Search
-
Stroke Survival as a Warrior – Kimi's Story
It seemed like a normal Wednesday, except Kimi Woolsey was feeling really stressed. On Sept. 4, 2019 she was rushing to get ready for an appointment when suddenly, she could not feel her legs. Kimi immediately knew something was wrong and called out to her fiancé, Paul, for help. After seeing a bright light in her right eye, she felt a severe, sharp pain in her head traveling down into her leg. Paul quickly called 911, the EMT’s arrived and her stroke survival journey began. At first the medical team thought she had a complicated migraine, but one of them suspected a stroke. On the way to the hospital Kimi felt numbness and her face drooping, then instantly, no pain. For a moment she thought she was dying, going from pain to numbness and realizing she couldn’t move or speak. Kimi didn’t know she was having another massive stroke in transit. Each year nearly 800,000 people in the U.S. suffer a stroke, or “brain attack” – that’s one every 40 seconds. Of those, about 75% occur in people over age 65. However, at only 45 years old, Kimi is proof that a stroke can happen at any age. Stroke Survival Begins for Kimi Upon arriving at the emergency department of Renown Regional Medical Center the Certified Comprehensive Stroke Center team went into action. Kimi received a brain MRI, then was wheeled into surgery for a thrombectomy (clot removal). She was in the intensive care unit for 11 days. She remembers someone telling her, “Generally people don’t survive this magnitude of stroke.” And a doctor saying, “You are here for a reason.” Kimi’s comeback journey began with the comprehensive care team at Renown Rehabilitation Hospital. “Literally I had the best day of my life that first day there…I was so happy because I couldn’t imagine being in a safer place with people that literally live for you,” she recalls. During her 41 days there, her biggest milestone was being able to get out of bed and walk. For Kimi the support she felt at the rehab hospital was key to her progress, ”I still feel loved and appreciated and they’re rooting for me still and I can feel it.” Although she left the rehab hospital on Oct. 18, 2019, she is still working on improving the left side of her body. Currently Kimi works with therapists in outpatient physical rehabilitation sessions, continuing to see improvement in both her hand and leg. Her advice to those currently in a rehab hospital setting is, “Stay as long as you can to get the most out of it and push, push, push.” Kimi’s Stroke Survival as a Warrior “Having a stroke is not for the faint of heart,” says Kimi. She experienced despair and felt discouraged. Many days she would ask herself, “Why am I here?” Today she proudly calls herself a stroke warrior and refuses to be a victim of her stroke. Alongside her tenacious spirit, Kimi actively helps others on their stroke survival journey. Before her stroke she never dreamed of starting a non-profit foundation. Now, each day you’ll find her texting inspiration to others, offering advice and connecting with other struggling stroke survivors on her Facebook page, Stroke Warrior Recovery Coach. Her goal is to become the person she needed to talk to after her stroke; she currently coaches several stroke survivors. “Stroke survivors need to know that they aren’t alone. Mental support and encouragement are so important for each person’s stroke journey,” Kimi said. Along with the physical changes, Kimi feels the stroke magnified her empathy. “I was always in a hurry in my life. People didn’t go fast enough for me – on the road, at the grocery store, in a line. Now I have more patience with myself and others." Kimi realizes most people cannot wrap their brain around the concept of a stroke. In fact, the brain fog, physical challenges and frustration are hard to explain… unless you’ve experienced them. “You need to find your tribe,” she explains. “I have a passion for helping people through this process.” Most of all, she encourages people to keep going and never stop. After her stroke, Kimi has a greater appreciation for her family, health and life. She is one of the patients featured in the current “Fight The Good Fight” trauma and physical rehab advertising campaign. “I wake up every day and fight,” she asserts. “Each day you have to fight for your recovery and fight for yourself.”
