Search
-
Air Guard RN Makes an Impact in Community and Beyond
Everyday, Renown salutes its more than 150 active military and veterans on staff. Becca Gilbert, a Renown trauma nurse, is an example of the many outstanding service members at Renown who are serving both their country and their community. Becca Gilbert, BSN, RN, wears many uniforms. When she’s not wearing scrubs in her role as a trauma nurse in the intensive care unit of Renown Regional Medical Center, she’s wearing fatigues as a first lieutenant in the Nevada Air National Guard. “Service is huge,” says Becca Gilbert, RN, of her role in the Air Guard. “It’s something that is ingrained in me and a big part of who I am as a person. I find a lot of pride in being a part of something that is bigger than what is going on in my world.” Renown Health was named one of 15 recipients across the nation — and the only health system in the U.S. — for the Department of Defense’s highest employer award, the Secretary of Defense Employer Support Freedom Award, for exceptional support of its military employees. The Employer Support of the Guard and Reserves and Renown held a ceremony June 29 to recognize the award and to honor representatives of Renown who currently serve in the Guard and Reserves. With her Air Guard background, Gilbert is preassigned veteran patients at the Renown ICU. She says she’s able to relate to the veterans and their families and create a quick bond with them. “I’ve been assigned patients who are guard members with traumatic injuries — it’s good but hard,” Gilbert explains. “But I really love working with patients who are veterans.” Gilbert’s first career was as a veterinarian technician. Then enlisted in the Nevada Air National Guard in August 2008 — following in her father’s footsteps — and trained to serve as an EMT. While she was a medic, she went to nursing school for her second bachelor’s degree and was able to commission as an officer after graduation. Serving Our Community Gilbert says her work in the guard offers benefits that help with her job responsibilities at Renown, where she’s worked for four years. “At Renown, we are really a team and rely on each other to make sure there are good outcomes,” she says. “In the guard, officers are often put in charge, which teaches you a lot of things — organization, decision making and thinking of others. I think all of those things go hand-in-hand with my role as a nurse, especially in the ICU. People in the guard count on you as an officer and leader, and that is really important in the ICU when patients are counting on you for a positive outcome.” Gilbert’s responsibilities in the guard vary, including training for disaster relief missions and ensuring service members are fit and healthy enough to perform their jobs. “Training is a large part of the military — trauma training, physical fitness training and staying current on certifications,” she says. Locally she also leads the Self Aid Buddy Care program, a United States Air Force program that encompasses basic life support and limb-saving techniques to help wounded or injured personnel survive in medical emergencies until medical help is available. With the guard, Gilbert has also been involved in a bleeding-control program for volunteers in the community. She teaches community groups how to stop bleeding if they are a bystander to a car accident or other type of event, and is working with Renown trauma surgeon Marty Bain, M.D. to implement the program at Renown as well. Making a Difference Abroad In January, Gilbert was presented with an opportunity through the Nevada Guard State Partnership Program to travel outside the United States to the Kingdom of Tonga in the South Pacific and work at the Women and Children Crisis Centre, which assists families who are dealing with domestic violence. Gilbert praised the women who work at the center for their efforts towards change, as she says domestic violence is common in Tonga. “The women who work at the Women and Children Crisis Centre are pioneers,” she says. “They are trying to make changes by documenting what is going on and providing statistics to the lords and kings of Tonga. Some of it still isn’t accepted, but they continue to help the women and children of Tonga. They are helping so many people.” Renown Health salutes Gilbert for her tireless service to her country and her community here at home.
Read More About Air Guard RN Makes an Impact in Community and Beyond
-
Baby's Ears and Altitude Changes
One of the best things about living in the Reno area is the beautiful mountain range that surrounds our city. Many families take advantage of the activities the mountains have to offer or travel over them to visit friends and family in neighboring areas. However, for parents of infants there is often angst over your baby’s ears and altitude changes and the associated potential for ear pain and/or “popping.” Fortunately, there are things you can do to protect your infant’s ears the next time you drive over the mountain or hop on a plane with your little one. Baby’s Ears and Altitude Changes: What Causes Them to “Pop” The simple answer is pressure. The problem originates in the middle ear where there is an air pocket that is vulnerable to changes in pressure. The Eustachian tube, which runs behind the nose to the middle ear, is constantly absorbing and resupplying air to this pocket to keep it balanced. When the pressure is not balanced, your ears feel “clogged” or like they need to “pop.” In some cases this sensation can cause significant ear pain and even temporary hearing loss. Rapid changes in elevation or altitude, like driving over a mountain, or ascending or descending on an airplane, can cause rapid changes in pressure. In order to avoid problems, the Eustachian tube needs to open widely and frequently to equalize those pressure changes. The problem often intensifies during descents as you go from an area of lower atmospheric pressure to an area of higher atmospheric pressure. This is why you hear babies screaming on planes during descent or why your infant is wailing in the car seat as you head down the mountain. What can you do to make it a more comfortable trip for your child? First, be prepared. Babies cannot intentionally “pop” their ears like adults can, but we can help them by encouraging them to swallow. Offer your baby a pacifier or bottle while making ascents and descents. If possible, it may be helpful to have an adult ride in the back seat with baby if you’re in the car to ensure this can happen. Don’t let your baby sleep during descent on a plane. Help your little traveler out by offering him or her a pacifier during this process, as descent is the most likely time for pain associated with altitude changes. If your baby is congested prior to travel involving altitude changes, seek the advice of your pediatrician since they may have other solutions, including medications such as decongestants. If you return from a trip and notice your infant is still fussy and uncomfortable, contact your child’s doctor for a thorough ear evaluation. Safe travels!
