Search
-
Air Guard RN Makes an Impact in Community and Beyond
Everyday, Renown salutes its more than 150 active military and veterans on staff. Becca Gilbert, a Renown trauma nurse, is an example of the many outstanding service members at Renown who are serving both their country and their community. Becca Gilbert, BSN, RN, wears many uniforms. When she’s not wearing scrubs in her role as a trauma nurse in the intensive care unit of Renown Regional Medical Center, she’s wearing fatigues as a first lieutenant in the Nevada Air National Guard. “Service is huge,” says Becca Gilbert, RN, of her role in the Air Guard. “It’s something that is ingrained in me and a big part of who I am as a person. I find a lot of pride in being a part of something that is bigger than what is going on in my world.” Renown Health was named one of 15 recipients across the nation — and the only health system in the U.S. — for the Department of Defense’s highest employer award, the Secretary of Defense Employer Support Freedom Award, for exceptional support of its military employees. The Employer Support of the Guard and Reserves and Renown held a ceremony June 29 to recognize the award and to honor representatives of Renown who currently serve in the Guard and Reserves. With her Air Guard background, Gilbert is preassigned veteran patients at the Renown ICU. She says she’s able to relate to the veterans and their families and create a quick bond with them. “I’ve been assigned patients who are guard members with traumatic injuries — it’s good but hard,” Gilbert explains. “But I really love working with patients who are veterans.” Gilbert’s first career was as a veterinarian technician. Then enlisted in the Nevada Air National Guard in August 2008 — following in her father’s footsteps — and trained to serve as an EMT. While she was a medic, she went to nursing school for her second bachelor’s degree and was able to commission as an officer after graduation. Serving Our Community Gilbert says her work in the guard offers benefits that help with her job responsibilities at Renown, where she’s worked for four years. “At Renown, we are really a team and rely on each other to make sure there are good outcomes,” she says. “In the guard, officers are often put in charge, which teaches you a lot of things — organization, decision making and thinking of others. I think all of those things go hand-in-hand with my role as a nurse, especially in the ICU. People in the guard count on you as an officer and leader, and that is really important in the ICU when patients are counting on you for a positive outcome.” Gilbert’s responsibilities in the guard vary, including training for disaster relief missions and ensuring service members are fit and healthy enough to perform their jobs. “Training is a large part of the military — trauma training, physical fitness training and staying current on certifications,” she says. Locally she also leads the Self Aid Buddy Care program, a United States Air Force program that encompasses basic life support and limb-saving techniques to help wounded or injured personnel survive in medical emergencies until medical help is available. With the guard, Gilbert has also been involved in a bleeding-control program for volunteers in the community. She teaches community groups how to stop bleeding if they are a bystander to a car accident or other type of event, and is working with Renown trauma surgeon Marty Bain, M.D. to implement the program at Renown as well. Making a Difference Abroad In January, Gilbert was presented with an opportunity through the Nevada Guard State Partnership Program to travel outside the United States to the Kingdom of Tonga in the South Pacific and work at the Women and Children Crisis Centre, which assists families who are dealing with domestic violence. Gilbert praised the women who work at the center for their efforts towards change, as she says domestic violence is common in Tonga. “The women who work at the Women and Children Crisis Centre are pioneers,” she says. “They are trying to make changes by documenting what is going on and providing statistics to the lords and kings of Tonga. Some of it still isn’t accepted, but they continue to help the women and children of Tonga. They are helping so many people.” Renown Health salutes Gilbert for her tireless service to her country and her community here at home.
