Search
-
Use Caution: Mixing Over-the-Counter Medications Can Be Harmful
With allergy season’s extended stay and cold and flu season having just begun, you may soon find yourself seeking relief through several different kinds of over-the-counter medications. Know what precautions you need to take when fighting multiple symptoms with multiple medications. When you’re too sick to go to work but not sick enough for a doctor’s visit, over-the-counter medicines are a welcome relief to help alleviate that fever, runny nose or allergies. But because those medicines aren’t signed off on or managed by your doctor and pharmacist, it’s crucial that you’re especially mindful of what you put into your body. Whenever you pop a pill, you want to make sure you’re taking the right dosage, waiting the right amount of time before taking another dose and not mixing certain medicines together. Recent stories like this one detail dangerous over-the-counter medicine combinations, and we’re following suit: Here is a quick go-to guide about potentially harmful over-the-counter combinations. Too Much Tylenol/Acetaminophen Tylenol — or acetaminophen — is a popular pain reliever for many, but too much can be bad for your liver. “Our bodies have a finite ability to metabolize Tylenol,” says Andy Wright, clinical pharmacist at Renown Rehabilitation Hospital. “When too much builds up in the liver, it becomes toxic. In patients with medical conditions like cirrhosis of the liver or hepatitis, this could be disastrous.” Remember, acetaminophen is in more than just Tylenol and generic pain relievers. You may also see acetaminophen in flu, cold and cough medicines, like Nyquil, and some prescription medications including Norco and Percocet. Keep a list of the medications you take, and limit daily acetaminophen use to 3,000 mg per day. When you’re scanning medicine bottle contents, remember acetaminophen is also referred to as APAP, AC, acetam or paracetamol. Mixing Painkillers When you’re dealing with pain and not getting any relief, taking a different medication may seem like the easy solution. Maybe you take some Aleve — a form of naproxen — for a headache, but it isn’t working, so you switch to Motrin, an over-the-counter form of ibuprofen. Not a smart idea. Ibuprofen and naproxen along with aspirin are known as nonsteroidal anti-inflammatory drugs (NSAIDS). Because these medicines work in similar ways, they should never be combined or used in larger doses or more frequently than directed. Otherwise your risk of side effects can increase, which range from mild nausea to severe gastrointestinal bleeding. It’s also important to consider your family history when taking NSAIDs because, “recent studies have shown NSAIDs may have greater cardiovascular risks for people taking blood thinners or those with hypertension,” explains Andy. “A good example is ibuprofen: It has a relatively low gastrointestinal bleed risk while it has a moderate to high cardiovascular risk. The opposite is true for naproxen.” Rather than experimenting with multiple medicines, figure out which drug works best for you. You may find muscle soreness improves with aspirin, whereas when a headache hits, naproxen is best. Keep in mind that these medications aren’t always best for everyone in the family. “Aspirin in children and teens is not recommended unless under the supervision of a doctor,” Andy says. And pregnant and lactating women should generally avoid NSAIDS due to risk of birth defects and bleeding. “In both of these cases, acetaminophen or Tylenol are preferred but only if approved by an OB/GYN.” Fighting Allergies Over-the-counter antihistamines like Claritin, Zyrtec and Allegra have made fighting itchy eyes and runny noses a little easier. But these daily medicines — when taken inappropriately or in the wrong combinations — can also have an adverse effect. Similar to acetaminophen, you need to watch for antihistamines in other products. Sleep aids — like Tylenol PM and Unisom — commonly use an antihistamine known as diphenhydramine, which may increase your risk of overdose. “Combining antihistamines, or overdosing, can cause many adverse effects including dry mouth, blurred vision — even arrhythmias,” Andy says. “Only take these medications on their own.” If you’re still struggling with symptoms, you can talk to your doctor about adding an over-the-counter nasal steroid. Andy confirms the importance of closely following the directions listed on antihistamine (and all medicine) bottles. He has seen extended release nasal decongestants cause significant arrhythmias requiring medical care after a patient took the medicine with warm fluids. “The decongestant in question is designed to slowly release, but it can dissolve suddenly in the presence of warm liquids like coffee,” Andy explains. “This can cause the pill to deliver 12 to 24 hours of medication all at once.” Taking an Antidiarrheal with Calcium Calcium supplements and antidiarrheal medicines are another harmful combination. Calcium firms up your stool, but if taken with an antidiarrheal, can cause severe constipation. If you need to take an antidiarrheal, take a break from your calcium for a few days until you’re back to normal. Another consideration when taking calcium supplements or calcium-based antacids is gas. “I’ve had several patients report cases of excessive gas using Tums or calcium carbonate-based supplements.” Andy suggests instead “trying Maalox or Mylanta for indigestion and Citracal as a supplement.” Talk with Your Doctor or Pharmacist About Your Medications If over-the-counter drugs aren’t providing the relief you need, it’s time to see your doctor. And remember, for your safety it is important to keep your doctor and pharmacist up-to-date with any medications — prescribed or over-the-counter — that you are taking.
