Search
-
-
12Dec
Space is limited for this event, and registration is required. This workshop is focused on understanding and completing a Nevada Durable Power of Attorney of Healthcare, also known as an Advance Directive. What to expect: A brief presentation about the document, its contents and purpose. Time for questions. Staff will be on hand to assist with document completion. A notary will be present for notarization. Participants may have their document uploaded into their Renown electronic medical record and/or submitted to the Nevada Living Will Lockbox on their behalf. Please come prepared with names, addresses, and phone numbers of those you want to appoint in the document and a photo ID if notarization is desired. All required paperwork will be provided by our staff. If you have questions about this workshop, please call Jessica Elmore, LMSW at 775-982-5098. There is no charge to attend this workshop.
Read More About Advance Directive Workshop
-
-
-
15Aug
Space is limited for this event, and registration is required. This workshop is focused on understanding and completing a Nevada Durable Power of Attorney of Healthcare, also known as an Advance Directive. What to expect: A brief presentation about the document, its contents and purpose. Time for questions. Staff will be on hand to assist with document completion. A notary will be present for notarization. Participants may have their document uploaded into their Renown electronic medical record and/or submitted to the Nevada Living Will Lockbox on their behalf. Please come prepared with names, addresses, and phone numbers of those you want to appoint in the document and a photo ID if notarization is desired. All required paperwork will be provided by our staff. If you have questions about this workshop, please call Jessica Elmore, LMSW at 775-982-5098. There is no charge to attend this workshop.
Read More About Advance Directive Workshop
-
-
-
20Jun
Space is limited for this event, and registration is required. This workshop is focused on understanding and completing a Nevada Durable Power of Attorney of Healthcare, also known as an Advance Directive. What to expect: A brief presentation about the document, its contents and purpose. Time for questions. Staff will be on hand to assist with document completion. A notary will be present for notarization. Participants may have their document uploaded into their Renown electronic medical record and/or submitted to the Nevada Living Will Lockbox on their behalf. Please come prepared with names, addresses, and phone numbers of those you want to appoint in the document and a photo ID if notarization is desired. All required paperwork will be provided by our staff. If you have questions about this workshop, please call Jessica Elmore, LMSW at 775-982-5098. There is no charge to attend this workshop.
Read More About Advance Directive Workshop
-
-
-
10Oct
Space is limited for this event, and registration is required. This workshop is focused on understanding and completing a Nevada Durable Power of Attorney of Healthcare, also known as an Advance Directive. What to expect: A brief presentation about the document, its contents and purpose. Time for questions. Staff will be on hand to assist with document completion. A notary will be present for notarization. Participants may have their document uploaded into their Renown electronic medical record and/or submitted to the Nevada Living Will Lockbox on their behalf. Please come prepared with names, addresses, and phone numbers of those you want to appoint in the document and a photo ID if notarization is desired. All required paperwork will be provided by our staff. If you have questions about this workshop, please call Jessica Elmore, LMSW at 775-982-5098. There is no charge to attend this workshop.
Read More About Advance Directive Workshop
-
-
Use Caution: Mixing Over-the-Counter Medications Can Be Harmful
With allergy season’s extended stay and cold and flu season having just begun, you may soon find yourself seeking relief through several different kinds of over-the-counter medications. Know what precautions you need to take when fighting multiple symptoms with multiple medications. When you’re too sick to go to work but not sick enough for a doctor’s visit, over-the-counter medicines are a welcome relief to help alleviate that fever, runny nose or allergies. But because those medicines aren’t signed off on or managed by your doctor and pharmacist, it’s crucial that you’re especially mindful of what you put into your body. Whenever you pop a pill, you want to make sure you’re taking the right dosage, waiting the right amount of time before taking another dose and not mixing certain medicines together. Recent stories like this one detail dangerous over-the-counter medicine combinations, and we’re following suit: Here is a quick go-to guide about potentially harmful over-the-counter combinations. Too Much Tylenol/Acetaminophen Tylenol — or acetaminophen — is a popular pain reliever for many, but too much