-
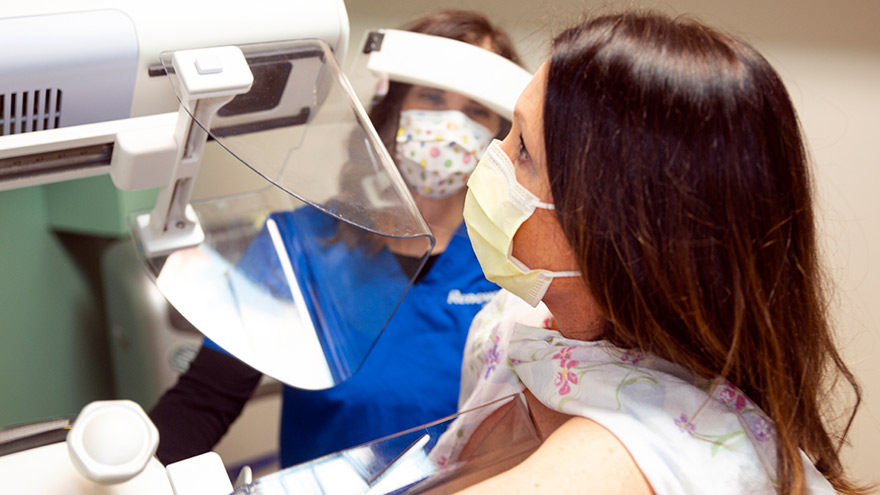
3D vs Whole Breast Ultrasound Which is Right for You
Breast cancer is the leading cause of cancer deaths in women in the U.S. That’s why early detection is so important. Dr. George Krakora, a radiologist with Renown Institute for Cancer, explains what to watch for and how new technology can lead to early detection. Most women know the importance of breast health and staying current with annual breast exams, but may not know that both screening guidelines and technology is evolving. So we asked George Krakora, MD, a radiologist for the Renown Institute for Cancer, what every woman should know about breast cancer detection and which screening method is right for them. First off, when should women start getting breast exams? Generally, women should start getting breast exams using mammography or ultrasound after they turn 40 years old. But we also want women ages 18 to 39 to talk to their primary care provider and ask for what’s called a formal risk assessment to see if screening is needed sooner. And you want to make sure your care provider is giving you a breast exam starting at age 25. It’s also a good idea to be familiar with how your breasts look and feel so you can report any changes to your care provider. What are the risk factors for breast cancer? Are there any preventive steps women can take? There a few risk factors you can’t control, like your age, family history of breast or other cancers, and if you have dense breast tissue. Your risk for breast cancer increases as you get older, and most breast cancers are diagnosed after age 50. Knowing your family history is important because a history of cancer and shared lifestyle can raise your risk. Your breast density can also increase your risk: Women with high breast density are four-to-five times more likely to get breast cancer than women with low breast density. But the good news is there are quite a few things you can do to prevent breast cancer, like not smoking, watching your alcohol intake, and maintaining a healthy weight with good diet and exercise. There are a lot of newer screenings out today. What is the difference between 2-D and 3-D mammography? In a 2-D mammogram, the tech takes X-rays of the breast. These pictures can show the radiologist if there are any lumps or tumors you might not be able to feel. In 3-D mammography, the process is largely the same but more X-rays are taken and it takes a few seconds longer for each image. This kind of exam detects 41 percent more cancers and reduces the number of false-positive results given to patients. This improvement in technology is great for both patients and their care providers. 3-D mammography provides better images of the breast, which allow doctors to more clearly diagnose and avoid false positives, especially in women with dense breast tissue. And what about a whole breast ultrasound. What is that? A whole breast ultrasound uses sound waves to detect cancerous tumors in the breast without using any radiation — it’s an ultrasound just like pregnant women get to check up on their baby. And the exam only takes about 20 minutes. We recommend these exams for patients whose mammograms have shown that they have dense breast tissue. Dense breast tissue can make it harder for doctors to see any abnormalities, lumps or tumors in a mammogram, so this technology ensures better early detection.
