Search
-
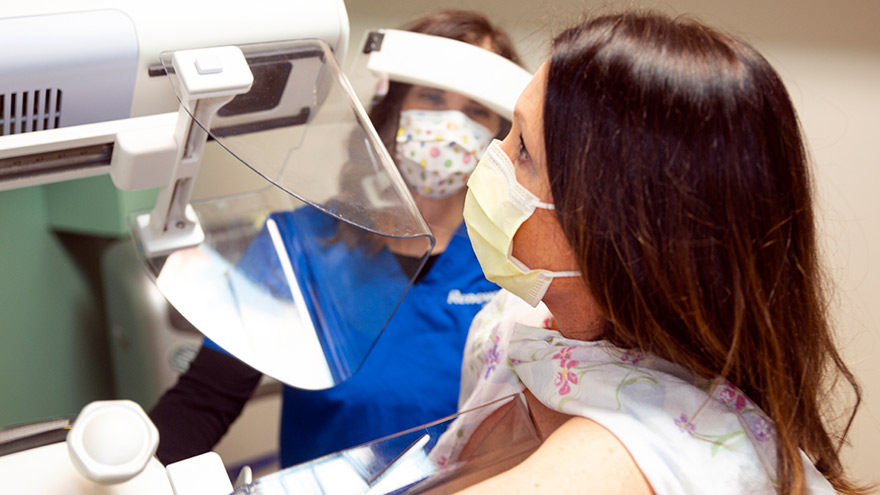
What Every Woman Needs to Know About Dense Breast Tissue
In honor of International Women’s Day, we’re working to spread the word about taking care of your breast health and encouraging the women in your life to do the same. Heather Reimer is on a mission — a mission to educate women everywhere about breast tissue type. For women with dense breasts, knowing your breast tissue type is absolutely critical, as cancers embedded in dense breast tissue are not always detectable with a mammogram alone. Dense breast tissue requires a breast ultrasound screening to get a complete breast health picture. Whole Breast Ultrasound for Dense Breast Tissue Heather knows this firsthand. She has dense breasts, and in this video she shares her story about finding breast cancer during a breast ultrasound screening — cancer that went undetected with her mammogram screening alone. As a result of that experience, Heather founded Each One. Tell One. — a movement to encourage women to pass along this information to others and to prompt those with dense breast and implants to consult with their doctor to schedule a whole breast ultrasound screening. To schedule a mammogram or a whole breast ultrasound, call 775-982-8100.
Read More About What Every Woman Needs to Know About Dense Breast Tissue
-
The Facts About Menopause and Early Menopause
Menopause is something that every woman experiences at some point in her lifetime. Learn what to expect and how you can help manage the symptoms and health risks. Most women don’t experience menopause until their 50s, but certain factors such as chromosomal abnormalities, glandular problems and chemotherapy can cause early menopause before the age of 40. No matter what your age, it’s a good idea be aware of the risks and treatments available to maintain a comfortable and healthy lifestyle. Health Risks of Menopause Two of the biggest health risks posed to women who have gone through menopause are bone density loss and risk of cardiovascular disease. Bone loss can be treated with bisphosphonate and estrogens. “Calcium with vitamin D and weight bearing exercise will also limit bone loss,” says Vickie Tippett, MD and OB/GYN at Renown Health. For cardiovascular risk, a healthy lifestyle is key. Discontinuing tobacco use, getting regular exercise and maintaining a healthy weight and diet all help reduce a woman’s risk of cardiovascular disease. Managing Discomforts of Menopause One of the most common complaints about menopause is the discomfort of hot flashes. “Hot flashes can be treated with systemic estrogen alone or in combination with progesterone or another agent similar to estrogen,” Dr. Tippett says. “Non-hormonal medications such as SSRIs and antidepressants also work.” Vaginal dryness, another common symptom of menopause, can also be treated with estrogen, estrogen-like compounds and personal lubricants. Pills, patches, creams and many other formulations are available to help alleviate discomfort. Knowing when, why and what to expect when it comes to menopause can help make the transition easier. Learn the facts about menopause in the infographic below.