-
Heart Attack Survivor Fights the Good Fight
Something wasn’t right. Even though it was the holiday season, on December 23, 2018, Mondo Corona didn’t feel good…not to mention his sudden earache. Although Christmas was a happy celebration with his family. He still felt tired. Was it the flu? And that darn earache wouldn’t go away. On that cool winter day, Mondo could not imagine he was near death. Or that he would become a heart attack survivor. Know Your Heart A few days later, on December 27, he wasn’t feeling any better. He decided to go to the emergency room at Renown Regional Medical Center. That’s when a simple blood test revealed shocking results. “I thought about death a lot. I was calling people to ask them to help take care of my family if I wasn’t going to be here anymore,” he emotionally confesses. Although Mondo loves his job as a railroad engineer, it involves on-call shifts and an erratic sleep schedule. At that time his exercise and eating habits weren’t the best either. Yet he never imagined he would have a massive, often lethal, type of heart attack called ‘the widowmaker.’ In fact, his family had been concerned about his health for awhile. “He worked so much and he didn’t take care of himself and he didn’t exercise – he was burning the candle at both ends,” shares his wife, Alison. His daughter Justice, an avid exerciser, was always encouraging him to join her at the gym, but could never quite convince him. Mondo remembers the time before he became a heart attack survivor. “I didn’t have any exercise whatsoever in my life. At that point my eating habits were just terrible,” he shares. He went to the emergency room due to his earache, but nothing was found until one of the doctors ordered some tests. Specifically blood work showed high troponin levels. Troponin is a blood protein often released in large amounts when the heart muscle has damage, sometimes by a heart attack. Heart Attack Survivor “My surgeon came in and told us that it was going to be a triple bypass – that three of the four…major arteries were clogged 100 percent,” Mondo explains. Amazingly his heart was pumping on only 10 percent blood flow. Heart surgeon, Joseph Brandl, MD, told him he survived a widowmaker heart attack. This type of heart attack happens when there is a 100 percent blockage in the critical left anterior descending artery (LAD) of the heart. Frequently the symptoms can often be mistaken for the flu. According to the Centers for Disease Control and Prevention (CDC), every 40 seconds a person in the U.S. has a heart attack. And 1 in 5 heart attacks are “silent” – meaning you can be a heart attack survivor, but not know it. For Mondo’s children, seeing their strong father struggle after heart surgery was difficult. Justice tearfully shares, “It was really hard seeing him so vulnerable. He really needed anybody’s and everybody’s help at that point.” A Heart Attack Survivor Program After leaving the hospital on January 5, 2019, he was extremely weak. On February 12, Mondo began Renown Health’s Intensive Cardiac Rehabilitation (ICR) Program called the Healthy Heart Program. This program, requiring a doctor referral, includes 12 weeks of supervised exercise along with nutrition education and stress management skills. In spite of heart disease being the leading cause of death in the U.S. – more than all cancers combined, the risk can be lessened with daily lifestyle habits. Mondo credits the ICR program with motivating him and getting his focus back on his health. He saw the team members setting an example and also caring about his health. He describes one of his favorite recipes, “In ICR Sara showed us how to make this incredible fruit salad, with jicama, watermelon, grapes, oranges, red onion, and ginger!” Of course, the recovery process was not overnight. “It did take a long time to really realize that he was going to be back to normal, that he was going to be okay and that he was going to be that strong provider for me and my children,” Alison reflects. “Mondo’s had an amazing outcome and he’s not limited in his activities at all and should hopefully have a life that’s not limited at all from heart disease as we’re monitoring everything and everything’s looking good,” reports his heart doctor Jayson Morgan, MD. Mondo describes his care experience being a heart attack survivor as life-changing. “The care teams at both Renown and ICR were incredible. There wasn’t a single person we came across who didn’t immediately become a part of the family. They truly cared for us, all of us, including the extended family that came to visit. They were informative and supportive. I felt like I created lasting bonds with so many of them, especially the gang in ICR. What amazing people.” Lynice Anderson, Director of Intensive Cardiac Rehab, Healthy Heart Program, shares,” Mondo is one of the most genuine, thoughtful and humble people I have ever met. His love for his family is palpable. His impact on me personally and our team is forever.” She acknowledges family support is key to his success, “Mondo’s family is his rock and they are his. I have never met a family that was so ‘all in’ in the support of their loved one. His new heart healthy lifestyle is modeled through his family every day.” Fighting The Good Fight Of course, Mondo may look familiar to you. That’s because he is featured in Renown Health’s “Fight The Good Fight” brand campaign. For this reason, you may have seen him in advertising working out on a treadmill, shirtless, with his open heart surgery scar in full view. When asked how he feels about showing his scar he confidently says, “I don’t mind showing it to people. I don’t. I earned that scar.” He is a proud heart attack survivor. Today, he’s grateful to be alive and takes his health commitment seriously. “Things have a different feel now. The skies and lakes are bluer and the trees greener. My family is so much more a part of my day. We go on so many more outdoor adventures, trying to incorporate a little exercise into our fun. We watch what we eat more and are trying to teach our children and loved ones about healthy choices. And I think with a few we’ve even been successful!” he observes. “Don’t take life for granted.” “Unconditional love. I get nothing but support from my family without them I wouldn’t be where I’m at. What happened to me definitely makes me a fighter for sure. I’m fighting for my life – the good fight – I think life is good,” he adds.
-
Making Patient Safety the Priority It Deserves to Be
I am regularly amazed by medical advancements and innovation in the United States. However, even as we make significant progress in many areas of medicine, there is still much more work to be done in others. One such area is patient safety. What is Patient Safety? When we talk about patient safety, we are discussing how hospitals and healthcare organizations protect patients from errors, injuries and infections. Anyone can make a mistake at work, but in healthcare these mistakes can result in serious outcomes. In 1999, the Institute of Medicine released a report that estimated 98,000 deaths per year result from medical examination or treatment. The most recent study in 2013 suggested these numbers could range from 210,000 to 440,000 deaths per year. Many of these deaths result from preventable medical errors. This is inexcusable and shows how much more work our industry still needs to do to improve patient safety. Making Patient Safety a Priority Patient Safety is our number one priority at Renown Health. We dedicate a lot of time to establishing, reviewing, and revising our processes to prevent errors. Despite the obvious importance of patient safety, this issue is largely left to individual hospitals and health systems to manage. There is a surprising lack of national attention around this truly important issue. However, a silver lining of the COVID-19 pandemic is that it is igniting interest in hygiene and infection prevention. Patients want to learn more about the processes that are in place to prevent the spread of infections. In addition to the many protocols that guide our treatment of injuries and illness, Renown Health has implemented the following measures to prevent the spread of communicable diseases: Requiring everyone entering Renown sites to wear a mask or face covering. Establishing new processes to help patients and visitors practice social distancing. Limiting the number of visitors in our facilities. Screening all employees and patients for symptoms. Enhancing our already-thorough cleaning and disinfection processes. I hope patient safety and infection prevention remain in the national spotlight long after the COVID-19 pandemic has ended. The healthcare industry must come together to develop stronger systems and regulations to minimize preventable medical errors. We have a responsibility to our patients to do better.