Read More About 3D vs Whole Breast Ultrasound Which is Right for You
-
Handmade Bracelets a Labor of Love for Cancer Patients
The road through cancer treatment can test even the toughest of spirits. A local organization is handcrafting and donating beaded bracelets to the courageous women who have reached the finish line at Renown Infusion Services. After finishing her sixth and final cycle of chemotherapy at Renown Infusion Services, Joan Jackson told her nurse, Daun Russell, RN, she was tired. Russell returned with a box and opened it -- as she does for all cancer patients completing treatment -- and said, “pick one.” What Jackson was selecting was a beautiful, handmade bracelet crafted and donated by the local Soroptimist organization. Jackson picked a purple bracelet with a tag that read, "Congratulations on completing your treatment. Imagine what you can do now." “Picking the bracelet was such a special thing to mark my last day of chemo,” Jackson says. "Their gesture impacted me for the good after going through so much.” The women behind the bracelets Bev Perkins, a member of the Soroptimist International of Truckee Meadows, says the bracelet project began in 2009 as a way of celebrating those who completed cancer treatment. She wanted the project to be hands-on, so she involved the club members by organizing a small budget and asking others to donate jewelry. The group comes together each year to make the bracelets. Perkins disassembles the donated jewelry, adding newly purchased beads to make kits for the bracelets. The volunteers also add a metal tag inscribed with an inspiring word, like “believe,” “hope” or “love.” “It’s a labor of love for us,” says Kay Dumhan, group treasurer. “It’s to show empowerment and to help these women know there are people who are encouraged by them.” “When bracelets are donated there is usually quite a bit of feedback on how much it’s appreciated,” Dumhan says. “We never want to run out so we make sure we have a supply there. We’ve had cancer survivors as members and that makes it all the more personal.”
Read More About Handmade Bracelets a Labor of Love for Cancer Patients
-
Learn How to Spot Asthma in Children and How It Is Treated
Sometimes, children’s asthma masks itself in symptoms that can be similar to other common respiratory problems. Dr. Shipra Singh of Renown Medical Group – Pediatrics discusses some diagnoses and treatments for asthma in children. Adults can easily recognize when we are out of breath or struggling to breathe, but what if you noticed this regularly happening to your infant or child during their daily play? Would you think they might have asthma? It may be difficult to tell if your small child has asthma because the symptoms can be similar to other common respiratory problems (bronchitis, croup, pneumonia) or even allergies. Read on to learn how to spot and manage asthma in your infant or child with advice from Shipra Singh, M.D., MPH, Pediatric Pulmonologist at Renown Medical Group – Pediatrics. According to the Centers for Disease Control, asthma in children is a leading chronic illness and cause of school absenteeism in the U.S. Asthma is a multi-factorial disease. Smoking during pregnancy or a family history of allergies or asthma has been linked to a greater chance of developing childhood asthma. Asthma is usually on a spectrum and not a single disease. It can range from mild to severe. Because an infant’s or toddler’s airway is smaller than in older children and adults, even a slight blockage caused by mucus or a restricted airway due to swelling can make breathing hard for them. In children five and younger, one of the most common causes of asthma symptoms is a respiratory virus, which narrows the airways in the lungs. These include a cold, the flu, bronchitis, pneumonia and other illnesses. How can I tell if my child has asthma? Unfortunately small children are unable to describe their symptoms, making asthma difficult to diagnose. Your child may even be active, playing and smiling, although they are experiencing chest tightness or labored breathing. Observe your child and let the child’s doctor know if: Your child’s breathing behavior has changed (coughing, wheezing, rapid breathing) Your child’s breathing pattern changes (day vs. night, with rest or activity, inside vs. outside) You have a family history of asthma or allergies Your child’s breathing is triggered by any foods or allergies With your help, your child’s doctor can make the best diagnosis to determine if your child has asthma. A pediatric pulmonologist (lung specialist) or pediatric allergist may also have to be consulted for special testing. Tests may include lung function testing, allergy tests, blood tests and X-rays for an accurate diagnosis. What is the treatment for infants and toddlers? Young children can use many of the same medications as older children and adults, although the way they take them and the dosage will differ. A nebulizer (or breathing machine) creating a medicated mist for your child to breathe through a mask may be used. An inhaler with a small spacer tube connected to a mask is also common to help your child breath medication into their lungs. Either of these options are effective. Asthma in children is treated with both fast-acting and long-term medicines to open up airways quickly for easy breathing and also to lessen