Search
-
Cancer Nutrition - Helpful Tips to Support Your Loved One to Eat Healthy
Eating healthy is a daily challenge for many, but for those with cancer it is an even harder struggle. A cancer diagnosis not only impacts those diagnosed, but family members and friends too. One key area of concern is making sure your loved one stays well by eating healthy food every day. Here are some essential cancer nutrition tips from Renown Health registered dietitians Jessica Blauenstein and Amy Laster. Help to Prepare Meals and Snacks for Daily Cancer Nutrition Make it grab and go. Easy-to-make meals help reduce the burden of having to cook and prepare food. Having easy to grab snacks on the counter or in the fridge can help ensure your loved one has access to those nutrients when needed. Sit outside of the kitchen. This allows your loved one to avoid cooking smells which can make them feel sick as a side effect of cancer treatments. Also try serving them cold foods such as sandwiches, cheese and crackers, or shakes which have a mild scent. Try drinkable meals. Some people with cancer find it easier to sip their calories over the course of 30 minutes to an hour. Consider smoothies or supplemental shakes such as Ensure Enlive or Boost Plus as snacks not meal replacements. A great foundation for a smoothie is a protein source (Greek yogurt, protein powder, nut butters or milk) with a carbohydrate (fruits, juice or berries). Add other ingredients as desired, such as spinach, kale, and ground flaxseed or chia seeds to give it more vitamins, minerals, and fiber. Snack Ideas for Those Undergoing Cancer Treatment The following ideas are both quick and easy to make for your loved one. Chicken or tuna salad with whole grain crackers or as a sandwich on whole grain bread Greek yogurt mixed with cereal, fruit and/or nuts Cottage cheese with banana, cinnamon and/or peanut butter Favorite fruit with 100% natural peanut or almond butter spread - Try peanut butter with bananas, apples, or even celery Their favorite veggies dipped in a salad dressing of your choice - For example, carrots with hummus or ranch dressing Cheese and whole grain crackers - Add tomato slices with a dash of oregano on top for more flavor Eggs scrambled with cheese, vegetables and/or salsa Peanut butter and jelly sandwich on whole grain bread A baked sweet potato with some favorite toppings Hard boiled eggs and/or egg salad with whole grain crackers, or as a sandwich on whole grain bread Oatmeal or cream of wheat prepared with milk, fruit and/or nuts Sometimes your loved one may not feel like eating or refuse to eat. If treatment side effects are impacting your loved one’s ability to eat, please visit the websites below containing recipes tailored to treat side effects. Cook for Your Life ELLICSR Of course you may also consult a registered dietitian and/or the patients care team, if you have more cancer nutrition concerns. No Appetite? Assisting with Cancer Taste Changes Taste changes are common during cancer treatment. Patients experiencing these changes may not feel like eating, which can negatively impact their nutrition. Help your loved one overcome taste changes with these cancer nutrition strategies: Metallic or bitter taste in food - add something sweet such as maple syrup, honey or jelly. You may also try adding fat, such as a nut butter, avocado or regular butter. Pickles or vinegar could help with this too. A taste like cardboard - try adding salt and extra flavor to foods with seasonings and spices. Some examples are onion, garlic, chili powder, basil, oregano, rosemary, tarragon, barbecue sauce, mustard, ketchup, or mint. Lemon juice, citrus, vinegar, or pickles may also help with this as well Food tastes too sweet - try adding six drops of lemon or lime juice. Add small amounts until the sweetness is gone. Very salty taste - try adding ¼ teaspoon of lemon juice. Try plastic utensils instead of metal, especially if your loved one is struggling with foods tasting metallic. Dipping small bites of food into either lemon juice or vinegar can have a “palate cleansing” feel and may improve taste perception. This helps avoid getting tired of the flavor after a few bites. Try marinating food or meats in sweet fruit juices, salad dressings, or sweet-and-sour sauce. Other “palate cleansing” foods are lime juice, orange