Read More About Making Patient Safety the Priority It Deserves to Be
-
Cancer Nutrition - Helpful Tips to Support Your Loved One to Eat Healthy
Eating healthy is a daily challenge for many, but for those with cancer it is an even harder struggle. A cancer diagnosis not only impacts those diagnosed, but family members and friends too. One key area of concern is making sure your loved one stays well by eating healthy food every day. Here are some essential cancer nutrition tips from Renown Health registered dietitians Jessica Blauenstein and Amy Laster. Help to Prepare Meals and Snacks for Daily Cancer Nutrition Make it grab and go. Easy-to-make meals help reduce the burden of having to cook and prepare food. Having easy to grab snacks on the counter or in the fridge can help ensure your loved one has access to those nutrients when needed. Sit outside of the kitchen. This allows your loved one to avoid cooking smells which can make them feel sick as a side effect of cancer treatments. Also try serving them cold foods such as sandwiches, cheese and crackers, or shakes which have a mild scent. Try drinkable meals. Some people with cancer find it easier to sip their calories over the course of 30 minutes to an hour. Consider smoothies or supplemental shakes such as Ensure Enlive or Boost Plus as snacks not meal replacements. A great foundation for a smoothie is a protein source (Greek yogurt, protein powder, nut butters or milk) with a carbohydrate (fruits, juice or berries). Add other ingredients as desired, such as spinach, kale, and ground flaxseed or chia seeds to give it more vitamins, minerals, and fiber. Snack Ideas for Those Undergoing Cancer Treatment The following ideas are both quick and easy to make for your loved one. Chicken or tuna salad with whole grain crackers or as a sandwich on whole grain bread Greek yogurt mixed with cereal, fruit and/or nuts Cottage cheese with banana, cinnamon and/or peanut butter Favorite fruit with 100% natural peanut or almond butter spread - Try peanut butter with bananas, apples, or even celery Their favorite veggies dipped in a salad dressing of your choice - For example, carrots with hummus or ranch dressing Cheese and whole grain crackers - Add tomato slices with a dash of oregano on top for more flavor Eggs scrambled with cheese, vegetables and/or salsa Peanut butter and jelly sandwich on whole grain bread A baked sweet potato with some favorite toppings Hard boiled eggs and/or egg salad with whole grain crackers, or as a sandwich on whole grain bread Oatmeal or cream of wheat prepared with milk, fruit and/or nuts Sometimes your loved one may not feel like eating or refuse to eat. If treatment side effects are impacting your loved one’s ability to eat, please visit the websites below containing recipes tailored to treat side effects. Cook for Your Life ELLICSR Of course you may also consult a registered dietitian and/or the patients care team, if you have more cancer nutrition concerns. No Appetite? Assisting with Cancer Taste Changes Taste changes are common during cancer treatment. Patients experiencing these changes may not feel like eating, which can negatively impact their nutrition. Help your loved one overcome taste changes with these cancer nutrition strategies: Metallic or bitter taste in food - add something sweet such as maple syrup, honey or jelly. You may also try adding fat, such as a nut butter, avocado or regular butter. Pickles or vinegar could help with this too. A taste like cardboard - try adding salt and extra flavor to foods with seasonings and spices. Some examples are onion, garlic, chili powder, basil, oregano, rosemary, tarragon, barbecue sauce, mustard, ketchup, or mint. Lemon juice, citrus, vinegar, or pickles may also help with this as well Food tastes too sweet - try adding six drops of lemon or lime juice. Add small amounts until the sweetness is gone. Very salty taste - try adding ¼ teaspoon of lemon juice. Try plastic utensils instead of metal, especially if your loved one is struggling with foods tasting metallic. Dipping small bites of food into either lemon juice or vinegar can have a “palate cleansing” feel and may improve taste perception. This helps avoid getting tired of the flavor after a few bites. Try marinating food or meats in sweet fruit juices, salad dressings, or sweet-and-sour sauce. Other “palate cleansing” foods are lime juice, orange juice, mangos, lemongrass, parsley, cilantro, mint, ginger, basil, and pickled foods. Use aroma to make foods appealing, avoiding any smells that may cause nausea. In particular, cinnamon, nutmeg, cloves, coriander, cumin, ginger, and black pepper can add an aromatic flavor. Also include herbs such as oregano, rosemary and thyme. Think texture. Consider trying wafers, crunchy nut butters, carrots, celery, cucumbers, chips, rice crispies, corn flakes, crackers, panko crumbs, nuts, or seeds if you are able to chew and swallow them safely. Remember that patience with your loved one's changing appetite and tastes can be the strongest form of support you can provide. Nutrition Tips for Cancer Survivorship and Beyond If eating large