asthma symptoms over time. Communicate with your child’s medical providers to create a personalized asthma management plan for them. How can I manage my child’s asthma? Recognize your child’s breathing habits and be aware of worsening symptoms. Consult with your child’s doctor on a daily asthma action plan to recognize worsening symptoms and track medications. (Here’s an example of an asthma action plan provided by the U.S. Department of Health and Human Services’ National Institutes of Health). Be consistent with the plan and talk to your doctor before changing it. Have an emergency plan in case of a serious asthma attack. Know where the closest ER is and know who can take care of your other children. Also know what the medical treatment coverage is under your insurance plan. We asked Dr. Singh about asthma in children: “Discussing asthma with your child may be a difficult subject. Some kids find the subject frightening or confusing. Others, especially the older kids, may be resentful of the treatment and may not be interested in doing the treatment. Talk to your doctor about advice to build an open and trusting relationship regarding your child’s asthma care.” What can I do to reduce my child’s asthma? Know your child’s asthma triggers (dust, pets, pollen, etc.) Follow your asthma action plan Keep your child away from smoke Can my child outgrow their asthma? Asthma symptoms change day to day and year to year. An older child can better recognize and manage their symptoms, so asthma episodes may lessen. However asthma is a life-long condition of the airways, so it is important to always have an asthma action plan, even with occasional asthma events. Renown Health Pediatric Care | Same-Day Appointments: 775-982-KIDS Our team of pediatricians, specialists and nurse practitioners have specialized training in children’s healthcare needs. We see children from birth to age 18 for the following pediatric needs: Wellness and preventive visits Sick visits Immunizations Behavioral health Allergy Asthma Common cold Diabetes Asthma resources for parents: Asthma and Allergy Foundation of America Centers for Disease Control and Prevention
Read More About Learn How to Spot Asthma in Children and How It Is Treated
-
One Patients Story of Survival
Thanks in part to the care provided by Renown’s award-winning team of ICU nurses, Tony Mowatt is alive, thriving and engaged. Read his story — and learn about the exclusive Beacon Award of Excellence — below. The open road. The growl of the engine. The feeling of freedom. That’s what Oakland resident Tony Mowatt was enjoying as he drove up Highway 88 toward Reno for the semi-annual Street Vibrations event. But he wasn’t expecting to hit the diesel truck — or to fly off of his bike over 100 yards, skidding onto the side of the road. He was severely injured and in the midst of rural Nevada. He had crashed just outside Centerville, Nev., and was miles away from any critical care hospital. Having the only trauma center equipped to treat his serious injuries, Tony was flown to Renown Regional Medical Center and admitted to the intensive care unit (ICU). ICU Nurses Treat Patient, Support Family Tony’s girlfriend, Tasha Klubock, was notified by his friend that he had been taken to the hospital. She immediately drove from Oakland to Reno to see Tony at Renown. Her first night there was overwhelming and scary — nobody knew if Tony was going to survive. But the nurses helped Tasha cope with the initial shock. Caring for the patient isn’t their only job — they also care for the family. “They [the nurses] just kept coming in and checking on me,” she said. “Angela was so amazing that first night. I really just bonded to her, and I remember when the shift switched, I panicked thinking about who was coming on and wanting to meet the next nurse … But they all came to talk to me — I had updates from everybody. It was just amazing.” ICU Nurses Became Family Tony spent 32 days in Renown’s Sierra ICU, surviving a serious head injury, all with Tasha by his side. He and Tasha still stay in touch with Renown nurses. “Even though this was literally one of the most hideous, craziest things to go through,” Tasha said. “There was so much hope and they became such a family to me and I still think of that time fondly because of the nurses.” “I’m alive because they wanted me to be,” Tony said. And Tony and Tasha are now happily engaged and planning their wedding. Exceptional Care: Renown ICU Nurses Win Awards Renown’s ICU nurses provide care like this every day to countless patients — it’s so second nature to them that they forget how exceptional it truly is. But it’s certainly care like Tony’s that has earned them national recognition. The American Association of Critical Care Nurses awarded the Beacon Award of Excellence to the Sierra, Cardiac and Roseview ICUs. These are the only ICUs in Nevada to obtain this honor. The Beacon Award recognizes critical care nursing teams who exemplify excellence in areas like leadership, process systems, quality care, knowledge, learning and development, excellence in patient care and superior patient health outcomes. “I couldn’t have been more proud of what we’ve done to accomplish this,” said Nick Dovedot, Cardiac ICU nurse. “It represents who we are. Just a great group of individuals who all work together as a team to make our patients get better.”