can be bad for your liver. “Our bodies have a finite ability to metabolize Tylenol,” says Andy Wright, clinical pharmacist at Renown Rehabilitation Hospital. “When too much builds up in the liver, it becomes toxic. In patients with medical conditions like cirrhosis of the liver or hepatitis, this could be disastrous.” Remember, acetaminophen is in more than just Tylenol and generic pain relievers. You may also see acetaminophen in flu, cold and cough medicines, like Nyquil, and some prescription medications including Norco and Percocet. Keep a list of the medications you take, and limit daily acetaminophen use to 3,000 mg per day. When you’re scanning medicine bottle contents, remember acetaminophen is also referred to as APAP, AC, acetam or paracetamol. Mixing Painkillers When you’re dealing with pain and not getting any relief, taking a different medication may seem like the easy solution. Maybe you take some Aleve — a form of naproxen — for a headache, but it isn’t working, so you switch to Motrin, an over-the-counter form of ibuprofen. Not a smart idea. Ibuprofen and naproxen along with aspirin are known as nonsteroidal anti-inflammatory drugs (NSAIDS). Because these medicines work in similar ways, they should never be combined or used in larger doses or more frequently than directed. Otherwise your risk of side effects can increase, which range from mild nausea to severe gastrointestinal bleeding. It’s also important to consider your family history when taking NSAIDs because, “recent studies have shown NSAIDs may have greater cardiovascular risks for people taking blood thinners or those with hypertension,” explains Andy. “A good example is ibuprofen: It has a relatively low gastrointestinal bleed risk while it has a moderate to high cardiovascular risk. The opposite is true for naproxen.” Rather than experimenting with multiple medicines, figure out which drug works best for you. You may find muscle soreness improves with aspirin, whereas when a headache hits, naproxen is best. Keep in mind that these medications aren’t always best for everyone in the family. “Aspirin in children and teens is not recommended unless under the supervision of a doctor,” Andy says. And pregnant and lactating women should generally avoid NSAIDS due to risk of birth defects and bleeding. “In both of these cases, acetaminophen or Tylenol are preferred but only if approved by an OB/GYN.” Fighting Allergies Over-the-counter antihistamines like Claritin, Zyrtec and Allegra have made fighting itchy eyes and runny noses a little easier. But these daily medicines — when taken inappropriately or in the wrong combinations — can also have an adverse effect. Similar to acetaminophen, you need to watch for antihistamines in other products. Sleep aids — like Tylenol PM and Unisom — commonly use an antihistamine known as diphenhydramine, which may increase your risk of overdose. “Combining antihistamines, or overdosing, can cause many adverse effects including dry mouth, blurred vision — even arrhythmias,” Andy says. “Only take these medications on their own.” If you’re still struggling with symptoms, you can talk to your doctor about adding an over-the-counter nasal steroid. Andy confirms the importance of closely following the directions listed on antihistamine (and all medicine) bottles. He has seen extended release nasal decongestants cause significant arrhythmias requiring medical care after a patient took the medicine with warm fluids. “The decongestant in question is designed to slowly release, but it can dissolve suddenly in the presence of warm liquids like coffee,” Andy explains. “This can cause the pill to deliver 12 to 24 hours of medication all at once.” Taking an Antidiarrheal with Calcium Calcium supplements and antidiarrheal medicines are another harmful combination. Calcium firms up your stool, but if taken with an antidiarrheal, can cause severe constipation. If you need to take an antidiarrheal, take a break from your calcium for a few days until you’re back to normal. Another consideration when taking calcium supplements or calcium-based antacids is gas. “I’ve had several patients report cases of excessive gas using Tums or calcium carbonate-based supplements.” Andy suggests instead “trying Maalox or Mylanta for indigestion and Citracal as a supplement.” Talk with Your Doctor or Pharmacist About Your Medications If over-the-counter drugs aren’t providing the relief you need, it’s time to see your doctor. And remember, for your safety it is important to keep your doctor and pharmacist up-to-date with any medications — prescribed or over-the-counter — that you are taking.
Read More About Use Caution: Mixing Over-the-Counter Medications Can Be Harmful
-
CEO Blog: Improving Health Through Genetics and Big Data
Renown Health President and CEO Tony Slonim, MD, DrPH, discusses efforts nationwide to develop a more effective and efficient way to deliver care. explains the benefits of Renown Health’s population health study with the Desert Research Institute and 23andMe.