Read More About The Facts About Menopause and Early Menopause
-
3D vs Whole Breast Ultrasound Which is Right for You
Breast cancer is the leading cause of cancer deaths in women in the U.S. That’s why early detection is so important. Dr. George Krakora, a radiologist with Renown Institute for Cancer, explains what to watch for and how new technology can lead to early detection. Most women know the importance of breast health and staying current with annual breast exams, but may not know that both screening guidelines and technology is evolving. So we asked George Krakora, MD, a radiologist for the Renown Institute for Cancer, what every woman should know about breast cancer detection and which screening method is right for them. First off, when should women start getting breast exams? Generally, women should start getting breast exams using mammography or ultrasound after they turn 40 years old. But we also want women ages 18 to 39 to talk to their primary care provider and ask for what’s called a formal risk assessment to see if screening is needed sooner. And you want to make sure your care provider is giving you a breast exam starting at age 25. It’s also a good idea to be familiar with how your breasts look and feel so you can report any changes to your care provider. What are the risk factors for breast cancer? Are there any preventive steps women can take? There a few risk factors you can’t control, like your age, family history of breast or other cancers, and if you have dense breast tissue. Your risk for breast cancer increases as you get older, and most breast cancers are diagnosed after age 50. Knowing your family history is important because a history of cancer and shared lifestyle can raise your risk. Your breast density can also increase your risk: Women with high breast density are four-to-five times more likely to get breast cancer than women with low breast density. But the good news is there are quite a few things you can do to prevent breast cancer, like not smoking, watching your alcohol intake, and maintaining a healthy weight with good diet and exercise. There are a lot of newer screenings out today. What is the difference between 2-D and 3-D mammography? In a 2-D mammogram, the tech takes X-rays of the breast. These pictures can show the radiologist if there are any lumps or tumors you might not be able to feel. In 3-D mammography, the process is largely the same but more X-rays are taken and it takes a few seconds longer for each image. This kind of exam detects 41 percent more cancers and reduces the number of false-positive results given to patients. This improvement in technology is great for both patients and their care providers. 3-D mammography provides better images of the breast, which allow doctors to more clearly diagnose and avoid false positives, especially in women with dense breast tissue. And what about a whole breast ultrasound. What is that? A whole breast ultrasound uses sound waves to detect cancerous tumors in the breast without using any radiation — it’s an ultrasound just like pregnant women get to check up on their baby. And the exam only takes about 20 minutes. We recommend these exams for patients whose mammograms have shown that they have dense breast tissue. Dense breast tissue can make it harder for doctors to see any abnormalities, lumps or tumors in a mammogram, so this technology ensures better early detection.
Read More About 3D vs Whole Breast Ultrasound Which is Right for You
-
Copays vs. Coinsurance: Know the Difference
Health insurance is complicated, but you don't have to figure it out alone. Understanding terms and definitions is important when comparing health insurance plans. When you know more about health insurance, it can be much easier to make the right choice for you and your family. A common question when it comes to health insurance is, "Who pays for what?" Health insurance plans are very diverse and depending on your plan, you can have different types of cost-sharing: the cost of a medical visit or procedure an insured person shares with their insurance company. Two common examples of cost-sharing are copayments and coinsurance. You've likely heard both terms, but what are they and how are they different? Copayments Copayments (or copays) are typically a fixed dollar amount the insured person pays for their visit or procedure. They are a standard part of many health insurance plans and are usually collected for services like doctor visits or prescription drugs. For example: You go to the doctor because you are feeling sick. Your insurance policy states that you have a $20 copay for doctor office visits. You pay your $20 copay at the time of service and see the doctor. Coinsurance This is typically a percentage of the total cost of a visit or procedure. Like copays, coinsurance is a standard form of cost-sharing found in many insurance plans. For example: After a fall, you require crutches while you heal. Your coinsurance for durable medical equipment, like crutches, is 20% of the total cost. The crutches cost $50, so your insurance company will pay $40, or 80%, of the total cost. You will be billed $10 for your 20% coinsurance.
-
Health Insurance Terms Explained: Deductible and Out-of-Pocket Maximum
Health insurance might be one of the most complicated purchases you will make throughout your life, so it is important to understand the terms and definitions insurance companies use. Keep these in mind as you are comparing health insurance plan options to choose the right plan for you and make the most of your health insurance benefits. One area of health insurance that can cause confusion is the difference between a plan's deductible and out-of-pocket maximum. They both represent points at which the insurance company starts paying for covered services, but what are they and how do they work? What is a deductible? A deductible is the dollar amount you pay to healthcare providers for covered services each year before insurance pays for services, other than preventive care. After you pay your deductible, you usually pay only a copayment (copay) or coinsurance for covered services. Your insurance company pays the rest. Generally, plans with lower monthly premiums have higher deductibles. Plans with higher monthly premiums usually have lower deductibles. What is the out-of-pocket maximum? An out-of-pocket maximum is the most you or your family will pay for covered services in a calendar year. It combines deductibles and cost-sharing costs (coinsurance and copays). The out-of-pocket maximum does not include costs you paid for insurance premiums, costs for not-covered services or services received out-of-network. Here's an example: You get into an accident and go to the emergency room. Your insurance policy has a $1,000 deductible and an out-of-pocket maximum of $4,500. You pay the $1,000 deductible to the hospital before your insurance company will pay for any of the covered services you need. If you received services at the hospital that exceed $1,000, the insurance company will pay the covered charges because you have met your deductible for the year. The $1,000 you paid goes toward your out-of-pocket maximum, leaving you with $3,500 left to pay on copays and coinsurance for the rest of the calendar year. If you need services at the emergency room or any other covered services in the future, you will still have to pay the copay or coinsurance amount included in your policy, which goes toward your out-of-pocket maximum. If you reach your out-of-pocket maximum, you will no longer pay copays or coinsurance and your insurance will pay for all of the covered services you require for the rest of the calendar year.