-
How to Safely Store Breast Milk
Breast milk. It's often referred to as liquid gold. And fortunately, it can be safely refrigerated or frozen for later use, which can allow you to be a bit more flexible in your new routine with baby. Whether you're getting ready to return to work, planning for the chance date night out or just exclusively pumping, it's crucial to understand the guidelines for proper breast milk storage. Storing Breast Milk Use clean bottles with screw caps, hard plastic cups that have tight caps or nursing bags (pre-sterilized bags meant for breast milk). Be sure to label each container with the date the milk was pumped and your baby's name if the milk is going to childcare providers. You can add fresh, cooled milk to milk that is already frozen, but add no more than is already in the container. For example, if you have two ounces of frozen milk, then you can add up to two more ounces of cooled milk. For healthy full-term infants, milk can be stored as follows: Room temperature - six to eight hours (no warmer than 77°F, or 25°C). Refrigerator - up to five days at 32°-39°F (0°-3.9°C). Freezer– Varies depending on freezer type. Up to two weeks in a freezer compartment located within the refrigerator. Three to six months in a freezer that is self-contained (standard kitchen fridge/freezer combination) and kept at 0°F (-18°C). Breast milk should be stored in the back of the freezer and not in the door. Six to 12 months in a deep freezer that is kept at -4°F (-20°C). Be sure to leave about an inch of space at the top of the container or bottle to allow for expansion of the milk when it freezes. Thawing Breast Milk Place frozen breast milk in the refrigerator to thaw (about 24 hours) then warm by running warm water over the bag or bottle of milk and use it within the next 24 hours. If you need it immediately, remove it from the freezer and run warm water over it until it's at room temperature. Never microwave breast milk and do not refreeze it. Once your baby has started to drink from the bottle, you should use it within one hour. You may find that different resources provide different recommendations about the amount of time you can store breast milk at room temperature, in the refrigerator and in the freezer. Talk to your doctor or lactation consultant if you have any concerns or questions.
-
Cervical Cancer Screenings Can Reduce Risk of Cancer
According to the American Cancer Society, approximately 14,100 new cases of invasive cervical cancer will be diagnosed, and 4,280 women will die from cervical cancer. However, cervical cancer is preventable with regular screening tests and the HPV vaccine. It’s important to note that medical advances have allowed progress in diagnosing and treating cervical cancer. While it used to be one of the most common causes of cancer death for American women, the incidence of death has significantly declined. What to Know About the HPV Vaccine HPV vaccination is the best way to prevent cervical cancer and is recommended for all youth starting as early as age 9, or for teens and adults up to age 45 who didn’t start or finish the series. In Nevada, only 50.1% of teens ages 13-17 have been vaccinated for HPV. There are 13 types of HPV, and the vaccine Gardasil 9 protects against 9 of those HPV strains, greatly reducing the incidence of cervical cancer among vaccinated individuals. What to Know About Cervical Cancer Screenings The CDC says the most important thing you can do to help prevent cervical cancer is to have regular screening tests starting at age 21. And there are two common tests that can detect early stages of cervical cancer (or precancer) and improve health outcomes. The pap test (or pap smear). This screening looks for precancers. Women should begin getting pap smears when they’re 21. The human papillomavirus (HPV) test looks for the virus that can cause these cell changes. Cervical Cancer Screening Schedule The American Cancer Society offers the following guidelines for screenings: All women should begin cervical cancer screening at 21. Women between 21 and 29 should have a pap test every three years. Beginning at 30, the preferred way to screen is with a pap test combined with an HPV test every five years. This is called co-testing and should continue until age 65. A pap test (or pap smear) is performed during a regular screening appointment to look for precancers, cell changes on the cervix that might become cervical cancer if they are not evaluated or appropriately treated. Typically outpatient procedures can reduce the risk of long-term health impacts that prevent pre-cancerous cells from becoming cancer cells. Women over 65 who have had regular screenings in the previous ten years should stop cervical cancer screening as long as they haven’t had any severe precancers found in the last 20 years. How to Get Screened Request an appointment with your primary care physician or OBGYN to schedule a screening.