Read More About Air Guard RN Makes an Impact in Community and Beyond
-
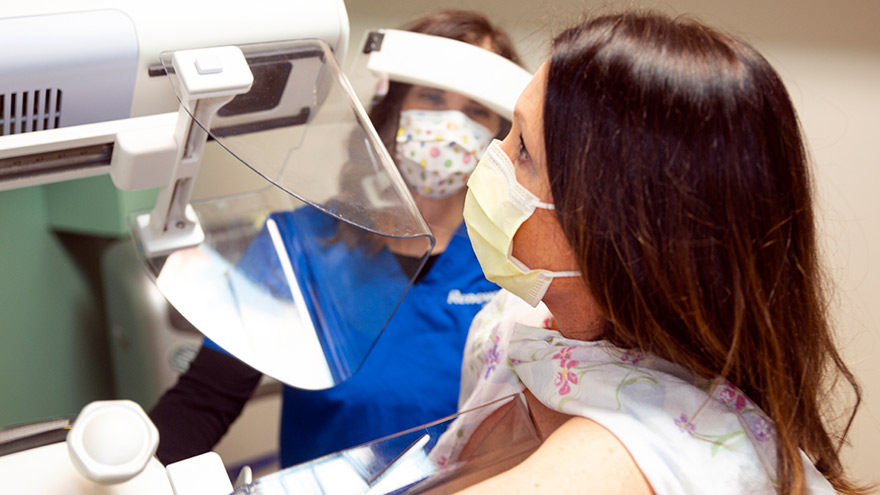
3D vs Whole Breast Ultrasound Which is Right for You
Breast cancer is the leading cause of cancer deaths in women in the U.S. That’s why early detection is so important. Dr. George Krakora, a radiologist with Renown Institute for Cancer, explains what to watch for and how new technology can lead to early detection. Most women know the importance of breast health and staying current with annual breast exams, but may not know that both screening guidelines and technology is evolving. So we asked George Krakora, MD, a radiologist for the Renown Institute for Cancer, what every woman should know about breast cancer detection and which screening method is right for them. First off, when should women start getting breast exams? Generally, women should start getting breast exams using mammography or ultrasound after they turn 40 years old. But we also want women ages 18 to 39 to talk to their primary care provider and ask for what’s called a formal risk assessment to see if screening is needed sooner. And you want to make sure your care provider is giving you a breast exam starting at age 25. It’s also a good idea to be familiar with how your breasts look and feel so you can report any changes to your care provider. What are the risk factors for breast cancer? Are there any preventive steps women can take? There a few risk factors you can’t control, like your age, family history of breast or other cancers, and if you have dense breast tissue. Your risk for breast cancer increases as you get older, and most breast cancers are diagnosed after age 50. Knowing your family history is important because a history of cancer and shared lifestyle can raise your risk. Your breast density can also increase your risk: Women with high breast density are four-to-five times more likely to get breast cancer than women with low breast density. But the good news is there are quite a few things you can do to prevent breast cancer, like not smoking, watching your alcohol intake, and maintaining a healthy weight with good diet and exercise. There are a lot of newer screenings out today. What is the difference between 2-D and 3-D mammography? In a 2-D mammogram, the tech takes X-rays of the breast. These pictures can show the radiologist if there are any lumps or tumors you might not be able to feel. In 3-D mammography, the process is largely the same but more X-rays are taken and it takes a few seconds longer for each image. This kind of exam detects 41 percent more cancers and reduces the number of false-positive results given to patients. This improvement in technology is great for both patients and their care providers. 3-D mammography provides better images of the breast, which allow doctors to more clearly diagnose and avoid false positives, especially in women with dense breast tissue. And what about a whole breast ultrasound. What is that? A whole breast ultrasound uses sound waves to detect cancerous tumors in the breast without using any radiation — it’s an ultrasound just like pregnant women get to check up on their baby. And the exam only takes about 20 minutes. We recommend these exams for patients whose mammograms have shown that they have dense breast tissue. Dense breast tissue can make it harder for doctors to see any abnormalities, lumps or tumors in a mammogram, so this technology ensures better early detection.