meals is difficult for your loved one, encourage them to snack throughout the day. Aim for 4-6 snacks or small meals per day. Focus on consuming 2-3 protein-rich foods each day such as lean animal meats, fish, eggs, soy or a protein supplement with 20-30 grams of protein per serving. Eat a variety of brightly colored fruits and veggies. Aim to make half of each meal fruits and vegetables. Eat less than 18 oz. (cooked weight) of red meat per week. Limit cold cuts, bacon, sausage, and hot dogs. Avoid excess salt and saturated fats. Cut back on simple carbs. (i.e. desserts, candies, white bread/pastas, french fries, packaged foods, chips) Drink in moderation- if at all- one drink per day for women, two for men. Get enough vitamin D (through diet and/or supplement) Avoid tobacco of any kind. Keep a healthy weight and stay up on exercise. Other Ways to Help a Loved One with Cancer Assist with Chores Allow your loved one to relax as you help take care of chores around the house, such as cleaning, cooking and grocery shopping. This may reduce overall stress and can be helpful for those that get tired after their treatments. Physical activity can still be beneficial, so be sure to do an activity together that they enjoy and is approved by their doctor. Be Patient It can be very difficult to see a loved one go through cancer treatment. Remember to be patient with your loved one. There may be things we want them to do or eat that we know would be good for them, however, meet your loved one with grace and understanding. It is ultimately their decision on what to do, just be there to support and assist them as they go through this challenging time. Additionally, Renown hosts free “Eating Well After Cancer Treatment” nutrition classes for cancer survivors. Our next cancer nutrition class series starts Thursday, June 3, 2021, and will be hosted virtually. It is open to anyone in the community. For more information or to register please click here.
Read More About Cancer Nutrition - Helpful Tips to Support Your Loved One to Eat Healthy
-
Addressing the Threat of Workplace Violence in Hospitals
In recent years, workplace violence against healthcare workers has been on the rise. According to the Occupational Safety and Health Administration (OSHA), about 75 percent of nearly 25,000 reported annual workplace assaults occur in healthcare and social service settings. Those who don’t work in healthcare may be surprised to learn that violent altercations are so common in our field. Hospital settings can create fear and stress for patients and their families. Pain, mind-altering medications and drugs, and difficult prognoses can amplify these feelings. While inappropriate responses may be understandable, violence cannot be tolerated. As the leader of a health system, protecting our employees is an issue that I take seriously. Reporting Workplace Violence Unfortunately, sometimes employees don’t report dangerous incidents fearing they might be blamed, or not realizing it’s a reportable offense. At Renown Health, we take these events seriously. We have clear, mandatory policies and protocols for reporting and investigating violent incidents. Each incident is investigated to ensure follow through and accountability. We also teach de-escalation skills to our hospital security teams, clinicians, and other frontline employees. As an added layer of protection, Renown Health has a first-rate security team that closely monitors activity on our campuses, addressing potential issues before they escalate. Our organization values our partnerships with community organizations including local law enforcement agencies like the Washoe County Sheriff’s Office and the Reno Police Department. Renown Health maintains a close relationship with these partners, and we alert them when our care teams experience an increase in violent incidents. I also recognize that workplace violence is a national problem that demands collaborative solutions. That’s why I am also proud to serve as a member of the American Hospital Association’s Hospitals Against Violence Advisory Committee. Nurses, doctors, paramedics, and frontline health workers care for us every day. It’s our responsibility to support them by ensuring they feel safe at work.
Read More About Addressing the Threat of Workplace Violence in Hospitals
-
From Cancer Survivor to Caregiver
Meet Haley Carroll Being a new nurse comes with many challenges and gaining experience is a journey, but Haley Carroll’s first day on the job was far from her first day in a hospital. Haley was diagnosed with lymphoma right before her senior year of high school, and she was declared cancer-free on December 2, 2015. Inspired by the incredible care she received during her cancer treatments and during her time at Renown Children’s Hospital, Haley enrolled in nursing school at the University of Nevada, Reno. She graduated in December 2020, just five years after beating cancer. “I’ve always been interested in nursing,” Haley says. “But once I was diagnosed and began to see everything that my nurses did for me, I knew that that’s what I wanted to do for patients, too.”