Read More About Cervical Cancer Screenings Can Reduce Risk of Cancer
-
Get Ready for Baby with Childbirth Classes
By taking our pregnancy and birth class, you will gain the tools necessary to have a safe and empowering birth experience for both you and your baby. Chris Marlo, Childbirth Educator at Renown Health explains why birth classes are important. For questions regarding classes or tours, contact Chris Marlo: chris.marlo@renown.org 775-982-4352 What is a Certified Childbirth Educator/Doula? If you are expecting a baby, Renown has a wide variety of classes to help prepare you for birth. Classes are taught by certified childbirth educators and doulas. A certified childbirth educator is a trusted resource who has a passion for educating expecting parents about childbirth, and will provide you with non-biased, evidence-based information. A doula is a professional labor assistant who provides physical and emotional support during pregnancy, childbirth and postpartum. As you prepare for birth, our certified educators will guide you each step of the way and ensure you receive the quality care you deserve. Why Should I Take Pregnancy and Birth Classes? For expecting parents, taking a childbirth education course is an important step in preparing for their new arrival. We cover topics such as labor and delivery, postpartum care, breastfeeding, nutrition, pain management techniques, and more. Our experienced instructors will provide you with the information you need to make informed decisions during your pregnancy and childbirth. With our classes, you can be sure that you have all the knowledge necessary to have a positive experience before, during, and after your baby’s arrival. Our classes will help ease your fears as we practice breathing, relaxation and the many tools you can utilize for birth. At Renown we understand that there is no right way to give birth, and our educators will offer a supportive environment where questions are encouraged, and everyone is respected. Childbirth Class Options: Baby and Family Suites Tour & Virtual Tour Breastfeeding Basics and Beyond Class Breathing & Relaxation Techniques for Birth Pregnancy and Birth – 5 & 7 Week Series Pregnancy and Birth Class Additional Resources: Baby Safe Class Babysitter Class Grandparents Virtual Class Infant CPR & Choking Class Newborn Care Nurturing Your Newborn Preparing for Postpartum Virtual Class
-
Building a Better Birth Team
Giving birth expends as much energy as running a marathon. And just like you would only run a marathon with training beforehand, there are exercises you can do to prepare for birth. But instead of a coach, you'll have your birth team. Your birth team exists to help you navigate pregnancy and labor and support your choices. Let's say you've never put together a birth team before and are wondering where to start. Today we'll go over the three main positions to fill for your birth team's starting lineup. Birthing Person The birthing person is the leader of the team. After all, you can't have a birth team without someone giving birth. This person could be the baby's mother, gestational surrogate, birth parent before adoption, a transgender father or a non-binary parent. If you are not the birthing person, don't presume to know what the ideal labor and birth circumstances should be. And if you are the birthing person, don't allow anyone else to tell you what you want. This is your body and your birth; you are the boss in the birth room. Doula No birth team is complete without a doula, and although doulas have increased in popularity lately, many people still don't know what a doula is. Simply put, a doula is a birth professional – not a medical provider – who offers emotional, physical and informational support during pregnancy, labor and beyond. Most doulas' services include at least one prenatal visit and one postpartum visit, as well as continuous care throughout active labor. Some doulas provide more than one prenatal/postpartum visit, so be sure to ask what is included in their fee. Even if you have a partner who will support you during labor, studies have shown that a doula can significantly increase your likelihood of a positive birth outcome. Even the most supportive partner needs to rest, and a doula can ensure that you still get the care you need while your partner gets a break. Midwife or Obstetrician Finally, you'll want to choose the medical professional who will attend your birth. Many folks choose to give birth with the OB/GYN who does their annual check-ups, but there are many reasons someone might choose a different provider for their birth. The first step to finding the best attending provider for your birth is to decide which model of care aligns closest to your values and goals: the Midwifery Model of Care or the Medical Model of Care. .tg {border-collapse:collapse;border-spacing:0;} .tg td{border-color:black;border-style:solid;border-width:1px;font-family:Arial, sans-serif;font-size:14px; overflow:hidden;padding:10px 5px;word-break:normal;} .tg th{border-color:black;border-style:solid;border-width:1px;font-family:Arial, sans-serif;font-size:14px; font-weight:normal;overflow:hidden;padding:10px 5px;word-break:normal;} .tg .tg-gqvw{background-color:#ffffff;color:#56266d;font-family:Arial, Helvetica, sans-serif !important;font-weight:bold; text-align:left;vertical-align:top} .tg .tg-8vim{background-color:#ffffff;color:#56266d;font-family:Arial, Helvetica, sans-serif !important;font-size:18px; font-weight:bold;text-align:left;vertical-align:top} .tg .tg-qm8j{background-color:#ffffff;color:#56266d;font-family:Arial, Helvetica, sans-serif !important;text-align:left; vertical-align:top} .tg {border-collapse:collapse;border-spacing:0;} .tg td{border-color:black;border-style:solid;border-width:1px;font-family:Arial, sans-serif;font-size:14px; overflow:hidden;padding:10px 5px;word-break:normal;} .tg th{border-color:black;border-style:solid;border-width:1px;font-family:Arial, sans-serif;font-size:14px; font-weight:normal;overflow:hidden;padding:10px 5px;word-break:normal;} .tg .tg-gqvw{background-color:#ffffff;color:#56266d;font-family:Arial, Helvetica, sans-serif !important;font-weight:bold; text-align:left;vertical-align:top} .tg .tg-8vim{background-color:#ffffff;color:#56266d;font-family:Arial, Helvetica, sans-serif !important;font-size:18px; font-weight:bold;text-align:left;vertical-align:top} .tg .tg-2rvk{background-color:#ffffff;color:#000000;font-family:Arial, Helvetica, sans-serif !important;text-align:left; vertical-align:top} Midwifery Model of Care Medical Model of Care Philosophy Birth is physiological. Birth is potentially pathological. Interventions Medical interventions can cause more complications, and therefore are only used as needed. Medical interventions should be used, even in non-emergency situations and sometimes as preventative measures. Decisions Birthing person is the key decision maker. Medical professional is the key decision maker. Provider’s Role Providers monitor labor and will intervene or transfer to hospital if needed. Providers assess and control the birthing process.