juice, mangos, lemongrass, parsley, cilantro, mint, ginger, basil, and pickled foods. Use aroma to make foods appealing, avoiding any smells that may cause nausea. In particular, cinnamon, nutmeg, cloves, coriander, cumin, ginger, and black pepper can add an aromatic flavor. Also include herbs such as oregano, rosemary and thyme. Think texture. Consider trying wafers, crunchy nut butters, carrots, celery, cucumbers, chips, rice crispies, corn flakes, crackers, panko crumbs, nuts, or seeds if you are able to chew and swallow them safely. Remember that patience with your loved one's changing appetite and tastes can be the strongest form of support you can provide. Nutrition Tips for Cancer Survivorship and Beyond If eating large meals is difficult for your loved one, encourage them to snack throughout the day. Aim for 4-6 snacks or small meals per day. Focus on consuming 2-3 protein-rich foods each day such as lean animal meats, fish, eggs, soy or a protein supplement with 20-30 grams of protein per serving. Eat a variety of brightly colored fruits and veggies. Aim to make half of each meal fruits and vegetables. Eat less than 18 oz. (cooked weight) of red meat per week. Limit cold cuts, bacon, sausage, and hot dogs. Avoid excess salt and saturated fats. Cut back on simple carbs. (i.e. desserts, candies, white bread/pastas, french fries, packaged foods, chips) Drink in moderation- if at all- one drink per day for women, two for men. Get enough vitamin D (through diet and/or supplement) Avoid tobacco of any kind. Keep a healthy weight and stay up on exercise. Other Ways to Help a Loved One with Cancer Assist with Chores Allow your loved one to relax as you help take care of chores around the house, such as cleaning, cooking and grocery shopping. This may reduce overall stress and can be helpful for those that get tired after their treatments. Physical activity can still be beneficial, so be sure to do an activity together that they enjoy and is approved by their doctor. Be Patient It can be very difficult to see a loved one go through cancer treatment. Remember to be patient with your loved one. There may be things we want them to do or eat that we know would be good for them, however, meet your loved one with grace and understanding. It is ultimately their decision on what to do, just be there to support and assist them as they go through this challenging time. Additionally, Renown hosts free “Eating Well After Cancer Treatment” nutrition classes for cancer survivors. Our next cancer nutrition class series starts Thursday, June 3, 2021, and will be hosted virtually. It is open to anyone in the community. For more information or to register please click here.
Read More About Cancer Nutrition - Helpful Tips to Support Your Loved One to Eat Healthy
-
How You Can be a COVID-19 Vaccine Ambassador
We get it – the entire world has been overwhelmed with COVID-19 vaccine information, questions and celebrations around vaccines developed to combat COVID-19 induring the past several months. It’s hard to know where to start in digesting all this news and information. But one thing is clear: healthcare experts agree that the authorized COVID-19 vaccines are safe, effective and recommended to help end this pandemic. If you are passionate about stepping up in your community to encourage the vaccination efforts, we’re offering a few ideas on how you can be an ambassador. Find the Facts Content on the vaccine is abundant, but and there’s a few resources that we can all rely on to help digest the information: The Centers for Disease Control (CDC) updates its website content around the vaccine regularly, and also offerings information in Spanish. Health departments across the U.S. are leading the way in distribution logistics planning, and partnering with other providers, like such as hospitals and pharmacies, to distribute give people doses. Their websites are great resources to understand options where you live. Locally, check out washoecounty.gov/health/programs-and-services/environmental-health/covid-19-guidance for vaccine updates in Washoe County. Many providers like Renown Health and other providers are sharing content around their recommendations for the vaccine. Get answers about the vaccine types from one of our pharmacists, read common concerns addressed by experts and view videos from many doctors and other specialists on our YouTube Channel.