Read More About 3D vs Whole Breast Ultrasound Which is Right for You
-
The Journey Within: Helping Others Through Grief
Learn more about a Renown Health nurse who formed a nonprofit to help other families through loss. After the unexpected loss of her young husband, a Renown Health nurse turned her grief into helping other families navigate the loss of a family member. Jen Walker, RN, MSN, director of clinical excellence, lost her high school sweetheart and husband of eight years when he passed away in October 2015, while their two boys, age 7 and 9, lost their father. Walker, a nurse at Renown since 2003, was overwhelmed by the outpouring of support she received from the Reno community. It inspired her to want to help others in the same situation. “After Travis passed, the community did some amazing things for me,” Walker says. “I got really motivated to do the same thing and to give back, so that’s when I came up with starting The Journey Within.” The Journey Within organization provides support and resources for young families who have lost a close family member. Before officially starting her organization, Walker used some of the money she received after her husband passed and personally donated to three families. And with the help of four board members, Jen officially started The Journey Within in February 2017, and they have helped six families so far. One of the board members is her sister, Anny Goff. “She thought of creating this foundation in the darkest time of her family’s life,” Goff says. “She knew there would be other families that would need help and support and immediately wanted to help others. It showed incredible strength and courage to keep moving forward.” Nursing Careers at Renown Health Nurses at Renown Health demonstrate a commitment to patients and their families through the integration of care, clinical expertise, education, evidence-based practice and the pursuit of quality patient outcomes. Learn more about our mission, vision and values and the benefits of a career in nursing at Renown Health today. Explore Nursing at Renown Walker’s organization supports families through financial donations, which she funds through two yearly fundraisers. The Travy Tourney is a golf tournament held in memory of Travis, and the “Let’s Toast to Travis Fundraiser” event raffles prizes and merchandise. Along with financial support, The Journey Within helps families connect with other community resources, such as counseling and grief therapy services. Walker hopes to expand her nonprofit’s fundraising and support for families beyond the Reno-Tahoe community. Because of her outstanding work at Renown and in the community, Walker recently received a 20 Under 40 award from the Reno-Tahoe Young Professionals Network. She has also received a Women of Achievement award, a Leader of the Quarter award and has been nominated four times for Northern Nevada Nurses of Achievement. “She is strong and resilient and cares a lot about people,” says Jen Richards, chief nursing officer, acute care services. “She never settles for the status quo and is always pushing our team to do better.” In navigating her own loss and starting a nonprofit to give back, Walker has learned a lot about the community. “I’ve gained a tremendous amount of respect for the community as a whole, but especially for the young community,” she says. “Seeing the young people in the community who have been willing to give back and live really selflessly has been amazing to me.” As someone who lost her husband, helping young families who have gone through the loss of a close loved one can hit close to home for Walker, but that doesn’t stop her — it fuels her. “That’s one of the hardest parts about doing this — it takes you back a little bit,” she says. “But it’s just a very good reminder of ‘why.’ Because when I get to talk with these families, I realize that now I am that person who is there to listen. I just want them to know that they’re talking to someone who’s been through something similar.”
Read More About The Journey Within: Helping Others Through Grief
-
Caring for the Whole Family: Renown Nurse Helps Patient with Ailing Pet
Registered Nurse Tori Tembey (left) shared how her co-worker and fellow RN Jennifer Payne helped a patient with his pet's end-of-life arrangements. "It was such a selfless act that Jennifer took the time to do this for the patient.” Tembey says. Pets become members of our own family, and when they are ill or at the end of their lives, it can be devastating for their owners. During a hospital stay, a Renown patient was faced with the difficult decision to euthanize their terminally ill pet. A Renown registered nurse stepped in to help in some pretty remarkable ways. Back in high school, Jennifer Payne wanted to be a veterinarian. She worked in a veterinary hospital and planned to attend veterinary school, but struggled with some of the situations she faced. “I have a lot of compassion for animals,” Payne explains. “And some of the things I saw while working at the vet — like people bringing in their cat saying, ‘I’m moving, you need to put this cat down’ — wasn’t OK with me, and wasn’t what I wanted to do.” She changed course and went into nursing, but recently drew upon her early experiences working with pets and their owners to help a Renown patient in an extraordinary way. Payne now works in the trauma intensive care unit at Renown Regional Medical Center, where she recently observed a county animal control officer visiting a patient. The patient was visibly upset — they learned their dog was terminally ill and in poor health, and a veterinarian was recommending euthanasia. The patient had lost another dog just before Christmas. The patient hoped to have his ill dog similarly cremated, but animal control does not perform cremation. “I overheard all of this and thought, ‘this is the most horrible thing I’ve ever heard,’” Payne says. She offered to pick up the dog, have him cremated and bring the ashes to the patient. She also took up a collection with her Renown colleagues to pay for the cremation. The next day — her day off — Payne and her young daughter picked up the ashes and brought them to the patient at the hospital. “He couldn’t even talk because he was crying so much,” Payne says. “He said ‘I can’t thank you enough for all you’ve done. You’re a wonderful person.’ There was a friend in the room who asked what my daughter’s name was, and I said ‘Estelle.’ The friend said, ‘Estelle, your mother is an angel.’” Payne, who has a golden retriever of her own, says she knows what it’s like to have “fur babies,” and she could see how important this dog was to the patient. “It was great to be able to do this for him,” she says. Renown salutes nurses like Jennifer Payne, who are making a genuine difference everyday in the lives of patients and in the community.