Read More About Use Caution: Mixing Over-the-Counter Medications Can Be Harmful
-
Think Outside the Box: Healthy, Creative School Lunch Hacks
Gone are the days of soggy PB&Js on white bread: Today’s school lunch is your chance to create a healthy, colorful midday meal! Here are a few simple tips, a week of lunch ideas and a shopping list to help you pack a lunch that won’t be offered up for trade during tomorrow’s lunch hour. While school lunches are getting healthier, packing and taking a lunch to school will ensure that your child is getting a healthy, well-balanced meal. Making lunches should be a team effort. Your kids can help pack their lunches by spreading on condiments or putting food in containers. To save time in the morning, pack lunches the night before. The following are a few suggested items you can use to ensure your child is eating a tasty but nutritious lunch: Main dishes Lunch meat and lowfat cheese roll ups English muffin pizzas Sandwich wraps – meat, cheese and veggies in a whole grain tortilla Pita pockets stuffed with grilled chicken and vegetables Soup Chef salad with spinach, veggies, cheese, lunch meat and dressing Tuna or chicken salad on a mini bagel Snacks and sides Fresh or dried fruit Natural apple sauce Baked tortilla chips and salsa Veggie sticks and hummus Cheese slices or string cheese with whole grain crackers Homemade trail mix with nuts, seeds and raisins Pudding Homemade fruit roll ups Popcorn (add different toppings such as salt, garlic, cinnamon, sugar or cayenne pepper) Drinks Water If you child doesn’t like plain water, try adding a few slices of fresh fruit (strawberries, lime, lemon) for more flavor. School Lunch Menu: Day-By-Day We’ve put together a week’s worth of colorful, fun and healthy school lunch ideas your kids will love. And we’ve also created a shopping list to help you easily locate all the ingredients on your weekend shopping trip. Monday: Turkey BLTA Roll-ups Roll-up Ingredients Turkey, cold cuts Bacon Avocado Tomatoes Side Dish Choices Blueberries Cucumbers Carrot sticks Tuesday: Bacon & Cucumber Sandwich Sandwich Ingredients Whole wheat English muffin Cucumber Bacon Side Dish Choices Apples slices Strawberries Vanilla yogurt mixed with sprinkled cinnamon Wednesday: DIY Lunchables Lunchables Ingredients Crackers Turkey, cold cuts Cheese Side Dish Choices Blueberries Carrots Cucumber Thursday: Veggie Grilled Cheese Veggie Grilled Cheese Ingredients English muffin Cheese Tomato Spinach leaves Avocado Side Dish Choices Apples slices Strawberries Vanilla yogurt mixed with sprinkled cinnamon Tomatoes Friday: DIY Pizzas DIY Pizza Ingredients 2 toasted English muffins Pizza sauce Cheese Turkey pepperoni Side Dish Choices Celery Black olives Shopping List (under 20 items) Cold section: Dairy 1 large container of vanilla yogurt 1 package of your favorite cheese Cold section: Deli meats 1 package of turkey pepperoni 1 package bacon 1 package turkey cold cuts Inside aisles Whole wheat English muffins 1 can of whole black olives 1 jar of pizza sauce 1 box of whole wheat or multigrain crackers Produce department 1 cucumber 1 stalk of celery 2 apples 1 container of strawberries 1 avocado 2 tomatoes 1 bunch of spinach leaves 1 container of blueberries 2 carrots For more healthy school lunch box options, visit our Kids Health & Nutrition board on Pinterest.
Read More About Think Outside the Box: Healthy, Creative School Lunch Hacks
-
Name-Brand Medication vs. Generic: What's the Difference?
Most prescriptions meds are available in generic form. Find out the similarities and differences between the two and how to determine whether a generic is right for you. Approximately 80 percent of prescriptions sold today are generics. If you’re taking a prescription medication, chances are it’s a generic form of the brand-name drug. But are you getting the same quality in a generic medication? Do generics measure up? The answer in most cases is yes — generics, just like branded products, are regulated by the Food and Drug Administration. “To have a generic product approved by the FDA, the generic manufacturer must prove that its product is bioequivalent to the branded product,” explains Adam Porath, PharmD, BCPS AQ-Cardiology, BCACP and Vice President of Pharmacy Services. Basically, it has to function the same. “Generic products are extremely well tolerated and will provide the same results as using a branded product,” Porath says. Here’s how generics are the same as name-brand prescriptions: Generic products contain the same active ingredients. They produce the same desired clinical effect and accompanying side effects. Generics come in the same form as their branded counterparts: pill, liquid or inhaler, for example. Release into the bloodstream matches the name brand in timing and strength. Here’s how they differ: Generics generally cost less. Federal law requires generics have different names and look different: shape, size, markings and color. Generics contain different inactive ingredients, like binders, fillers and artificial colors. Different side effects with generics can usually be attributed to these additions. Why do generics cost less? When pharmaceutical companies develop a new drug, they are paying for research, development, clinical studies, marketing — in some cases it can cost more than $800 million and take 10 to 15 years to develop a new drug. “The manufacturers of branded medication products have to recoup their research and development costs,” Porath says. So companies are granted a limited patent to sell their drug without the competition of generic counterparts. “When patent exclusivity ends, the market is open for any generic manufacturer to make a competing product with FDA approval.” Without the same startup costs, companies can sell generics at 80 to 85 percent less. And because more than one company can produce the same generics, competition drives prices even lower.
