to obtain testing. Notify the provider ahead of time before entering the physical office. Signs & Symptoms This current outbreak of West African monkeypox does not have the typical presentation of classic monkeypox. Symptoms usually appear one to three weeks after infection and include: Pimple-like rash or blisters on the face, inside the mouth, and on other areas of the body, like the hands, feet, chest, genitals, or anus. The rash will go through serval stages, including scabs, before healing and may be painful or itchy. Other symptoms of monkeypox can include: Fever Headache Muscle aches and backache Swollen lymph nodes Chills Exhaustion Respiratory symptoms such as sore throat, nasal congestion, or cough Symptoms of monkeypox may occur before or after a rash with some individuals only report experience a rash. Individuals with monkeypox are infectious once symptoms begin and remain infectious until lesions form scabs, scabs fall off, and a fresh layer of skin forms. The illness typically lasts 2-4 weeks.
-
Avoid Counterfeits and Find the Right Protective Mask with This Helpful Guide
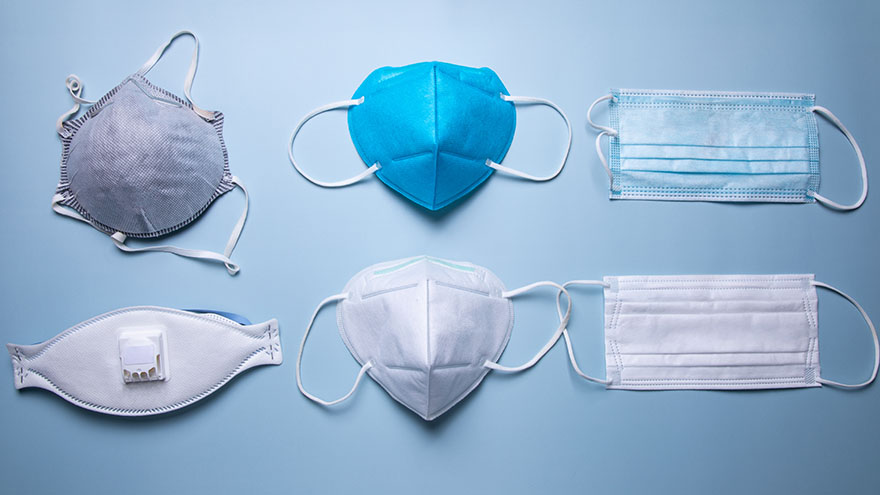
To better protect our patients, visitors and employees, cloth masks are no longer allowed at Renown facilities. Surgical masks, KN95 and N95 masks are allowed at Renown facilities. Appropriate face masks will be provided for visitors and patients who need one. With recent surges in the infectious COVID-19 omicron variant, many have sought to upgrade their face masks. But, let’s face it, shopping for face masks with adequate protection can be a challenge, especially considering the countless variations and the rise of counterfeit masks. Follow our straightforward guide below which includes some common red flags to help you discern between a high-quality face mask that provides proper protection and those that may be counterfeit. Types of Masks Qualities of a Real N95 Respirator Mask According to the National Institute for Occupational Safety and Health (NIOSH), N95 approved masks form a tight seal around your face and include a disposable respirator that removes particles including bacteria, viruses and dust as you breathe. N95 masks that are NIOSH approved undergo strict quality assurance and performance requirements to ensure mask respirators filter out up to 95% of hazardous particles. As a rule of thumb, N95 masks will not have ear loops, commonly used in cloth or surgical face masks. N95 respirators will contain two elastic bands or head straps that fasten behind the head, one securing the crown of the head and the other resting at the base of the neck, providing a snug fit and seal. Some other common signs that an N95 might be counterfeit include lack of all proper labeling, misspellings of NIOSH, decorative fabric and claiming to be approved for children. Currently, masks in adult sizes are the only masks to undergo NIOSH’s quality assurance and testing process. Respirators approved by NIOSH will include a testing certification (TC) approval number and will contain specific labeling on the facepiece of your mask. Find a full list of Center for Disease Control (CDC) and NIOSH requirements here. Identifying Real KN95 Respirator Masks Often preferred due to comfortability, the KN95 respirators were initially designed to meet Chinese standards for medical masks. Firstly, if a KN95 mask claims to be approved by the CDC, it is counterfeit as the CDC and NIOSH do not support any respiratory protective devices according to international standards. However, when KN95 masks are fitted and worn appropriately they do provide more protection than disposable masks. Legitimate KN95 masks will display a manufacturer number, GB2626-2019, ensuring accordance with current Chinese respirator standards for all masks made after July 1, 2021. Unlike N95 masks, it is important to note that KN95 masks are available in children's sizes. You might run into KN95 masks claiming to be “FDA (Food and Drug Administration) approved” or “FDA-registered,” but be aware that this does not mean much and is a misleading statement. What this indicates is that a mask maker has submitted paperwork to the FDA, but the product has not been thoroughly tested for proper filtration and protection. Surgical Masks Medical procedure masks often referred to as surgical or disposable masks vary in their protection according to a variety of factors including fit and filtration. The CDC defines medical procedure masks as “variably shaped, including flat pleated, cone-shaped, or duck-bill. Medical procedure masks are loose and are not expected to provide a reliable level of protection against airborne or aerosolized particles as N95 respirators regulated by the National Institute of for Occupational Safety and Health.” However, these types of masks provide more protection than cloth masks and are certainly better than wearing no mask at all. Often popular due to their level of comfort and cost-effectiveness, surgical masks can be knotted in the ear loop areas to provide a tighter seal and can be layered for additional filtration. Depending upon your budget and level of comfortability and protection, one variation of mask may suit you over another. Please remember to do your part in limiting the spread of COVID-19 and wear a surgical mask, KN95 or N95 mask when visiting Renown facilities.
Read More About Avoid Counterfeits and Find the Right Protective Mask with This Helpful Guide