Read More About Caring for the Whole Family: Renown Nurse Helps Patient with Ailing Pet
-
Know Your Numbers, Save Your Heart
There are some important numbers to know when it comes to good health. Learn more and receive a free blood pressure check at a primary care open house Feb. 27 at Renown Medical Group – Double R. Know Your Numbers Adults are pretty good at knowing and memorizing numbers — from passwords and PINs to addresses and phone numbers. But what about the numbers that could help save your life? Heart disease remains the leading cause of death in the U.S., with 633,842 deaths attributed to the disease in 2016, according to the National Center for Health Statistics. The American Heart Association lists the vital numbers you need to monitor to help prevent heart disease as blood pressure, total cholesterol, blood sugar and body mass index (BMI). With these numbers, your doctor can assess your risk of developing heart issues such as atherosclerosis, which can lead to other serious heart conditions. Atherosclerosis is a condition wherein plaque builds up in the arteries — the blood vessels that transport oxygen-rich blood to cells, the heart and other organs. These fatty deposits clog the arteries, inhibiting blood flow and reducing the amount of much-needed oxygen the body receives. These blockages can lead to angina, coronary heart disease, peripheral artery disease and even heart attack or stroke. But knowing your numbers and keeping them in healthy ranges can mitigate your risk of atherosclerosis and other heart conditions. First things first: Make an appointment with your healthcare provider to see how you’re doing. Learn your numbers and discuss how they may increase your personal risk of heart disease: Total Cholesterol Because cholesterol contributes to the buildup of plaque, keeping your numbers in check means keeping your arteries free of blockages. Check LDL (bad) cholesterol and HDL (good) cholesterol. Your body needs low levels of LDL, but not enough good cholesterol in your system can also increase risk. You can maintain healthy numbers by staying physically active and consuming a heart-healthy diet low in cholesterol and sodium. Statins, the class of drugs used to reduce LDL cholesterol, have proven so effective that the U.S. Preventive Service Task Force recommended in November that all adults older than 40 with one or more risk factors consider taking them. Blood Pressure High blood pressure places undue strain on your heart and arteries to move blood and oxygen throughout the body. And a heart that’s working too hard can lead to stroke, heart attack and heart failure. High blood pressure cannot be cured, but it can be managed by eating a heart-healthy diet low in alcohol, staying active and maintaining a healthy weight. Blood sugar Given that the body converts most of the food we eat into glucose, or blood sugar, for energy, adding sugar to the diet can raise blood sugar to unhealthy levels and damage the heart, increasing risk of cardiovascular disease and obesity. Opt for foods that are low in fat and added sugars and, instead, get your sweets in naturally occurring foods. Let added sugars be a treat and not the norm. Body Mass Index (BMI) Your BMI is used to determine whether you’re at a healthy weight. If you’re carrying extra pounds, the heart has to work harder, which increases risk of heart disease. Losing those pounds and maintaining a healthy weight reduces the burden on your heart and blood vessels and improves your blood pressure and cholesterol levels. So eat a heart-healthy diet and get active — even if you simply walk for 30 minutes a day. Because no symptoms indicate that you have poor cholesterol numbers, high blood pressure or high blood sugar levels, getting screened and learning your numbers is vital. Your doctor can determine what healthy levels look like for you individually and work with you to develop a plan for staying in optimum ranges. That plan will include heart-healthy eating, exercise, abstaining from smoking and, in some cases, medication. It’s up to you to stick with that plan between doctor visits. Do it for yourself, but consider making a pact for a more heart-healthy, active life with a buddy. Research shows people stick with exercise plans longer when they have a partner. This article also appeared in the Reno Gazette-Journal’s Health Source Aug. 27.