Read More About Health Insurance Terms Explained: Deductible and Out-of-Pocket Maximum
-
Get Moving: How to Exercise with Arthritis
An arthritis diagnosis doesn’t mean your exercise routine has to end. In fact, a consistent routine can actually improve mobility. Although stiff and painful joints can make it difficult to keep moving, staying active is essential for easing pain. October 11 is World Arthritis Day, so we asked Michelle Higgins, MPT at Renown Physical Therapy & Rehab some advice about exercising with arthritis. According to the Arthritis Foundation, arthritis affects one in five adults and 300,000 children. As a matter of fact arthritis is the nation’s leading cause of disability. Your joints certainly don’t need to suffer when you exercise. In general exercise is actually necessary for those with arthritis. Not only does it reduce joint pain, but it also increases strength and flexibility. Furthermore those adopting a regular exercise routine also have more energy, deeper sleep and find it easier to maintain a healthy weight. “Exercise is a necessary component to managing your arthritis,” says Higgins. “Consistent participation in an exercise program has been shown to promote long-term pain relief, increased body function and an improved quality of life. Alternatively, a lack of exercise can actually increase joint pain or stiffness and eventually lead to long term disability and suffering.” Exercising With Arthritis Exercise truly is the most effective non-drug arthritis treatment available for reducing pain and improving movement. And it can even include daily activities like gardening, dancing or walking your dog. Of course talk to your doctor or physical therapist about what exercises fit into your specific treatment plan. With this is mind, the four specific components below are important to an effective arthritis exercise program: Range of motion Moving joints through their full available range of movement is important. This frequently increases function and decreases joint stiffness and pain. For this reason, aim to complete these exercises daily. Examples include bending, straightening, and rotating specific joints, or static and dynamic stretching. Strengthening These exercises target muscles supporting and protecting our joints and bones. Strengthening is also necessary for weight control, so two-to-three sessions per week are recommended. In order to allow your body to adapt, begin with light resistance and start slow. Strength exercises include weightlifting and using resistance bands. Low-impact aerobic exercise Aerobic exercise is certainly necessary for overall well-being, weight management and heart health. Aim for two-to-three sessions a week. Low-impact exercises include walking, swimming, cycling, elliptical machine exercises and water aerobics. Balance Good balance is also vital for an effective arthritis program. On the positive side, solid balance prevents falls by increasing your ability to stay upright whether you are moving or sitting still. Likewise, it improves your confidence with walking and daily activities. In order to keep excellent balance, incorporate daily balance exercises. Examples of balance exercises include the use of an exercise ball, Tai Chi and exercises such as standing on one foot. Start Slow, Finish Strong As you begin your exercise program, remember to listen to your body. Start slowly – it can take several weeks for your body to adjust to exercise. Consult your doctor, or physical therapist, if you experience increasing pain or swelling which doesn’t go away with rest. Above all, incorporate fun and motivating activities so you’ll stick to them long term and improve your results. Renown Physical Therapy & Rehab 775-982-5001 Through outpatient physical, occupational and speech therapy, Renown Physical Therapy & Rehab gives you hands-on, individualized treatment in convenient Reno/Sparks locations. We have the latest, most advanced physical therapy and rehab equipment, specialty services and treatments. Renown Physical Therapy & Rehab is now open on Robb Drive in addition to three additional locations in Reno and Sparks. Call 775-982-5001 or visit us online.