-
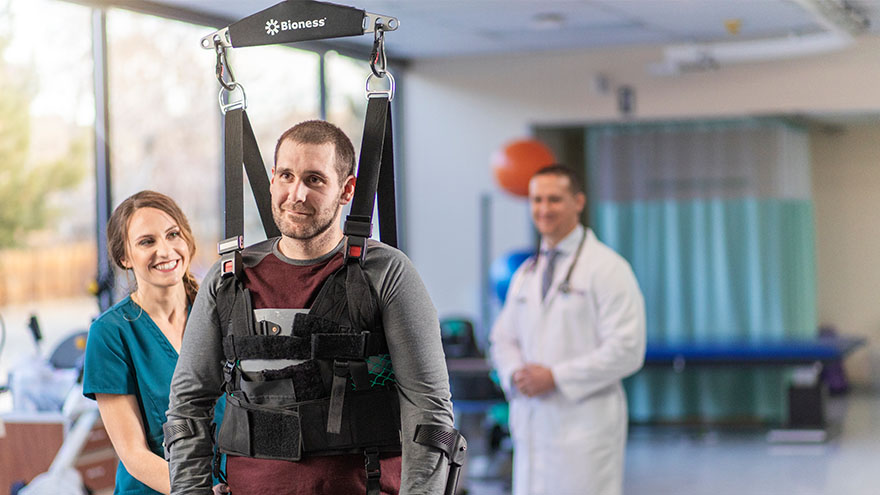
The Road to Recovery Close to Home
Meet Connor Smith Life was hectic for Connor Smith. He had just finished at the top of his class at both the fire academy and paramedic school and was looking forward to starting work in northern Nevada. It was winter 2019, and he was ready to have some fun. The plan was to ride ATVs at Sand Mountain with his brother Cody, dad Lance and some friends, but a jump would change everything. Connor’s ATV took off but landed awkwardly, and he remembers immediately knowing he was paralyzed. Connor’s mom, Dana Shugar, was at home when she received the upsetting call from Cody, who told her he had an accident. Connor was flown to Renown Regional Medical Center, the area’s only Level II Trauma Center. After a seven-hour emergency surgery, Dana learned that Connor would live but only had a slight chance of walking again due to a spinal fracture. “The surgeon saved his life. It’s amazing how your life can change in a matter of seconds,” she said. Once his condition stabilized, Connor moved to the Renown Rehabilitation Hospital and began physical rehabilitation. “Thank God for the people at rehab,” Dana said. “Dr. Pence, the therapists, nurses and all the employees were a wonderful support system, explaining everything and answering all our questions. The kindness they showed got me through.” Connor agrees, calling the Renown rehab team nothing short of amazing.
-
A Family's Legacy
Dr. Derek Beenfeldt first joined the Renown family in 2014 as a family medicine physician after graduating from University of Nevada, Reno, School of Medicine (UNR Med) in 2011. His son Davis was only 10 years old when Dr. Beenfeldt decided to change careers and attend medical school. Ten years later, Davis is following in his dad’s footsteps as a third year student at UNR Med. “I am proud of Davis for taking on the challenges and the commitment that I know goes along with attending medical school,” Dr. Beenfeldt said. “I also feel lucky that we have a medical school with such a great reputation and resources close to home.” The affiliation is a great source of pride for Dr. Beenfeldt. Not just because two important organizations in his life are joining forces, but he also sees it as both entities taking on an immense responsibility – the challenge to be better for incoming students, and subsequently to improve healthcare in Nevada. Davis is currently going through his rotations and spending countless hours a week at Renown Regional. His dad is right there by his side supporting him along the way. “It has been really interesting to have discussions about the UNR medical school with Davis, I recognize the names of many of the professors and courses from when I was a student,” Dr. Beenfeldt said. “I tried to be empathetic, as I can relate to how difficult and stressful this time is for him. Dr. Beenfeldt currently works as chief medical officer for Renown’s insurance arm Hometown Health, and Davis is still browsing specialties. “I don’t know what kind of medicine I want to focus on yet, but I feel lucky that I can attend medical school so close to home and have the option to continue helping my fellow Nevadans after I graduate.” UNR Med at a Glance UNR’s Medical School was established in 1969 Over the last 50 years, UNR Med has educated 3,900+ physicians More than 30% of UNR Med physician graduates continue to practice in Nevada UNR Med is the state’s oldest medical school
-
Reliable Care From Home
Renown Health has always been on the frontlines of technological advancement, and that innovation remained unwavering during the COVID-19 pandemic. Our telehealth teams heeded the call to provide home monitoring for our patients, transforming how we provide care. The care providers at Renown successfully monitored lower acuity COVID-19 patients from the comfort of their own homes. Bernard Lee was diagnosed with COVID-19 and pneumonia, and was able to return home to continue his recovery with a home monitoring system. While at home, Bernard’s health took a turn for the worse while he was sleeping, but thanks to the continuous monitoring of Health at Home, his worsening vitals did not go unnoticed. “This monitoring system really saved my life,” Bernard said. “It was telling me that my sats were low, but I didn’t even feel the common COVID symptoms; I just felt tired.” Because of his low oxygen saturation (sats) and the continuous monitoring, he woke up to providers calling to check on him in the early morning. He was immediately transferred to the Renown Intensive Care Unit to be cared for and monitored by our expert care teams. Today Bernard is recovering, feeling great and continuously refers to the team and the home monitoring system as his guardian angels.
-
What is Dry Drowning?