-
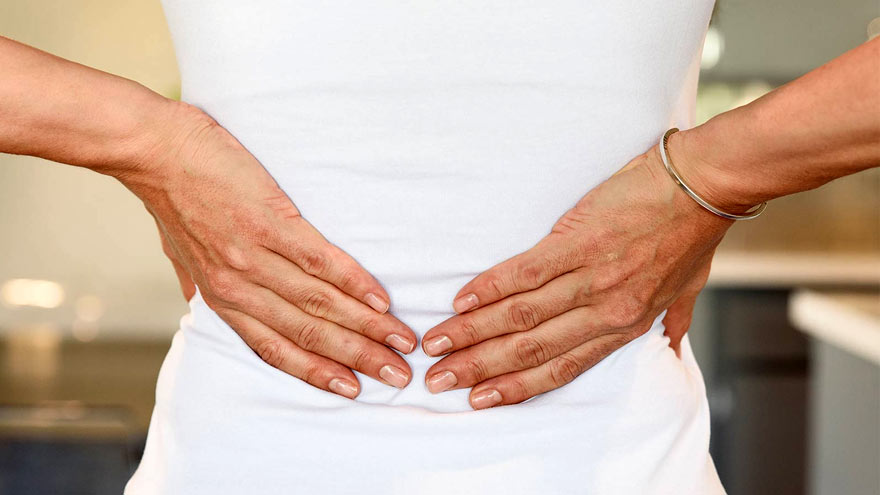
Low Back Pain – How to Stop the Ache
Low back pain is not only a problem most people have at some point in life, but also the leading cause of disability in the U.S. Whether it is a sharp spasm from lifting something heavy or a daily constant ache, there are various treatments available to relieve your pain. Jessica Ryder PT, DPT, cert VRS, with Renown Health Outpatient Therapy, explains some common causes of this pain, how to treat it and ways to prevent pain flare-ups. It’s important to realize most cases of low back pain are short term. Frequently lasting only a few days or weeks. In general these cases leave no long-term damage to the spine, muscles, discs or nerves. “However, it can become episodic or chronic (lasting longer than 12 weeks) if it is not properly understood or managed by the individual, ” cautions Ryder. Causes of Pain Specifically back discomfort can be related to: Wear and tear on the spine due to age or poor movement patterns Injury to spinal discs Sprains (overstretching or tearing of ligaments) and strains (tears in tendons or muscles) Trauma Irregularities of the spine present at birth (example: scoliosis)Notably the above issues may result in a “pinched nerve” or sciatica, causing pain to extend down the leg. Risk Factors for Pain In particular, your chance of developing low back pain increases with the risk factors below: Age Being overweight Low fitness level or occasional physical activity (“weekend warrior”) Family history Pregnancy Poor posture Jobs requiring heavy physical work (landscaping, plumbers, construction, etc.)
-
Cervical Cancer Screenings Can Reduce Risk of Cancer
According to the American Cancer Society, approximately 14,100 new cases of invasive cervical cancer will be diagnosed, and 4,280 women will die from cervical cancer. However, cervical cancer is preventable with regular screening tests and the HPV vaccine. It’s important to note that medical advances have allowed progress in diagnosing and treating cervical cancer. While it used to be one of the most common causes of cancer death for American women, the incidence of death has significantly declined. What to Know About the HPV Vaccine HPV vaccination is the best way to prevent cervical cancer and is recommended for all youth starting as early as age 9, or for teens and adults up to age 45 who didn’t start or finish the series. In Nevada, only 50.1% of teens ages 13-17 have been vaccinated for HPV. There are 13 types of HPV, and the vaccine Gardasil 9 protects against 9 of those HPV strains, greatly reducing the incidence of cervical cancer among vaccinated individuals. What to Know About Cervical Cancer Screenings The CDC says the most important thing you can do to help prevent cervical cancer is to have regular screening tests starting at age 21. And there are two common tests that can detect early stages of cervical cancer (or precancer) and improve health outcomes. The pap test (or pap smear). This screening looks for precancers. Women should begin getting pap smears when they’re 21. The human papillomavirus (HPV) test looks for the virus that can cause these cell changes. Cervical Cancer Screening Schedule The American Cancer Society offers the following guidelines for screenings: All women should begin cervical cancer screening at 21. Women between 21 and 29 should have a pap test every three years. Beginning at 30, the preferred way to screen is with a pap test combined with an HPV test every five years. This is called co-testing and should continue until age 65. A pap test (or pap smear) is performed during a regular screening appointment to look for precancers, cell changes on the cervix that might become cervical cancer if they are not evaluated or appropriately treated. Typically outpatient procedures can reduce the risk of long-term health impacts that prevent pre-cancerous cells from becoming cancer cells. Women over 65 who have had regular screenings in the previous ten years should stop cervical cancer screening as long as they haven’t had any severe precancers found in the last 20 years. How to Get Screened Request an appointment with your primary care physician or OBGYN to schedule a screening.