Read More About CEO Blog: Improving Health Through Genetics and Big Data
-
Here's How to Commemorate National Healthcare Decision Day
National Healthcare Decision Day is forthcoming. Here’s an easy and free way to commemorate the occasion: openly discussing how we want to be cared for at the end of our lives. Join Renown Health’s experts at a workshop about making decisions about an advance directive. Among the random national holidays, this one has significance: April 16 is National Healthcare Decision Day. And experts agree that the best time to discuss your views about end-of-life care and to learn what choices are available is before a life-limiting illness or crisis occurs. By preparing in advance, you can help reduce the doubt and anxiety related to decision making for your family if you cannot speak for yourself. “Completing your advance directive is a gift you give your family,” says Mary-Ann Brown, RN, MSN, director of Palliative Care. “The stress associated with these difficult decisions is decreased if everyone knows what is important to you and what you want the end of life.” What Are Advance Directives? An advance directive is a document that states your choices about medical treatment and names another person to make medical decisions on your behalf if you are unable to. This document allows you to make legally valid decisions about future medical care. Find more information about advance directives and the form online. The Conversation The first step in completing an Advance Directive is to think about what’s important to you and talk to your loved ones. The Conversation Project provides helpful tools to guide you and your family through this challenging topic. Getting this information together will help you fill out and complete your advance directives. Some things to consider and discuss with your family include: When you think about the last phase of your life, what’s most important to you? Who do you want involved in your care? Who should make decisions on your behalf if you’re not able to? Where do you want or not want to receive care? Are there specific treatments you would or would not want? Complete Your Advance Directive Planning In order to complete an advance directive, you will need either two witnesses or a notary to sign the form. Be sure to note restrictions on the witness process. When an advance directive is complete, you should keep the original. Copies should be given to your agent named in the form, your family, your doctor(s) and the location that you receive care. Renown Health offers four advance directive workshops every month to cover the details of filling out this document. A healthcare team is available to answer questions and work through the process with you. A notary is also present to finalize the process, which means you can complete your advanced directives during this workshop. Find the workshop by calling 775-982-RSVP for more information. Advance Care Planning Workshop April 17, 1-2:30 p.m. | Free Join Renown Health’s experts for a workshop about making decisions regarding end-of-life care. You will learn how to fill out an advance directive, receive one-on-one assistance and have your documents signed by a notary. Workshops are typically held several times each month. To RSVP, call 775-982-7787
Read More About Here's How to Commemorate National Healthcare Decision Day
-
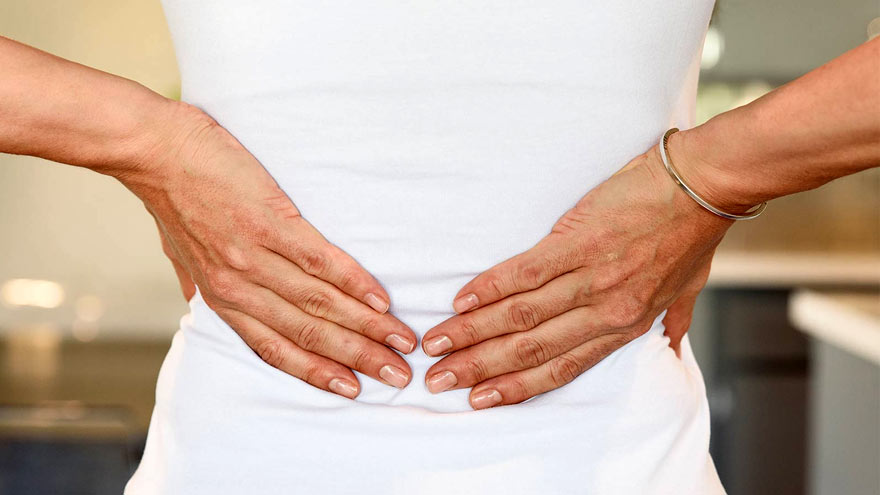
Low Back Pain – How to Stop the Ache
Low back pain is not only a problem most people have at some point in life, but also the leading cause of disability in the U.S. Whether it is a sharp spasm from lifting something heavy or a daily constant ache, there are various treatments available to relieve your pain. Jessica Ryder PT, DPT, cert VRS, with Renown Health Outpatient Therapy, explains some common causes of this pain, how to treat it and ways to prevent pain flare-ups. It’s important to realize most cases of low back pain are short term. Frequently lasting only a few days or weeks. In general these cases leave no long-term damage to the spine, muscles, discs or nerves. “However, it can become episodic or chronic (lasting longer than 12 weeks) if it is not properly understood or managed by the individual, ” cautions Ryder. Causes of Pain Specifically back discomfort can be related to: Wear and tear on the spine due to age or poor movement patterns Injury to spinal discs Sprains (overstretching or tearing of ligaments) and strains (tears in tendons or muscles) Trauma Irregularities of the spine present at birth (example: scoliosis)Notably the above issues may result in a “pinched nerve” or sciatica, causing pain to extend down the leg. Risk Factors for Pain In particular, your chance of developing low back pain increases with the risk factors below: Age Being overweight Low fitness level or occasional physical activity (“weekend warrior”) Family history Pregnancy Poor posture Jobs requiring heavy physical work (landscaping, plumbers, construction, etc.)