Whether you're a parent, grandparent, caregiver or sibling, you should know drowning is the second leading cause of death among children. Yet, while we are vigilant about protecting children from water accidents and drowning, a condition known as dry drowning or delayed drowning can go unnoticed. In fact, most people aren't even aware it exists. Dry drowning defined Dry drowning is a side-effect of a near-drowning experience and includes spasms of the vocal cords and larynx — known as a laryngospasm. This occurs when the body attempts to shut down the passage of any liquid into the lungs. Unfortunately, it can also shut down the passage of air into the lungs and force fluid into the stomach and lungs. Often the condition is not discovered until it's too late — severe cases can cause death within one to 24 hours after a water incident occurs. Who is susceptible? Novice or first-time swimmers are at increased risk, as are children with asthma and known breathing issues. In addition, children who have had pneumonia or experienced acute respiratory distress syndrome are also at greater risk. To reduce these factors, caregivers should be exceptionally watchful of inexperienced swimmers. According to Leland Sullivan, MD, of Northern Nevada Emergency Physicians, children under the age of 5 are most susceptible to drowning and often drown in residential swimming pools. Infants less than 1-year-old most often drown in bathtubs. What are the signs of a dry drowning episode? If your child has a near-drowning incident, a few moments of coughing until they calm down is normal. However, you should know the more severe signs and symptoms to watch for during the 24 hours following the incident, including: Persistent coughing Difficulty breathing and/or shortness of breath Chest pains Extreme fatigue and/or lethargy Change in typical behavior Face becomes pale What is the treatment and prognosis for dry drowning? Dr. Sullivan recommends that all victims of near-drowning incidents seek medical attention, even if they have no symptoms. If caught early, dry drowning can be treated. If you think your child is experiencing a dry drowning episode, go to the nearest emergency room as quickly as possible — do not attempt treatment at home. Healthcare professionals will work to supply oxygen to your child's lungs to restore and regulate breathing.
-
3,000 Miles Away But Close to Home
Overcoming poverty is not a task of charity, it is an act of justice. Like slavery and apartheid, poverty is not natural. It is man-made and can overcome by the actions of human beings. Sometimes it falls on a generation to be great. You can be that great generation. Let your greatness bloom. – Nelson Mandela, February 2005, Make Poverty History Campaign in London Lifting away the curtain that symbolized the front door, I entered a dark, cinderblock room and instantly became overwhelmed by an unpleasant odor. Working with oncology patients as a Child Life Specialist and an Occupational Therapist for over ten years, I recognized that smell. I had arrived in Guatemala – more than 3,000 miles from Reno – and it was my first day of a week-long trip where I would be serving alongside physicians in low-income communities providing free medical care for residents. My name is Brittany Jemmoua, I am an occupational therapist at Renown, and I recently volunteered with Kalan Kuxtal, a non-profit Guatemalan organization. I served alongside physicians by providing free primary care mobile clinics and home visits. The care we provided focused on prevention, intervention, education and lifestyle/medication management as we partnered with local entities, such as fire stations, community centers and schools to transform hundreds of lives. Speaking in both English and Spanish, I collected patient intake information, performed exams, tested for diabetes, and collaborated on a diabetes research project focused on daily risk assessment. Beyond these tasks, I immersed myself in the culture and learned more from the Guatemalan people than I could have ever imagined. Similar to Renown, Kalan Kuxtal Operates with Community at its Core Kalan Kuxtal, a Mayan expression meaning “life guardian,” is different from other volunteer medical trip organizations, and I took home valuable insights and lessons from their way of life that I now consider daily in my practice at Renown. I expanded my knowledge about diabetes, hypertension, pharmacology, infectious diseases, pregnancy complication, vector-borne illness and tuberculosis. We conducted home visits for socially neglected populations rather than expecting everyone to come to our clinics. I found that being welcomed into people’s homes gives you a different lens in which to view how their medical diagnoses interact with living conditions, occupations, and quality of life. This is when I met Mercedes and her mom. Her mom, Ms. Valencia, had jaundice skin and a substantial Basal Cell Carcinoma aggressively protruding from her face that impacted eating, hearing, seeing, sleep and social interactions. This opportunity to serve within their home led to an important palliative care conversation that would have been missed had we stayed in the clinic. We combed the rural neighborhoods assessing people’s risk for diabetes, taking glucose tests and educating families about their next steps. Many individuals had uncontrolled diabetes and misunderstandings regarding basic health management strategies. At the end of the day, many people demonstrated feelings of empowerment by actively offering solutions regarding how they will manage their day-to-day glucose with diet and exercise. Small actions can lead to big changes, and in the long-term, these health actions can help them avoid medication costs and focus on affording basic life necessities, such as water and electricity. Kalan Kuxtal organized a cultural day that included going to local businesses and community leaders to learn more about how they support the people of Guatemala. For example, Valhalla Macadamia Farm’s main goal is to help communities gain access to income, employment, and improved wellbeing by donating macadamia trees to families to grow and then sell macadamia products. A Weeklong Trip with Lifelong Impacts Each patient made a lasting impact on me, both personally and professionally. One specific family I saw in the clinic had a unique situation in that their two-year-old daughter, Margareth Elizabeth Cifuentes Bautista, was laboriously diagnosed with irregular corneal syndrome associated with glaucoma of congenital origin. Due to Guatemala’s limited prenatal screens and interventions, Elizabeth is nearly blind. While highly spirited and happy, she trips, bumps and feels her way through life. One barrier to her healthcare access is that her hard-working parents remain well below the poverty line, making less than $900/month. I am working to connect them with generous US Ophthalmologists and pediatric eye specialists to explore how we might save her sight and help her family. Their biggest dream is that she could recover her eyesight. “I know that this is not a life-threatening situation, but it is still something that never stops hurting me,” Jorge Cifuentes, Elizabeth’s father, said. “Unfortunately, our situation here is very hard. This country [Guatemala], although beautiful, it is very difficult to get ahead. We are people living in underprivileged conditions which complicates our situation even more. However, we are still trying to thrive by being kind and hardworking people. Thank you for helping us.” I have had the privilege of an opportunity for education, access to healthcare, employment and am aware that inequity and injustice prevail. This experience reinforced my understanding that medicine is a physically and mentally demanding profession that requires a commitment to service, continuous learning and adaptation both on local and global scales. I encourage everyone to please join me in serving the underserved by volunteering. Brittany is an experienced Occupational Therapist at Renown and volunteers with Kalan Kuxtal and other entities, such as The Robert Unsworth Foundation and Rock Steady Boxing to elevate communities. She loves being an Occupational Therapist; however, her life experiences confirm that her true calling is to become a physician. She is currently applying to medical school. Brittany is eager to earn the responsibility to improve lives and communities as their engaged physician. Brittany is tentatively scheduled to return to Guatemala at the end of this year to continue partnering with the people for a better future. You are welcome to join!