Read More About How You Can be a COVID-19 Vaccine Ambassador
-
Why Childhood Immunizations Are So Important
Immunizations (vaccines) save the lives of thousands of children and adults annually, protecting us from illnesses that can lead to disease, hospital stays, life-long complications and even death. Not only do immunizations protect the persons receiving the vaccine, but through herd immunity, vaccines protect children that are unable to get vaccines due to illness or age and our elderly community members whose immunities may have declined. Vanessa Slots, M.D., offers insight on the importance of immunizations. Immunizations Your Child Needs (and when) Birth to 6 Months Hepatitis B: Shortly after birth, first vaccine dose Diphtheria, Tetanus, and Pertussis (DTaP), Polio, Haemophilus Influenza (HiB), Pneumonia, Hepatitis B and Rotavirus: Ages 2, 4 and 6 months, boosters and vaccines One Year to 18 Months MMR and Varicella (chickenpox) vaccine: Age 1, first vaccine dose Hepatitis A, HiB and Pneumonia: Age 1, booster DTaP: 15 months, fourth vaccine dose Hepatitis, second dose: 18 months Flu Vaccine: 6 months and older, annually* *In the year after receiving their first dose, an infant will need a booster one month later. Four Years Old MMRV, DTaP and Polio, final dose: Four years of age Pre-Teen and Beyond Tdap and Meningitis: Before starting middle school, children receive these vaccines. They are also old enough to start the HPV vaccine, an essential vaccine for all young adults to protect against cancer, genital warts and cervical dysplasia.
Read More About Why Childhood Immunizations Are So Important
-
Dorm Safety and Bacterial Meningitis
Bacterial meningitis is probably the last thing on your mind as you help your child prepare for college. Buying books and stocking up on necessities may top your list, but it’s a good idea to ensure your student is up-to-date on their meningitis vaccine. How Bacterial Meningitis Spreads According to the Centers for Disease Control and Prevention, people living in close quarters are more likely to spread this illness to one another. For example, you may have heard about the higher risk of meningococcal (or bacterial) meningitis for new college students. The risk is so serious that many colleges and universities require proof of a vaccine for new students moving into campus housing. This includes the University of Nevada, Reno. To clarify, all incoming freshmen under 23 years of age must show proof of their up-to-date meningitis shot. “Bacterial meningitis is considered a medical emergency, and anyone with the signs and symptoms should be evaluated in the emergency room immediately,” says Vanessa Slots, MD, Renown pediatrician. Symptoms of Bacterial Meningitis Fever Nausea Vomiting Irritability Headache Confusion Back pain Stiff or painful neck Leg pain Light sensitivity Rash on the torso or lower extremities It’s important to know many of these symptoms for both bacterial and viral meningitis are the same. However, the viral type is more common, often clearing up in seven to 10 days without complications. Nonetheless, you should go to the emergency room to be looked at, as the signs are similar for both illnesses. Why is Bacterial Meningitis Dangerous? This illness moves quickly, and in some cases, it can seem like the flu or severe strep throat and take a few days to develop. Or, it can hit in just hours. “Bacterial meningitis has an overall death rate of 10 to 15 percent despite treatment with antibiotics,” Dr. Slots warns. Another critical point is problems after recovery can also be severe. Frequently these include brain damage, amputations, infections around the heart, seizures and shock.
-
More Than a Cold
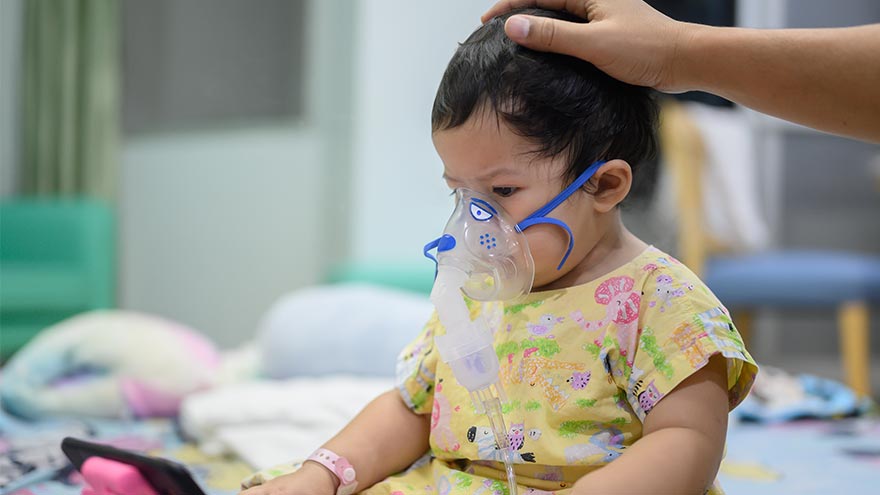