-
11 Tips Caregivers Need to Know
Becoming a caregiver or playing a more active role in another’s healthcare is a big responsibility. At some point, almost all adults will support an aging parent or a loved one in need. Keeping track of their needs and wellbeing, while also prioritizing your own can become overwhelming. It’s important to know: you are not alone, and help is available. Read on for 11 tips to help you manage your time, your own wellbeing and your loved one’s care. Self-care comes first. When your main priority is the person in your life who needs care, it’s easy for your own needs to take the backseat. Give yourself time each day to focus on your personal wellbeing. It’s hard to give a loved one the care they need if your own needs are not met. Prioritize the Activities of Daily Living (ADL). Make a note of what ADLs your loved one can do alone, what they need help with and what activities require the most help. This will help you work through the day with them, as well as plan out how the day’s activities will go. Do a home safety audit. Do showers, bathtubs and steps have safety grab bars? Look around the house for additional tripping hazards, like rugs or electrical cords. If your loved one struggles with day-to-day navigation of the home, consider scheduling an occupational therapy appointment. This type of therapy helps a person develop or maintain the motions required to accomplish daily tasks. You might also qualify for a referral to in-home healthcare, such as Home Care. Have the hard conversation. The best time to discuss views about end of life care and to learn what choices are available is before a life-limiting illness or crisis occurs. With advance care planning, you can help reduce the doubt and anxiety related to decision making at the end of life. Completing an Advance Directive is a great tool to sort out all these decisions before they’re needed. Attend a free workshop to learn more and complete this important document. Identify when you need respite. Respite care involves receiving a short-term break from caregiving. Organizing in-home care for your loved one will allow you to step away and tend to your needs. By identifying what kind of respite care you are seeking, you can find the right person to provide you with that much-needed break. Don’t wait until you feel overwhelmed, plan ahead. Write down insurance contact information. Have a direct connection to the right insurance professional for support and advice. If your loved one is eligible Medicare, this is a good opportunity to review their current selections and if they would benefit from a Medicare Advantage Plan or Medicare Supplement Insurance. Seeking out expert advice or information on Medicare options is a great way to navigate this. Consider calling a broker, or attend a free educational seminar with Senior Care Plus. Gather legal and financial information. Make a list of all existing legal documents and financial accounts that your loved one has. These might include a will, advance directive, power of attorney, bank accounts or investment accounts. If you have questions about how to manage them, or need assistance in setting up additional framework, reach out to a lawyer, legal service, financial adviser or bank representative. Create an inventory of medical information. Identify where all of your loved one’s medical records are, as well as a list of providers or healthcare practices where they have received care. Consider if you should have your loved one give you Proxy Access in MyChart, which allows you to access all the features in MyChart on their behalf, including viewing upcoming appointments, viewing test results and emailing a doctor on their behalf. Make a list of what others can do. Think about all the little (and big) things that need to happen, and write down tasks that others could take care of you. When someone says “let me know what I can do” you’ll be ready with a pre-written list of items they may be able to assist with. Tasks could include tackling around-the-house repairs, scheduling lawn work, helping to walk the dog, taking a car for an oil change and cleaning. Find programs and events for social enjoyment. If and when possible, seek an activity outside of the home. Look for community centers that have programs for seniors, recreational activities or meals that you can patriciate in together. If leaving the home is not an option, arrange for visits or in-home activities, such as movie nights, card games or time to visit with family. Research long-term options. If you will be considering a nursing home or assisted living, make a list of amenities that you and the person you are caring for would like. Take this list with you when visiting potential locations to make sure you don’t forget to ask about each item.