-
A Renown Anesthesiologist's Unique Journey
Dr. Nariman Rahimzadeh’s career path has been anything but typical. From humble beginnings as a shuttle bus driver for Renown Regional Medical Center, then named Washoe Medical Center, to his service as Chief of Staff for Renown South Meadows Medical Center, the steps and detours he took along the way – and the strong support from his colleagues and family members – make up a tale of perseverance, conviction, compassion and inspiration. However, his healthcare career journey began several years before he even joined Washoe Medical Center in the 1990s. It all began 7,446 miles away in Iran. This is Dr. Rahimzadeh’s story. Defining Moments The moment Dr. Rahimzadeh knew he wanted to dedicate his career to the healthcare field started during his childhood. Growing up in Iran during the midst of the Iranian Revolution, a thought that often came to mind was, “Who is helping all the people injured in the war?” The answer? The doctors. “In Iranian society, doctors are extremely valued, as they are the first to help people in need,” said Dr. Rahimzadeh. “I knew I wanted to give back to society in some way, and I see my time in Iran as very formative in my future career. I just didn’t know it yet.” After immigrating to the U.S. with his family during his preteen years, he only had one mission: to support his family. “My desires were to help my family not fall behind,” he said. “I didn’t have career aspirations at the time. All I knew is that I wanted to help my family and my community, which immediately opened its arms up to us, as well as be a good student and a good ambassador for Iran.” Dr. Rahimzadeh remembers several influential people that helped solidify his aspiration from “helping people” to “helping people as a healthcare professional.” Their family physician and other medical professionals in the family’s lives were monumental in helping him make this decision. Coupled with his natural love for the sciences, the decision to become a doctor became clear. But the question remained, “How do I get started in the healthcare field?” No Links to Healthcare? No Problem With no physicians in his immediate family and no direct connections to healthcare, Dr. Rahimzadeh set off to follow the advice he received from the influential people in his life: get a job at a healthcare facility, regardless of what the job title is. Some of his friends had recently joined Washoe Medical Center as patient transporters and mentioned job openings that were available. He sprang into action and headed to Washoe Medical Center to apply. Just one problem – he didn’t have the EMT certification requirement. Enter Barry O’Sullivan, who would be Dr. Rahimzadeh’s first supervisor at Washoe Medical Center (and a friend he still speaks with to this day). Barry saw promise in Dr. Rahimzadeh immediately. As a result, Barry made a suggestion to him that would ultimately set him on the course towards medicine. “Barry told me that he had an open position that I could work while completing the senior year of my undergraduate degree and studying for my EMT certification and eventually becoming a patient transporter. He told me Washoe Medical Center would support me in this endeavor. So, I asked what the job was and learned it was driving a shuttle bus.” Without hesitation, Dr. Rahimzadeh responded, “I’ll take it.” And so, his fulfilling journey with Washoe Medical Center, and eventually Renown Health, began. While he finished up the last few months of his degree at the University of Nevada, Reno, (UNR) Dr. Rahimzadeh proudly drove the shuttle bus a few days a week. The job not only helped him pay for his degree and put food on the table, but it also allowed him to begin living out his passion for helping people in the healthcare field. Dr. Rahimzadeh graduated with his bachelor's degree in Pre-Medicine from UNR and finished his EMT certification program. Sure enough, Barry and Washoe Medical Center lived up to their promises and helped him secure his first direct healthcare job as an EMT and Patient Transporter with REMSA. But he didn’t stop there – after several years as a ground transporter, his career literally took flight. He joined REMSA Ground Ambulance and eventually Care Flight as a Flight EMT II, caring for patients that were flying to Washoe Medical Center from nearby communities that needed lifesaving medical care. Helping save lives every day as a member of the emergency medical team is an ultimate feat, especially when it comes to Dr. Rahimzadeh. And he didn’t stop there. Valuing One-on-One Connections In the 1990s, as it is today, the U.S. experienced a significant primary care provider shortage which resulted in many medical schools encouraging students to complete their residencies in a primary care specialty, like internal medicine – which is precisely what Dr. Rahimzadeh set out to do at the University of Connecticut. However, his mind would soon change about the course of his career. “I had a deep, introspective conversation with my residency program director, openly and honestly chatting about my future,” Dr. Rahimzadeh said. “I ended up taking a week off of my residency and wrote a long pros and cons list about what I wanted to do with my life in the medical field.” Eventually he decided on anesthesiology because of the opportunity to have a one-on-one relationship with every surgery patient, regardless of their procedure. “Even though it’s for a short duration of time, it is a very impactful relationship,” he said. “I feel I am making a difference in the outcomes and lives of patients every day.” Dr. Rahimzadeh finished his internal medicine residency in three years and passed his board exam, and he went on to do the same thing for