Read More About Name-Brand Medication vs. Generic: What's the Difference?
-
Learn How to Spot Asthma in Children and How It Is Treated
Sometimes, children’s asthma masks itself in symptoms that can be similar to other common respiratory problems. Dr. Shipra Singh of Renown Medical Group – Pediatrics discusses some diagnoses and treatments for asthma in children. Adults can easily recognize when we are out of breath or struggling to breathe, but what if you noticed this regularly happening to your infant or child during their daily play? Would you think they might have asthma? It may be difficult to tell if your small child has asthma because the symptoms can be similar to other common respiratory problems (bronchitis, croup, pneumonia) or even allergies. Read on to learn how to spot and manage asthma in your infant or child with advice from Shipra Singh, M.D., MPH, Pediatric Pulmonologist at Renown Medical Group – Pediatrics. According to the Centers for Disease Control, asthma in children is a leading chronic illness and cause of school absenteeism in the U.S. Asthma is a multi-factorial disease. Smoking during pregnancy or a family history of allergies or asthma has been linked to a greater chance of developing childhood asthma. Asthma is usually on a spectrum and not a single disease. It can range from mild to severe. Because an infant’s or toddler’s airway is smaller than in older children and adults, even a slight blockage caused by mucus or a restricted airway due to swelling can make breathing hard for them. In children five and younger, one of the most common causes of asthma symptoms is a respiratory virus, which narrows the airways in the lungs. These include a cold, the flu, bronchitis, pneumonia and other illnesses. How can I tell if my child has asthma? Unfortunately small children are unable to describe their symptoms, making asthma difficult to diagnose. Your child may even be active, playing and smiling, although they are experiencing chest tightness or labored breathing. Observe your child and let the child’s doctor know if: Your child’s breathing behavior has changed (coughing, wheezing, rapid breathing) Your child’s breathing pattern changes (day vs. night, with rest or activity, inside vs. outside) You have a family history of asthma or allergies Your child’s breathing is triggered by any foods or allergies With your help, your child’s doctor can make the best diagnosis to determine if your child has asthma. A pediatric pulmonologist (lung specialist) or pediatric allergist may also have to be consulted for special testing. Tests may include lung function testing, allergy tests, blood tests and X-rays for an accurate diagnosis. What is the treatment for infants and toddlers? Young children can use many of the same medications as older children and adults, although the way they take them and the dosage will differ. A nebulizer (or breathing machine) creating a medicated mist for your child to breathe through a mask may be used. An inhaler with a small spacer tube connected to a mask is also common to help your child breath medication into their lungs. Either of these options are effective. Asthma in children is treated with both fast-acting and long-term medicines to open up airways quickly for easy breathing and also to lessen asthma symptoms over time. Communicate with your child’s medical providers to create a personalized asthma management plan for them. How can I manage my child’s asthma? Recognize your child’s breathing habits and be aware of worsening symptoms. Consult with your child’s doctor on a daily asthma action plan to recognize worsening symptoms and track medications. (Here’s an example of an asthma action plan provided by the U.S. Department of Health and Human Services’ National Institutes of Health). Be consistent with the plan and talk to your doctor before changing it. Have an emergency plan in case of a serious asthma attack. Know where the closest ER is and know who can take care of your other children. Also know what the medical treatment coverage is under your insurance plan. We asked Dr. Singh about asthma in children: “Discussing asthma with your child may be a difficult subject. Some kids find the subject frightening or confusing. Others, especially the older kids, may be resentful of the treatment and may not be interested in doing the treatment. Talk to your doctor about advice to build an open and trusting relationship regarding your child’s asthma care.” What can I do to reduce my child’s asthma? Know your child’s asthma triggers (dust, pets, pollen, etc.) Follow your asthma action plan Keep your child away from smoke Can my child outgrow their asthma? Asthma symptoms change day to day and year to year. An older child can better recognize and manage their symptoms, so asthma episodes may lessen. However asthma is a life-long condition of the airways, so it is important to always have an asthma action plan, even with occasional asthma events. Renown Health Pediatric Care | Same-Day Appointments: 775-982-KIDS Our team of pediatricians, specialists and nurse practitioners have specialized training in children’s healthcare needs. We see children from birth to age 18 for the following pediatric needs: Wellness and preventive visits Sick visits Immunizations Behavioral health Allergy Asthma Common cold Diabetes Asthma resources for parents: Asthma and Allergy Foundation of America Centers for Disease Control and Prevention