-
Department Spotlight: NICU Transport
Bringing in new life is an exciting and beautiful occasion. The possibilities for the newest members of our world are endless – what will the child grow up to become? What will they achieve in their lifetime? Anyone will agree that a new life is precious and protecting that life by any means possible is a necessity. Sometimes, however, a baby’s journey into our world brings along obstacles. Prematurity, congenital defects and other complications can accompany a birth and the baby’s first few moments of life. But what happens when these complications happen outside of a fully-functioning Labor & Delivery unit, or if the complications need a special level of intervention with a health system capable of caring for their unique needs? Enter the NICU Transport team at Renown Health. As the only Neonatal Intensive Care Unit (NICU) Transport team in northern Nevada, these dedicated nurses, respiratory therapists and neonatal nurse practitioners – who have normal unit duties of their own at Renown Regional Medical Center – step up to the plate to take on this extra duty to support members of their community facing some of the scariest moments of their lives. To them, transporting babies in critical condition and giving them the best chance of life isn’t just a responsibility; it’s a calling. The NICU on Wheels When the Saint Mary’s maternity unit, which was Renown’s partner in NICU transport duties, made the decision to close, our dedicated NICU nurses and respiratory therapists diligently rose to the occasion to fill the demand. Dubbed the “NICU on Wheels,” Renown’s team went from taking on transport duties every other day to 365 days a year – and they are always ready to go at a moment’s notice, whether it’s by ambulance or by fixed-wing aircraft. “When we learned about the closure we knew it was our calling and knew we had to step up,” said Rachel D., Neonatal Transport RN at Renown. “We still have regular days on the floor, and we each switch off being on-call for transport. Once we get a distress call, we have 30 minutes to get to the hospital, grab our gear and go. We have to essentially put a whole room’s worth of portable equipment in one bag.” “I really enjoy being a part of the transport team and making a difference from northern Nevada to northern California,” added Sam V., Supervisor of Respiratory Care at Renown. “We are able to practice at the top of our skill level and use autonomy that not every practitioner gets to use.” Each NICU Transport unit works in teams of three when heading out into the field: one nurse (our bedside experts), one nurse practitioner (our education experts) and one respiratory therapist (our lung and breathing experts). With several years – and in many cases, decades – of experience in NICU nursing, NICU transport duties and respiratory therapy, this team is poised to provide state-of-the-art lifesaving care en route to the hospital. This diverse array of experiences among the team especially comes in handy as they continue to face the increased transport workload. “We are so thankful to have Saint Mary’s employees come over and work on our team after their maternity ward closed,” said Melyssa H., RN, NICU Transport Coordinator at Renown. “Helping the babies, as well as helping the scared families, will always be our top priority.” “I love the complexity that babies provide in the NICU,” added Jennifer J., Neonatal Transport RN at Renown. “Providing hands-on care right at the bedside along other members of the team is such a rewarding experience.” Education is also a crucial tool in NICU care, especially in the field. The nurse practitioners on this team make it their mission to outreach to the community, including our rural health partners, and help them build the tools and skills they need to care for our smallest and most critical patients. “I have been on a few transports where we went out and did not have to bring the baby over to the hospital, and we were able to provide lots of education instead,” said Shiela A., Respiratory Specialist at Renown. “For instance, I was called out to Fallon for a baby that was in respiratory distress. When we arrived, we saw the baby was awake and active although intubated. The tube came out, and we retaped it. While we stayed to observe the baby to make sure everything was okay, the nurse practitioner on the team provided educational tools to the family on what they can improve on regarding their baby’s tubing. Our nurses do such a great job with these teachings.” “When I started, I quickly noticed that more education was needed in the field,” added Jennifer J., RN. “Now I see the momentum we’ve had in these communities really take full force. Because of this education, and the confidence we instill in our patients’ families, each baby’s transition to our team has become so much easier. It has been awesome to watch this progress over the years.” With immense experience, education and a strong commitment to their community under their wing, the NICU on Wheels is only just getting started. Teamwork Makes the Dream Work Running a successful NICU Transport operation, especially as the sole health system participating, takes a village. With only three professionals out in the field, the team leans on their fellow nurses, physicians, surgeons and specialists to make the operation run as smoothly as possible. From REMSA and Care Flight helping load patients in and get them to the hospital safely, to Renown’s Clinical Engineering team who are first on the scene when machines need repairs and troubleshooting, everyone rises to the occasion to achieve the best-possible outcome for our youngest patients at some of the most challenging moments of the beginning of their lives – and they are fully trusted to move those mountains. “Being a part of the NICU Transport team has given us the opportunity to facilitate a