Read More About Cervical Cancer Screenings Can Reduce Risk of Cancer
-
Getting to Know Stephanie Kruse
There are a lot of impressive titles you can use to describe Stephanie Kruse: entrepreneur, marketer, philanthropist, leader, adventurer, nurse. And now with her planned gift to the Renown Health Nursing Excellence Endowment, she can add one more to the list: a member of the Renown Legacy Society – a group of visionary supporters who have chosen to make a lasting commitment to the future health and wellbeing of northern Nevadans. This generous planned gift comes on the heels of a significant cash gift made to the Nursing Education Fund last summer. Stephanie is an inspiring example of someone who has dedicated her life to helping others. The daughter of a nurse and a retired nurse herself, Stephanie knows the hard work, selflessness and dedication it takes to create a successful business and community. As Chair of the Renown Health Foundation Board of Directors, she also understands the importance of attracting and retaining nurses within a healthcare system. As a way to contribute to a cause near and dear to her heart, she decided to include the Renown Nursing Excellence Endowment as a beneficiary of her retirement plans. “I wanted to honor the memory of my mother, who was a registered nurse in a small-town hospital in Iowa.,” said Stephanie. “I was always very conscious of her passion for providing great care to her patients, and I wanted to provide funding for others interested in nursing.” Across the nation, health systems are facing a shortage of nurses and nursing-related professionals. Renown is proactively implementing programs to build our pipeline of potential future nurses and keep those already in the field. Stephanie’s generous gift will help the endowment provide programs such as training, scholarships, loan repayment and professional development to increase retention and recruitment of prospective nurses. “As nurses, we are entrusted with our patients’ lives,” said Melodie Osborn, Chief Nurse Executive at Renown Health. “We have the privilege of caring for people in their most vulnerable time and helping those who cannot help themselves. Stephanie’s generous gift to the Nursing Excellence Endowment Fund will help us develop new nurses for the future so we can continue to provide care to those in need for generations to come.” No Stranger to Healthcare Long before she found herself leading the Renown Health Foundation Board, Stephanie learned the ins and outs of healthcare. She graduated from nursing school and became a part-time nurse in a Sioux Falls, South Dakota nursing home while attending Augustana College to obtain a degree in journalism and a minor in theater. As part of her journalism program, Stephanie completed an internship in the public relations department of a Sioux Falls hospital, and that led to her accepting a position as director of public relations at a sister hospital. She later was recruited by Saint Mary's Hospital and moved to Reno to be the director of marketing in 1981. She stayed at Saint Mary's for almost 10 years before starting her own company in pursuit of her passion for marketing strategy. Since launching her brand, Stephanie has grown KPS3 to a multi-million-dollar firm with more than 60 staff members. Somehow, she is still able to find time to serve on six (!) volunteer boards, most of which are dedicated to improving access to better health and human services. “I have a soft spot in my heart for organizations who strive against all odds to help those with the greatest needs,” said Stephanie.
-
Why are Annual Exams & Routine Screenings Important?