Read More About Learn How to Spot Asthma in Children and How It Is Treated
-
One Patients Story of Survival
Thanks in part to the care provided by Renown’s award-winning team of ICU nurses, Tony Mowatt is alive, thriving and engaged. Read his story — and learn about the exclusive Beacon Award of Excellence — below. The open road. The growl of the engine. The feeling of freedom. That’s what Oakland resident Tony Mowatt was enjoying as he drove up Highway 88 toward Reno for the semi-annual Street Vibrations event. But he wasn’t expecting to hit the diesel truck — or to fly off of his bike over 100 yards, skidding onto the side of the road. He was severely injured and in the midst of rural Nevada. He had crashed just outside Centerville, Nev., and was miles away from any critical care hospital. Having the only trauma center equipped to treat his serious injuries, Tony was flown to Renown Regional Medical Center and admitted to the intensive care unit (ICU). ICU Nurses Treat Patient, Support Family Tony’s girlfriend, Tasha Klubock, was notified by his friend that he had been taken to the hospital. She immediately drove from Oakland to Reno to see Tony at Renown. Her first night there was overwhelming and scary — nobody knew if Tony was going to survive. But the nurses helped Tasha cope with the initial shock. Caring for the patient isn’t their only job — they also care for the family. “They [the nurses] just kept coming in and checking on me,” she said. “Angela was so amazing that first night. I really just bonded to her, and I remember when the shift switched, I panicked thinking about who was coming on and wanting to meet the next nurse … But they all came to talk to me — I had updates from everybody. It was just amazing.” ICU Nurses Became Family Tony spent 32 days in Renown’s Sierra ICU, surviving a serious head injury, all with Tasha by his side. He and Tasha still stay in touch with Renown nurses. “Even though this was literally one of the most hideous, craziest things to go through,” Tasha said. “There was so much hope and they became such a family to me and I still think of that time fondly because of the nurses.” “I’m alive because they wanted me to be,” Tony said. And Tony and Tasha are now happily engaged and planning their wedding. Exceptional Care: Renown ICU Nurses Win Awards Renown’s ICU nurses provide care like this every day to countless patients — it’s so second nature to them that they forget how exceptional it truly is. But it’s certainly care like Tony’s that has earned them national recognition. The American Association of Critical Care Nurses awarded the Beacon Award of Excellence to the Sierra, Cardiac and Roseview ICUs. These are the only ICUs in Nevada to obtain this honor. The Beacon Award recognizes critical care nursing teams who exemplify excellence in areas like leadership, process systems, quality care, knowledge, learning and development, excellence in patient care and superior patient health outcomes. “I couldn’t have been more proud of what we’ve done to accomplish this,” said Nick Dovedot, Cardiac ICU nurse. “It represents who we are. Just a great group of individuals who all work together as a team to make our patients get better.”
-
Get to Know the Types of Car Seats
Parents often struggle with installing and choosing car seats for their children. Picking out a car seat for your child is a never-ending battle. Safe Kids Washoe County has made it simple for you to understand the types of car seats that will work for your child. Types of Car Seats Rear-Facing Only Seat. Your baby's first car seat is often used from 5 to 40 pounds. People usually buy this type of seat because it is portable. Convertible Car Seat. This seat is larger and stays in the car; it may be rear-facing until your child is two years or more. After that, it can change to a forward-facing seat. Forward-facing-only car seat. This type of seat is used in one direction and has a 5-point harness and top tether. Combination seat. This is a forward-facing seat with a 5-point harness and top tether and can change into a booster seat when you remove the harness. 3-in-1 car seat. This seat also stays in the car. You can use it rear-facing, forward-facing, and then later, as a booster seat. Booster seat. It boosts the child for a safer and more comfortable fit of the adult seat belt. Make sure your child has outgrown the weight or height limits allowed in the forward-facing car seat. The seat belt must lie flat across your child's chest, on the bony part of the shoulder, and low on the hips or upper thighs. Most children will be between the ages of 8 to 12 years old before they are ready for the seat belt alone. Have a trained car seat technician check your installation Why: 3 out of 4 car seats are installed improperly, with some studies show that the misuse rate is 90%, with the average car seat having three mistakes. Solution: Ensuring that your child's car seat is installed correctly by a certified car seat technician will ensure your child's safety.