anesthesiology. He then ventured back home to Reno. Career Progression at Its Finest Dr. Rahimzadeh knows that people don’t always get to settle down in a place that influenced their upbringing, care and dream, yet he was able to make that vision a reality for himself. “I feel like Renown Health and myself have this intertwined relationship that led to my growth as a person and as a physician,” he said. “For that, I feel very blessed." Upon his arrival back to Reno with two residencies under his belt, Dr. Rahimzadeh was quickly hired at one of the two anesthesiology groups in town at the time. He started his career with Sierra Anesthesia and after working for the group for several years, he joined Associated Anesthesiologists of Reno in 2014, which went on to become one of the largest anesthesiology groups in northern Nevada. The group continuously worked very closely with Renown, taking care of all of its surgical patient needs and eventually becoming Renown Medical Group employees as of April 1, 2022, with Dr. Rahimzadeh setting up his home base at the Renown South Meadows campus. Today, Dr. Rahimzadeh wears three “hats” at Renown. As a medical professional first and foremost, his largest “hat” is his general anesthesiologist role, where he cares for patients in the operating room. Another significant “hat” is his role as the Medical Director for Surgical Services, where he reviews surgical patient charges alongside his dedicated team of nurses and ensures optimal patient outcomes by verifying they have had the appropriate workup to proceed with surgery in a safe manner. To round out his immense responsibilities with Renown, he serves as Chief of Staff for Renown South Meadows, where he makes connections with colleagues and collaborates with leaders to review protocols, policies and address concerns that arise. Outside of Renown, Dr. Rahimzadeh is still a contributor within his own anesthesiology practice. He also is the current President of the Nevada State Society of Anesthesiologists and the Director to the Board of Directors of the American Society of Anesthesiologists, helping bridge the gap in anesthesia concerns between his northern and southern Nevada colleagues. He reflects on the opportunities Renown and our local community have extended to him by saying, “If you can dream big enough and continue to chase your dreams, you can make it happen right here.” On the COVID-19 Frontlines Nothing could prepare us for the dire situation hospitals on the east coast – especially those in Livingston, New Jersey – were experiencing at the beginning of the pandemic. Livingston was known as the “second hardest hit area” by COVID-19 in April of 2020. Hospitals were overwhelmed with patients in the ICU fighting for their lives. They needed help, and they needed help now. Unable and unwilling to sit idly by, Dr. Rahimzadeh and six of his colleagues from his practice traveled to Livingston to help. They jumped in on the frontlines alongside other anesthesiologists and intensivists to offset the sudden influx of COVID-19 patients. Many lives were saved, and Dr. Rahimzadeh was a direct part of that. “When you care and work with people that also care, you can move the needle a lot – it doesn’t matter where you're from,” he said. Home Means Nevada – and Renown Renown Health is deeply rooted in the northern Nevada community. Dr. Rahimzadeh is proud to be among a diverse team who have taken responsibility for its community for generations. "We live in a very passionate and caring community, which is often underestimated,” he said. “It’s clear to me that Renown refuses to settle. Renown is incredibly progressive in providing the best for the community. We never remain stagnant, we keep moving forward and we take care of your loved ones. This health system has never been able to sit still and settle for the status quo. That stands out to me.” One story especially sticks out to Dr. Rahimzadeh as the moment when he knew that Renown was home. In 1997 while working as a patient transporter, his grandmother passed away on the sixth floor of the Sierra Tower at what is now Renown Regional Medical Center. At the funeral, a huge bouquet of flowers arrived. Not being especially close to anyone in Reno yet, Dr. Rahimzadeh's family had no idea who sent the beautiful arrangement. Turns out, it was Rod Callahan, the Chief Operating Officer (COO) of Washoe Medical Center at the time. “At that point, I knew I wasn’t just a part of a workforce with thousands of employees,” said Dr. Rahimzadeh. “The COO cared so much about me that he felt compelled to send such a wonderful gift during a tragic time. That’s the value of a local, community-focused hospital; the people here know you and care about you. There’s a reason why people stay at Renown for so long – we feel that connection.” Dr. Rahimzadeh also reflected on how far Renown South Meadows has come, from the time he immigrated to the U.S. to today. “Growing up, Renown South Meadows was kind of a ‘mom and pop shop’ primarily serving senior citizens in one wing and surgical patients in the other,” he said. “Now, I am so proud to see how far it has come. It really made its niche in the community in a great way. The future is bright!” It’s clear that Dr. Rahimzadeh is leaving a lasting legacy with his family, from the local community to global medicine. His son is a senior at Baylor University in Texas with a strong desire to go into medicine, just like his dad. His daughter is a junior at Bishop Manogue Catholic High School in Reno and enjoys being involved in her community. His loving wife is a speech therapist in the area. The Rahimzadeh family is thriving together, and they all share the same conviction about northern Nevada and Renown: “This is home.”