deeper, meaningful relationship with providers and a patient’s entire care team,” said Rachel D., RN. “They entrust us with our assessment skills, opinions and skill levels. There is an equal layer of trust between us and them.” Despite the pressure they feel every day, the NICU Transport team never let it overtake them and instead let it empower them. “We are under a lot of pressure and stress regardless of the case, and yet, we all work so well together; the teamwork really is incredible,” said Lisa A., Respiratory Specialist at Renown. “I am very proud of how our team steps up and is very intricate, even down to organization. For example, team members like Shiela arrange all the respiratory bags and make sure they are laid out in a way that makes the procedure as simple as possible to ensure there are no complications.” The nurses and respiratory therapists also partner together on the NICU floor and are always ready to provide coverage when their transport colleagues get a call. Committed to collaboration and ready to jump into action, the NICU Transport team works together to elevate each other and the bottom line for each patient. “This is a full-time gig, and the group works together to make sure everyone is covered; we are all very collaborative,” said Sarah K., Respiratory Specialist at Renown. “We all think of our patients as extra special, and it’s nice to know that you can make a difference in the baby’s life and the lives of the family. We all have a sense of purpose in giving back to the community.” “I am just so thankful to be a part of this team,” added Marcia A., Neonatal Transport RN at Renown. “We really have developed a strong bond.” A Track Record of Success The life-saving measures that each member of the NICU Transport team take surpass hospital walls. The impact they have on each baby are remembered and celebrated for years, and they often develop lifelong relationships with patients and their families after their stay in the NICU. One prime example of this can be found in an impassioned letter from Tess, the mother of a young boy who was in the midst of respiratory distress and needed immediate intervention. Because of the valiant efforts of Renown’s NICU Transport team, her child, Warren, is a healthy and happy baby to this day. She recalls the experience: Warren had stopped breathing while getting routine blood work. He was resuscitated twice while at an area hospital. We made the decision to transfer him to Renown for him to be admitted into the NICU. Within an hour and a half of this decision, Renown had sent a team consisting of a respiratory therapist, nurse and nurse practitioner to come and get him. As soon as the team entered the room, we immediately felt safe and comforted. The team made sure we knew exactly what was going on and what was going to happen in the following hours, and they let us know they would do everything for Warren. He was resuscitated two more times by the respiratory therapist while getting ready for transport. At that time, the decision was made to intubate for a smoother ride to Renown. We knew you all had his best interest in mind, and of course, we trusted you with everything. The intubation went well, and he was packed up and ready to drive. Today, Warren is hitting all of his developmental milestones and is a normal, happy baby in everyone’s eyes. We can’t thank the NICU Transport team enough for taking such good care of Warren and helping him Fight the Good Fight. “This success wasn’t just due to our three-person unit – our manager, Jason, also jumped in and drove all the way to Carson City to stabilize the child,” said Shiela A. “This just goes to show that no matter our title, we are always here to help and make a huge difference in the lives of our patients.” Success stories of children like Warren describe the common mission of the NICU Transport team in detail, and while there are more of these stories to come, the team is always ready to make the necessary sacrifices for the greater good of their patients. “Sarah K. is like Warren’s guardian angel,” said Tess. “We call her ‘Auntie Sarah’ now. He wouldn’t be here if it weren’t for her and the entire NICU Transport team. It takes a special kind of person to work in the NICU. I can never repay this team for what they’ve done for Warren and our family.” “I am proud of this team, their flexibility and the sacrifices they have made to do transport 365 days a year,” added Melyssa H., RN.” The remarkable success of the NICU Transport team serves as proof of the unwavering and tireless commitment of each and every team member, bringing hope to families during their most difficult moments. “NICU Transport forces you to be confident in yourself and your abilities and to push yourself a step further,” said Rachel D., RN. “I am a better nurse because I joined the transport team.”
-
Senior Care Plus Loves Pickleball
Senior Care Plus is pleased to announce we are now a proud sponsor of Jam On It Pickleball, open to the community seven days a week at the Reno Sparks Convention Center. We’re excited to help promote this fun activity to our members, employees and the public. Pickleball has many wonderful health benefits – particularly for seniors. It’s a low-impact game that raises the heart rate, improves hand-eye coordination and increases mobility. In addition to the obvious physical benefits, pickleball is a great social activity. Getting out of the house and playing a fun, easy-to-learn game with others is a great way to make new friends while improving your physical and mental health! Ralph Barbato, a Senior Care Plus member from Reno, is a huge fan of pickleball and all it has to offer. “Pickleball has made such a positive impact on my life. I love the physical and mental health benefits along with the social aspect – it’s a great way to meet new people and I’m excited to have it in our community,” said Ralph.