-
Local Organization Receive $250K Build Health Challenge Award
Award given to Truckee Meadows Health Communities, Renown Health & Washoe County Health District. Truckee Meadows Healthy Communities (TMHC), Renown Health and the Washoe County Health District received the BUILD Health Challenge® award, a $250,000 grant to support Caring For Reno’s Elders (C.A.R.E.) program. The award comes as a collaborative result of more than 30 local organizations submitting a proposal for the funding. Renown Health announced that the organization is matching the grant alongside other pledged funding from the community, bringing the current C.A.R.E. support to $580,000. Together the entities will focus on senior loneliness and the health issues it creates. The partners are honored that Truckee Meadows was selected as one of 18 communities to receive funding from BUILD in the 2019-2021 term. “C.A.R.E will be a community approach to enhance life quality for elders by reducing social isolation and loneliness, issues that seriously impact senior health,” said co-team leader Kindle Craig, Sr. Director Renown Institutes. “Loneliness is the root cause of many issues including suicide1 , chronic disease2 and a reduction in lifespan3 . Washoe County senior suicide rates are two and four times the national rate for those aged 65 and 85 years, respectively4 . That is unacceptable.” Sharon Zadra, TMHC executive director and co-team leader, said this project will tackle barriers to socialization such as access to affordable housing, transportation and healthcare. “We’ll bring the entire community on-board, long-term, to increase social connectedness and reduce health and mortality issues associated with loneliness by starting a cross generational ‘Kindness Epidemic,’” Zadra said. The BUILD Health Challenge is a national program focused on bold, upstream, integrated, local and data driven projects that can improve community health. The award provides funding, capacity building support and access to a national peer-learning network to enhance collaborative partnerships locally to address our community’s most pressing health challenges. The C.A.R.E team expresses special thanks to the BUILD Health Challenge for its support of this initiative. “Loneliness and isolation in our senior population leads to declines in both mental and physical health, and increased mortality,” said Kevin Dick, Washoe County District Health Officer. “We are incredibly honored to join the BUILD cohort, teaming with TMHC and Renown Health to bring long-term solutions by building a cohesive social network to improve the health of our elders.” The BUILD Health Challenge® is made possible with the support of: BlueCross BlueShield of South Carolina Foundation, the Blue Cross and Blue Shield of North Carolina Foundation, Blue Shield of California Foundation, Communities Foundation of Texas, de Beaumont Foundation, Episcopal Health Foundation, The Kresge Foundation, Methodist Healthcare Ministries of South Texas, Inc., New Jersey Health Initiatives, Robert Wood Johnson Foundation, and W.K. Kellogg Foundation. TMHC, Renown Health and WCHD have worked united for the last five years, rallying diverse partners and community leaders to influence and advocate for the region’s capacity to ensure a healthy community.
Read More About Local Organization Receive $250K Build Health Challenge Award
-
Transitioning Your Child Out of Their Car Seat
Car seat technicians often find parents are moving their child to their next car seat stage too soon, as they get older. Here are a few reminders of when to transition your child from their booster seat to a seat belt. Moving to a booster seat too soon According to Safe Kids Worldwide, nearly 9 in 10 parents remove children from their booster before they’ve reached the recommended height, weight, or age of their car seat recommendations, which leaves the seat belt in a position on the child that could injure them. If the child is not the proper height, the seat belt can rise up on the belly, instead of the hips where it’s supposed to sit, which can lead to spinal cord damage or whiplash in the event of a car crash. Solution: You can switch from a car seat to a booster seat when your child has topped the weight allowed by the car seat manufacturer; typically 40 to 80 pounds (18 to 36 kilograms). Remember, however, that your child is safest remaining in a car seat with a harness for as long as possible. Booster seats must always be used with a lap and shoulder belt — never a lap-only belt. Transitioning to a safety belt too soon Older children need booster seats to help ensure the seat belt stays properly positioned on their body. The lap belt should lie low across the child's hips and pelvis with the shoulder belt crosses the middle of the child's chest and shoulder, so that in the event of a crash, the forces are applied to the hip bones and not the abdomen. If the lap belt is not positioned properly then it could lead to injuries to the spinal cord and abdominal organs. Solution: Most kids can safely use an adult seat belt sometime between ages 8 and 12. Always use a booster seat until the child passes the 6-step test Your child reaches a height of 4 feet, 9 inches (nearly 1.5 meters) Their back is flat against the seat back. Knees bend over the edge of the seat and feet are flat on the floor. The shoulder belt sits on their shoulder and chest (not face or neck.) The lap belt sits low on their hips and touches their upper thighs (not on their stomach.) Your child can sit comfortably this way for the entire trip. The American Academy of Pediatrics reminds us that the back seat is the safest place for children younger than age 13.