Respiratory syncytial virus, also known as RSV, is a common respiratory virus that impacts the lungs and breathing pathways. The virus can be dangerous for infants and young children and is also concerning for older adults. While most older kids and adults only experience cold-like systems and recover in a week or two, an estimated 58,000-80,000 children younger than 5 years old are hospitalized due to RSV each year, and in 2022 healthcare organizations across the country are experiencing higher infection rates than in years past. "RSV typically peaks in the winter, but this season we are seeing an earlier surge in cases,” said Dr. Vanessa Slots, the Division Chief of General Pediatrics at Renown. “Infants who are infected with RSV almost always show symptoms. Call your healthcare provider immediately if your child is having difficulty breathing, is not drinking enough fluids or is experiencing worsening symptoms.” Symptoms of RSV: Runny nose Decrease in appetite/inability to drink Dry diapers, an indication of dehydration Cough, which may progress to wheezing or difficulty breathing Irritability (most common in very young infants) Decreased activity (most common in very young infants) Decreased appetite (most common in very young infants) Apnea, pauses in breathing for more than 10 seconds (most common in very young infants) What to do if you think your child has RSV: Call your pediatrician! If you suspect your child might have RSV, consulting their healthcare provider is the best first line of defense. From here they will help you build an appropriate treatment plan for child. Keep in mind that many pediatrician offices offer 24/7 call lines. If your child is experiencing retracted breathing (when the area between the ribs and in the neck sinks in when a person attempts to inhale), dehydration (not drinking and decrease in wet diapers) or apnea (pauses in breathing for more than 10 seconds) please call 911 or go to the closest emergency room. Treating RSV from home: Clear your child's nasal pathway with a bulb syringe or saline spray/drops Stay home and rest Drink plenty of fluids to prevent dehydration Manage fever with fever reducers such as acetaminophen or ibuprofen Preventing the spread of RSV: Good news! The biggest RSV prevention tips are almost identical to what we’ve already been doing to prevent COVID-19 – so hopefully, these actions are already second nature. If you have young children or regularly encounter younger children, remember to: Wash your hands often Keep your hands off your face Avoid close contact with sick people Cover your coughs and sneezes Clean and disinfect surfaces Stay home when you are sick Get vaccinated against the flu and COVID-19 to prevent more serious co-infections RSV is dangerous for older adults, Too Older adults – especially those over 65 years old, have chronic heart or lung disease or a weakened immune system – also need to be hyper-vigilant about RSV. If you or your loved one is in the older adult at-risk group, remember to follow the above prevention measures and talk to your healthcare provider immediately if you suspect you have RSV. *Data courtesy of the Center for Disease Control and Prevention.
-
Prevention Against STIs Matters
According to the U.S. Department of Health and Human Services, there are more than 20 million estimated new sexually transmitted infection (STI) cases in the United States each year, with rates continuing to increase. What you may not know is most STIs are preventable. We talked with Renown Adolescent Medicine Specialist, Caroline Barangan, MD to learn more about STIs. How Can You Get an STI? The CDC (Center for Disease Control) says that STIs are acquired through sexual contact. There are bacteria, viruses or parasites that can cause an STI which may pass from person to person in blood, semen, vaginal and other bodily fluids. How Do You Know if You Have an STI? STIs can have a range of signs and symptoms such as: Warts, bumps or sores on or near the penis, vagina, mouth or anus Swelling, redness or severe itching near the penis or vagina Discharge from the penis Vaginal bleeding that’s not your period Painful or uncomfortable sex Vaginal discharge that has an unpleasant odor, causes irritation or is a different color or amount than usual Weight loss, diarrhea or night sweats Aches, pains, fever and chills Jaundice (yellowing of the skin and whites of the eyes) Painful or frequent urination Sore throat if you engage in oral sex It’s important to know that the majority of people who have an STI commonly have no symptoms at all, which is why it’s important to get regularly tested once you have had any sexual activity. Young people less than 25 years of age should be screened on a yearly basis at minimum.