March is Colorectal Cancer Awareness Month, and we want you to receive the best preventative care possible. Early detection can help prevent serious illness, yet many people still choose to skip their annual exams and routine screenings. Bonnie Ferrara, MD, MPH, Section Chief for Primary Care at Renown Medical Group, further explains the importance of this simple, easy way to stay healthy. Why are annual exams so important? The benefits of early detection and prevention to save lives and reduce the impacts of disease have been proven. These exams are the perfect opportunity to get your health questions answered. “This is your chance to sit down with your provider and talk about your overall health and your family’s health history as well as your concerns for the future,” says Bonnie Ferrara, M.D., family medicine. “It’s the opportunity for your provider to talk with you about your lifestyle, tobacco use, exercise and alcohol use, all of which make a difference in your future longevity.” The annual wellness exam is also an ideal time for most adult patients to discuss health screenings. In addition, these visits are the perfect time to address issues that may not directly relate to a particular medical problem or immediate illness. A good rule of thumb is to schedule these appointments around your birthday each year to make sure you and your provider are both updated on your care. Why would you need an annual exam if you aren’t feeling sick? According to Dr. Ferrara, seeing your care provider when you aren’t sick is one of the best times. “It is better if you try to arrange this visit when you are not feeling ill,” she says. “It is an opportunity to talk about wellness. Not only how to contribute to your wellness but also the changes that you can make that will make huge dividends in the future for your wellness. In addition, it allows us to do some education about what to expect in the coming years as far as your health and lifestyle changes.” What can you expect at an annual exam? Annual exams usually check your: History – lifestyle behaviors, health concerns, vaccination status, family medical history Vitals – blood pressure, heart rate, respiration rate and temperature General appearance – your care provider can find out a lot about you just by watching and talking to you Dr. Ferrara adds, “If this is a Medicare annual wellness exam, it is an opportunity to talk to your provider about depression and dementia as well as be tested for those.” You can also leverage your annual exam to speak to your provider about managing your chronic health problems. "As a provider, these visits give us the opportunity to hear how the medications and lifestyle changes we have recommended are working and if you are having problems with these, we have the opportunity to make suggestions of how to do things better for the future," Dr. Ferrara.
Read More About Why are Annual Exams & Routine Screenings Important?
-
Life-Saving CPR: Are Your Skills up to Date?
If CPR (cardiopulmonary resuscitation) is performed in the first few minutes of cardiac arrest, a person’s chance of survival can double or even triple. Troy Wiedenbeck, MD, cardiologist with the Renown Institute for Heart & Vascular Health, explains how you can be ready to perform it in case of an emergency. According to the American Heart Association, over 350,000 out-of-hospital cardiac arrests occur in the U.S. This highlights the importance of CPR to everyone, not just medical personnel. Most people do not have heart trouble at a hospital or fire station, they have it going about their everyday lives. And when someone has a heart attack outside of a hospital, their survival often depends on receiving help from a bystander. Signs of Heart Trouble First, how do you know when someone is experiencing cardiac arrest? The signs and symptoms of cardiac arrest are immediate and drastic, including: Sudden collapse No pulse Not breathing Loss of consciousness And sometimes, patients can experience symptoms beforehand, such as fatigue, fainting, blackouts, dizziness, chest pain, shortness of breath or vomiting. CPR Change Many of us know CPR as both mouth-to-mouth and pumps to the chest, but the rule now is hands-only. Can you explain the change? Hands-only CPR is exactly what the name says -- it's CPR without mouth-to-mouth. The American Heart Association recommends using only your hands. So if you see someone suddenly collapse, it’s recommended to call 9-1-1 and push hard and fast in the center of their chest. Doing this will get blood flowing back to the brain, lungs and other organs for someone having heart problems. Performing CPR on Adults vs. Children Hands-only CPR is just as effective as mouth-to-mouth and chest compressions for teens and adults who may have gone into cardiac arrest. Remember, it’s important to act fast. First, call 9-1-1 and then start chest compressions right away. If you perform CPR on someone within the first few minutes, it can double or triple their chance of survival. Keep in mind, for infants and children younger than 12 years old, regular CPR with mouth-to-mouth, as well as chest compressions, is still recommended. Two Steps to Save a Life If you see a teen or adult suddenly collapse follow these two steps: Call 911 so care providers can begin to respond. When calling 911, be specific about your location, especially if you are calling from a cell phone. Knowing the street address, building, floor and closest entry point can save precious time for first responders. Answering the dispatcher’s questions will make sure help arrives fast, and at the correct location. Push hard and fast in the center of the chest. The goal during CPR is 100 to 120 compressions per minute, about the same tempo as the song “Stayin’ Alive,” or “Thriller.” For hand placement, it’s also important to put the heel of your hand on the center of their chest and place the other hand on top. Push down on their chest at least two inches. It may seem severe at the time, but pushing this hard can truly save a life. Continue performing compressions as long as possible. If you tire, have someone take over compressions, if possible, and take turns until medical help arrives. For information on a CPR course in Reno, please contact REMSA at 775-858-5700.