Read More About Transitioning Your Child Out of Their Car Seat
-
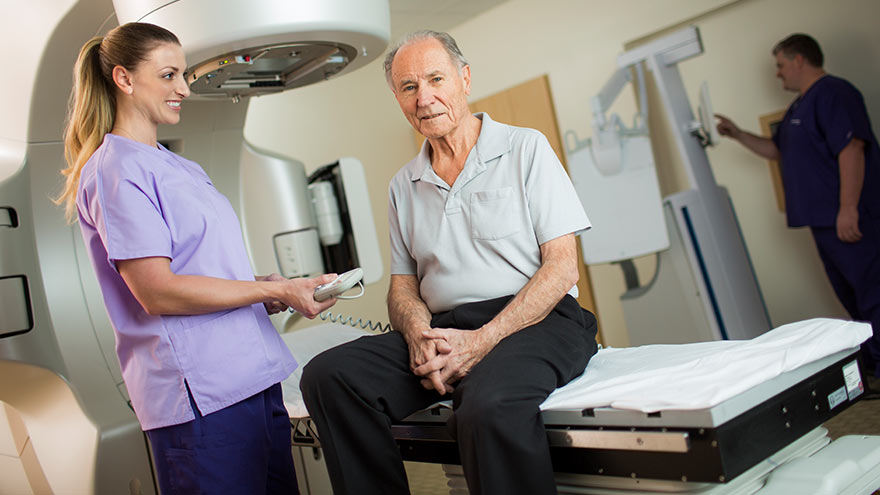
What Is the Importance of Having an Institute for Cancer?
What is an institute for cancer — and why does it matter that we have one right here in Reno? Here, a radiation oncologist answers those questions and more. Sadly, our community health needs assessment shows cancer is the second leading cause of death in Washoe County. But many residents may not know there is an institute for cancer right here in Reno that can care for you or your loved one after diagnosis. Dr. Michael Hardacre, a radiation oncologist with Renown Institute for Cancer is here with more. What is an institute for cancer? The way I like to think of it: An Institute has healthcare providers highly trained in patient-centered care. For example, when you have cancer, many times you’ll see a lot of doctors. A program brings those doctors together — so you really have one team working together. An Institute takes that one step further. Say there are other needs beyond the doctor’s office such as nurse navigators, dietitians, physical therapists to help you get on track, etc. An Institute really proactively thinks of the need of the cancer patient. It then makes sure all those things are available to them throughout their treatment. The term “institute for cancer” identifies a cancer program that is comprehensive and multidisciplinary in nature. For Renown, that means that we have the specialists in medical oncology, surgical oncology and radiation oncology working together with other specialists to assure that a patient has coordinated care throughout the entire treatment course of cancer care. Together with cancer prevention and diagnostics, genetic assessment, supportive care, clinical trials, and cancer survivorship, the institute for cancer provides care for the community, families and patients along the entire spectrum of cancer care. What types of cancer do you treat? We’re fortunate to be able to provide cancer treatments for all types of cancers, and we’re one of the major referral centers for northern Nevada. Most commonly, just like much of the country, lung cancer, prostate cancer and breast cancer are the most frequent we see. Our care spans brain, to neck cancer and everything in between. As an accredited comprehensive community cancer program, Renown Health provides services for all cancer types. The highest volume cancers treated at Renown are breast, colorectal, lung, genitourinary, blood and gynecologic cancers. Most treatments can be done right here in Reno, but when there are specialty needs such as stem cell or bone marrow transplantation, we partner with quaternary centers, like Stanford, to assure a smooth transition of care both to and from the quaternary center. What kinds of care and treatments are offered? We offer a wide range of comprehensive care. We treat the cancer itself — surgical, radiation oncology, medical oncology in the form of chemotherapy or pills. Also addressed: dietary needs, physical therapy and navigation through this whole process. People may be surprised by the scope and scale of the Renown Institute for Cancer. For instance, our Radiation Center has the latest technologies to treat cancers. This includes the Linear Accelerators, which are machines with treatment planning software tools. In addition to the traditional external radiation treatments provided in most centers, Renown performs specialty treatments using High-Dose Brachytherapy, a treatment with an active radiation “source” and in Brain Stereotactic Radiosurgery, assuring that patients can stay right here in northern Nevada — close to home. What does that mean for the quality of care? I think it’s always great in any environment to have external people come into your program and not only share what’s happening nationally and what we could do better, but also to validate “are you doing things at the highest level you can?” That accreditation process is just one way to give us that seal of approval. We’re lucky enough this year to get the gold award by the American College of Surgeons — its highest honor. We were honored to receive it. Why is important that you’re an accredited institute? Accreditation assures our community that quality is a top priority for us. Each of the accrediting bodies has a set of standards that identify service and quality standards. Renown Institute for Cancer has the following accreditations: American College of Surgeons’ Commission on Cancer: Full Cancer Program accreditation, standards address issues from cancer prevention/diagnosis to treatment to survivorship and/or end-of-life. Renown received the Gold Level Accreditation in 2018, the highest level of accreditation possible; American College of Surgeons’ National Accreditation Program for Breast Centers: Full Breast Center/Program accreditation, standards address issues from breast cancer prevention/diagnosis to treatment to survivorship and/or end-of-life; American College of Radiology – Radiation Therapy: Full Radiation Oncology accreditation for radiation equipment, treatment planning, treatment and treatment follow-up; and American College of Radiology – Mammography Services.