-
Understanding "In-Network" and "Out-of-Network" Providers
When finding a provider to receive your health services, you've probably heard the terms "in-network" and "out-of-network" when it comes to your health plan. But what do these terms mean for a patient? And why should you be aware if a provider is out-of-network? What does it mean when a provider is "in-network" with a health plan? A provider is a person or facility that provides healthcare. When a provider is in-network it means there is a contractual agreement with that health plan regarding the rates for services. The provider will accept negotiated rates for services from the insurance. This means a patient will typically pay less for medical services received and is less likely to receive surprise bills. What does it mean when a provider is "out-of-network" with a health plan? Providers that are out-of-network are those that do not participate in that health plan's network. The provider is not contracted with the health insurance plan to accepted negotiated rates. This mean that patients will typically pay more or the full amount for the service they receive. Why should patients see in-network providers? Seeing an in-network provider for medical services can significantly reduce your medical expenses. Remember that in-network providers have a contractual agreement for negotiated rates with the health plan, so they cannot charge you more than that negotiated rate for a service. Seeing an in-network provider will always ensure any costs you do incur (copays or co-insurance) are applied to your health plan's deductible and out-of-pocket maximum (out-of-network costs don't apply to these amounts). To find the amounts you will pay for specific services, you can check your health insurance plan's Summary of Benefits. What is the best way to find which providers are in-network with a patient's health plan? Most health insurance companies offer multiple ways to find if a provider is in-network. To find the most accurate benefit information from your health plan, you can: Call their Customer Service department Check their website for their online provider directories If offered, check your online member portal.
Read More About Understanding "In-Network" and "Out-of-Network" Providers
-
3 Ways to Switch to a Medicaid Plan Accepted at Renown
Medicaid plays a significant role in our health care system and is the nation’s public health insurance program. In addition, this program is the predominant source of long-term care coverage for Americans. Renown Health is contracted with two Medicaid plans: Molina and Anthem. If you currently have a different plan but want to change to one that Renown accepts, you can request to change plans during the open enrollment period from January 1 to March 31. Request to change your Medicaid plan in one of three ways: Request a change to your plan, or managed care organization (MCO), by reviewing the available MCO plans online at bit.ly/MCOPlansNV and filling out the form on the webpage. Email Nevada Medicaid to ask for a plan change and include your name, Medicaid ID and the names and Medicaid IDs of any dependents in your home: MCORedistribution@dhcfp.nv.gov. Call your local Medicaid district office at 775-687-1900 (northern Nevada) or 702-668-4200 (southern Nevada) to ask about changing your plan. For more information about the Medicaid plans accepted at Renown Health, please visit: Anthem Molina Healthcare Renown Health accepts most insurances, but please visit the link below for the full list. Click here for all accepted plans
Read More About 3 Ways to Switch to a Medicaid Plan Accepted at Renown
-
Health Insurance Terms Explained: HMO, EPO and PPO Plans
When it comes to purchasing a health insurance plan, you’ve probably heard of the two plan types, HMO and PPO, but what exactly do these terms mean, and what is an EPO? Let’s learn more about these plan types and how you can choose the plan that meets your needs. What is an HMO Plan? HMO stands for “Health Maintenance Organization.” HMO plans contract with doctors and hospitals creating a network to provide health services for members in a specific area at lower rates, while also meeting quality standards. HMO plans require you to select a primary care physician (PCP) and usually require a referral from your PCP to see a specialist or to have certain tests done. If you choose to see a provider outside of the HMO’s network, the plan will not cover those services and you will be responsible for all charges. What is an EPO Plan? An EPO means “Exclusive Provider Organization.” This plan provides members with the opportunity to choose in-network providers within a broader network and to visit specialists without a referral from their primary care doctor. EPO plans offer a larger network than an HMO plan and typically do not have the out-of-network benefits of PPO plans. Generally, EPO plans cost more than an HMO, but less than a PPO. What is a PPO Plan? PPO stands for “Preferred Provider Organization.” PPO plans are often more flexible when it comes to choosing a doctor or a hospital. These plans still include a network of providers, but there are fewer restrictions on the providers you choose. PPO plans do not require you to select a primary care physician (PCP), giving you a broader network of providers. So, which plan should you choose? Each plan type has different benefits, so it depends on your health needs when choosing the right plan type. If you are looking for flexibility when choosing providers and locations, a PPO plan may better fit your needs. An EPO plan may be a better option if you travel often and want the flexibility of a larger network, but don’t necessarily need out-of-network benefits. If you regularly seek care in a certain geographic area and are looking for a health insurance plan at a lower price point, consider an HMO plan. To keep costs low, insurance carriers contract with providers and partner in plan members’ health to ensure quality care at the lowest cost. Whether you choose an HMO, EPO or PPO option, partnering with your health insurance carrier and your healthcare provider will help you receive the best care while controlling your out-of-pocket costs. Get the most out of your health insurance benefits! Established in 1988, Hometown Health is the insurance division of Renown Health and is northern Nevada’s largest and only locally-owned, not-for-profit insurance company providing wide-ranging medical coverage and great customer service to members.
Read More About Health Insurance Terms Explained: HMO, EPO and PPO Plans