Read More About Life-Saving CPR: Are Your Skills up to Date?
-
Addressing the Threat of Workplace Violence in Hospitals
In recent years, workplace violence against healthcare workers has been on the rise. According to the Occupational Safety and Health Administration (OSHA), about 75 percent of nearly 25,000 reported annual workplace assaults occur in healthcare and social service settings. Those who don’t work in healthcare may be surprised to learn that violent altercations are so common in our field. Hospital settings can create fear and stress for patients and their families. Pain, mind-altering medications and drugs, and difficult prognoses can amplify these feelings. While inappropriate responses may be understandable, violence cannot be tolerated. As the leader of a health system, protecting our employees is an issue that I take seriously. Reporting Workplace Violence Unfortunately, sometimes employees don’t report dangerous incidents fearing they might be blamed, or not realizing it’s a reportable offense. At Renown Health, we take these events seriously. We have clear, mandatory policies and protocols for reporting and investigating violent incidents. Each incident is investigated to ensure follow through and accountability. We also teach de-escalation skills to our hospital security teams, clinicians, and other frontline employees. As an added layer of protection, Renown Health has a first-rate security team that closely monitors activity on our campuses, addressing potential issues before they escalate. Our organization values our partnerships with community organizations including local law enforcement agencies like the Washoe County Sheriff’s Office and the Reno Police Department. Renown Health maintains a close relationship with these partners, and we alert them when our care teams experience an increase in violent incidents. I also recognize that workplace violence is a national problem that demands collaborative solutions. That’s why I am also proud to serve as a member of the American Hospital Association’s Hospitals Against Violence Advisory Committee. Nurses, doctors, paramedics, and frontline health workers care for us every day. It’s our responsibility to support them by ensuring they feel safe at work.
Read More About Addressing the Threat of Workplace Violence in Hospitals
-
Have a (Healthy) Heart: Maintain Your Blood Pressure
Do you know your blood pressure numbers? Dr. Michael Bloch explains how maintaining healthy numbers are important for good quality of life and increasing longevity. High blood pressure, or hypertension, affects 85 million Americans – that’s one in three people. Left untreated, it can lead to serious and sometimes life-threatening health concerns such as vision loss, kidney disease, heart failure, heart attack and stroke. But what is it, exactly, what makes it go up and why is that increase in pressure so dangerous? All About Blood Pressure In order to function properly, your body requires a continual supply of oxygen rich blood, which is goes to organs and tissues via blood vessels called arteries. Your beating heart produces the force (or pressure) your vessels require to move blood. This is your blood pressure. Your blood pressure numbers reflect two forces at work – the pressure created as blood is pumped throughout the body (systolic) and the pressure when your heart is at rest in between beats (diastolic). A normal, healthy reading shows a systolic level at 120 or below over a diastolic level of 80 or less: 120/80. An increase in pressure occurs slowly over time, straining the circulatory system and forcing the heart, blood vessels and tissues to work harder. This friction damages blood vessel walls and lets plaque buildup from LDL cholesterol, setting the stage for hardening of the arteries. As more and more plaque builds up, your blood vessels narrow, further raising blood pressure, damaging the circulatory system and increasing your risk of serious health conditions. The Silent Killer High blood pressure is known as a “silent killer,” as most people with it have no symptoms. In fact, one in six of those affected don’t even know they have the condition. That’s why it’s so important to know your numbers. The only way to find out if you have high blood pressure is to have it measured, either by a health professional or using a home monitor. If your numbers are high, there are things you can do to help lower it – it is treatable, but not curable. You can manage it with medications and lifestyle changes including: Adhering to the Mediterranean diet Decreasing sodium intake Avoiding excessive alcohol consumption Increasing exercise and activity levels Losing weight Prevention and Genetics Even better? High blood pressure doesn’t just happen. You can prevent the condition altogether. How? Know your numbers and know your risk. Look at your family medical history. Genetics certainly increases the risk of it, but those same lifestyle choices that can improve poor blood pressure can also prevent you from developing it. So if your numbers are good, keep them that way – eat well, move your body, maintain a healthy weight and drink alcohol in moderation.
Read More About Have a (Healthy) Heart: Maintain Your Blood Pressure