Read More About What Is the Importance of Having an Institute for Cancer?
-
Children's ER, Urgent Care or Wait it Out? Here's Your Guide
We’ve all been there: Your child gets sick right after urgent care closes — or worse, in the middle of the night. So do you wait it out, or do you load up and head to the Children’s ER? Pediatric Emergency Physician Joey Gassen, MD, with Northern Nevada Emergency Physicians, has insight. As parents, we often wish we had all the answers. And while a short-and-sweet comprehensive parenting guide is elusive, we can help if your questions involve whether to go to the children’s ER or wait it out. Here, a pediatric emergency physician explains when you should take your child to the Children’s ER at Renown Children’s Hospital, and what makes a children’s ER different. How do you know when it’s time to take your child to the ER? Having a sick or injured child is stressful. If you have a true emergency, you should go straight to the ER or call 911. When to go to the ER: Allergic reactions Asthma or severe shortness of breath Fever (infants less than two months old) Choking or poisoning Coughing up or vomiting blood Fainting, confusion or seizures Fractures or broken bones Head injuries Severe bleeding If you determine your child’s condition isn’t life-threatening but needs to be taken care of right away, urgent care is the best choice. Those conditions include: Cold and flu Coughs and sore throat Fevers Vomiting, diarrhea, stomach pain Cuts and severe scrapes Minor injuries and burns What is different about Renown Children’s ER compared to the adult ER? The difference starts when you first bring your child in. We have a lobby dedicated to our community’s smallest patients. The 24/7 lobby incorporates a child-friendly atmosphere with vibrant colors to help decrease anxiety that can accompany emergency situations. Our children’s ER also has equipment sized just for kids of any age. We offer a distraction machine, as well as games and movies, to help children cope with what can be a traumatic experience, like getting an IV. In addition, we have Child Life Specialists available to provide the emotional support to both children and their families. Why is it important to have an emergency room and lobby open 24/7 dedicated to children? Children aren’t just little people. They have special needs that require specialized care. Our children’s ER is staffed with skilled physicians and pediatric nurses certified in advanced pediatric emergency care to give your child the highest level of support. Renown Children’s Hospital From newborns to teens, Renown Children’s Hospital offers many different services and treatments designed specifically to take care of our community’s children. We provide a range of specialized services — from a dedicated Children’s ER and Pediatric ICU to a children’s imaging center and child’s asthma program. Explore Children’s Services
Read More About Children's ER, Urgent Care or Wait it Out? Here's Your Guide
-
How to Safely Give Children Over-the-Counter Medications
How can you ensure you’re giving your children safe doses of over-the-counter medications? The safest bet: Confirming dosages and recommendations with your doctor. With that in mind, here are a few answers to basic questions about OTC medications and children. It’s cold and flu season in Northern Nevada. This means you’ll find parents in the aisles of practically every drug store, wondering what will and will not work for their sick children. Over-the-counter (OTC) medications — and their dosages, side effects, interactions and more — can inspire abundant anxiety for parents. At the outset, the U.S. Food and Drug Administration offers the following warning about use of medicines for cough and colds in children: The FDA doesn’t recommend over-the-counter medicines for cough and cold symptoms in children younger than 2 years old. Prescription cough medicines containing codeine or hydrocodone are not indicated for use in children younger than 18 years old. Codeine and hydrocodone are opioids that are available in combination with other medicines, such as antihistamines and decongestants, in prescription medicines to treat cough and symptoms associated with allergies or the common cold for adults. Caregivers should also read labels on OTC cough and cold products, because some might contain codeine. So how can you feel comfortable administering any OTC medication to your children? The short answer is: Check with a doctor first. And with that in mind, here are a few common questions and answers from Kristin L. Wilson, MD, of Renown Pediatrics about children and OTC medications. Please talk about the importance of correct dosage of pediatric medications. Pediatric dosing is weight-based and unique to each medicine (and sometimes even the circumstance you are treating.) Therefore, there are no standardizations of “safe” amounts that apply to all medications. What are signs of an overdose of pediatric medications? Signs of intoxication/overdose are also unique to each medication and supplement. And to make it more confusing, mixing current prescriptions with various supplements or over-the-counter medications can cause significant adverse effects as well. Is there an age at which children take adult over-the-counter medications? Infants through adolescents can take medications that are also prescribed to adults, but only under a healthcare provider’s careful guidance. Dosing is determined by various factors dependent on child’s age and also medical history, as above. What is the takeaway about administering medications to children? When in doubt, ask a healthcare professional whether a medication or supplement is safe for your child based on his/her age and medical history as well as recommended dosing based on recent weights and other vital signs.
Read More About How to Safely Give Children Over-the-Counter Medications
-
A Day in the Life of a Child Life Specialist
March is Child Life Month, meaning this is the perfect time to ask: What exactly does a Child Life Specialist do? To find out, we “virtually” tagged along with one for a day. This is what a typical day looks like in this important role. For Child Life Specialist Brittany Best, play is a natural part of her work day. She approaches her role with a keen understanding of how the seemingly small tasks she performs every day — comforting children prior to a procedure, writing thank-you notes to donors, training interns — positively impact the lives of the children she serves and their families. So what does it take to work in Renown’s Child Life Program? Best shares some of the highlights from a “typical” shift. A Child Life Specialist’s Day 7:30 a.m. Clock in, put my belongings in my office, and print the patient census information. This helps me to get a sense of the day ahead, as I’m covering three areas today. 8-9 a.m. I look over the census sheets for all three areas and check in with the nurses in each area and then try to prioritize my day. 9:00 a.m. I attend Interdisciplinary Rounds for the Pediatric Intensive Care Unit, where the most critically ill or injured children are treated. Additionally, Interdisciplinary Rounds enable several key members of a patient’s care team to come together and offer expertise in patient care. 10:00 a.m. I come up to the specialty clinic/infusion center to check on the patients that have arrived already and see how things have been going since I had last seen them. We see patients frequently up here, as they are receiving treatment for cancer or other disease processes. 10:55 a.m. I’m notified by an RN that a patient needs an IV started, so I go meet with the patient and their family. I meet with a 6-year-old and mother to explain what an IV is and why it is needed. We go through an IV prep kit, looking at all the different items the nurse will use including cold stinky soap, a tight rubber band and also a flexible straw. I also teach this patient a breathing exercise to help them relax during the procedure with a simple exercise known as “smell flowers, blow out candles.” I demonstrate how to take a deep breath in through the nose — like smelling flowers — then how to blow that breath out — like blowing out birthday candles. 11:10 a.m. I walk with the patient and mom to the procedure room on the Children’s Patient Floor for an IV procedure. The Vecta distraction station is set up and running with its bright lights and water tube that bubbles with plastic fish swimming. The parent holds the patient in their lap, and with the distraction and medical preparation, we are successful! I give the patient a toy and provide emotional support to both the young patient and his mom. It’s easy to forget that these procedures can be stressful for the parents as well. 11:30 a.m. I finish rounding with staff to catch up on patients. In addition, I introduce myself to patients and put my contact number on the board in each room so the families know how to get a hold of me should they need anything. With support from volunteers, we distribute movies, games, and “All About Me” forms to patients and their families. These forms help us get to know our patients with things like their favorite foods and televisions shows. 12:45 p.m. I help with a lab draw in Children’s Specialty Care. A 3-year-old patient is very anxious about the “shot,” so I meet with the patient and parents to discuss coping techniques. The patient holds the Buzzy Bee and does well during the lab draw. The mom is relieved, and the patient is excited for a toy. The Buzzy Bee actually helps block the transmission of sharp pain on contact through icy numbing and also tingly vibration. 1 p.m. Joan, an artist with our Healing Arts Program, arrives on the Children’s Patient Floor to perform art therapy with patients. She helps two young patients who are interested in watercolor paintings. 1:15 p.m. Time for lunch and also a trip to Starbucks. 1:45 p.m. I finishing rounding and introducing myself and our services to the patients I have not met yet. 3 p.m. At this time, I meet with the parents of a newly diagnosed diabetic patient who is in intensive care. A new chronic diagnosis is always difficult, so I am there to provide emotional support. It’s instances like this that remind me every day why I love the work I do. 3:30 p.m. I meet with a new volunteer, discuss their role and also give the new volunteer a tour of the units. We are very thankful for all our volunteers on the floor, as their contributions help us provide a variety of basic services to a larger number of children. This also allows the Child Life Specialist to devote time to children who require more intense or specialized service. 4-5 p.m. I finish charting on patients and help two newly admitted families before I start to wrap up for the day. This evening we have a volunteer covering the times during shift change, which is helpful as it makes for a smooth transition for families during the meal time and change of shift. During this time, I write a note for this volunteer indicating the patients I want her to focus on. 5-5:30 p.m. Check in with critical patients and families before leaving for the day. All-in-all, it was a good day.
Read More About A Day in the Life of a Child Life Specialist