-
Renown Health Vision for Value Based Care
In recent years, healthcare has undergone many important transitions. One of the greatest changes has been the transition from a fee-for-service model to a value-based care model. Historically, healthcare organizations were paid for the amount of services they performed. This payment model resulted in more tests and procedures ordered, which, in turn, increased our country’s health care costs. However, now our government incentivizes health systems to provide the highest quality of care at the lowest cost possible. This new payment model is called value-based purchasing or value-based care. In this model, providers focus on delivering more coordinated and effective care. Additionally, healthcare organizations track important metrics like patient engagement, population health, and hospital readmissions. At Renown Health, we know that progress on these metrics represents real improvements in our patients’ lives. Shifting Focus from Illness to Wellness Healthcare organizations have traditionally viewed a hospital stay as the center of a patient’s wellness journey. At Renown Health, we believe a key part of our job is to help people live well every day. This means we focus not only on treating illness and injury but also on prevention efforts to keep people out of the hospital. For example, our employees help patients hazard-proof their homes to prevent falls, as falls are the leading cause of injuries in older adults. We also provide affordable health screenings to catch disease in its early stages, when it is more treatable. Renown Health also recognizes that many of the diseases our patients face – from diabetes to cancer – have social and environmental origins. We know that creating a healthier community will have a positive impact on their physical and mental health. Renown Health partners with local organizations to address community-based issues like addiction, pedestrian safety, air and water quality, climate change, and nutrition. Working together, we can lower the number of people who need care and improve the health and wellbeing of our community. Creating healthier environments and communities will help us prevent disease, which in turn will help us decrease spending and improve health. Most importantly, it will help people live up to their full potential. Dr. Slonim on Twitter | @RenownCEOTonyMD Interested in hearing more of Dr. Slomin’s thoughts on health and healthcare? Engage with him on Twitter. Follow Tony
-
My Inspiration to Keep Fighting Becoming a Grandparent
As a clinician and a cancer survivor, I know that hope is an essential force that drives people to work through difficult situations. I also believe there’s a strong correlation between hope and wellness. Hope inspires us to make healthy choices today with the understanding that these behaviors will benefit us in the future. In addition, an optimistic outlook helps patients face illness and injury with strength and confidence. While it’s easy for some people to maintain a positive outlook, it’s common to feel hopeless on a bad day. An important part of our job as healthcare providers is to help patients cultivate hope and build a strong foundation that carries them through their medical journey. The Importance of Family A common source of hope, for me and many others, is family. My family has recently welcomed our newest member, my first granddaughter, Emory. Becoming a grandparent has inspired me to reflect on the many blessings in my life. It’s not only been a opportunity to reflect, but also look ahead to the future. I often dream about the things Emory will accomplish one day, the kind of person she will become, and the world I want her to live in. These aspirations have renewed my determination to work hard and lead by example. At Renown Health, we know that hope and resilience are just as important in the recovery process as excellent medical care. That’s why we work with our patients to find sources of strength and inspiration in their own lives. We’re committed to helping our patients keep fighting the good fight for a healthier tomorrow.
Read More About My Inspiration to Keep Fighting Becoming a Grandparent
-
Beyond Jello A Healthier Approach to Hospital Food
Hospital food gets a bad rap and maybe it’s deserved. However, at Renown Health we strive to serve patients, visitors and staff meals that are both nutritious and delicious. In this video and blog post, Renown Health President and CEO, Tony Slonim, M.D., Dr.PH., FACHE, shares his thoughts on hospital food and modeling healthy lifestyles. Everyone knows that what we eat matters for almost every aspect of our health. Eating well can prevent chronic disease, control weight, improve our mood and even strengthen our bonds with loved ones as we come together to enjoy a family meal. Yet despite this knowledge, balancing work or school responsibilities, family life and everything in between can make eating healthy feel like an uphill battle. Recognizing this challenge, Renown Health invests in programming to help our community embrace healthy lifestyle habits – starting with our own employees. Knowing that people often look to their healthcare providers to model healthy behavior, we are deliberate in our efforts to help our employees and their families live well. We also provide healthy dining options in our on-campus restaurants and through our food and nutrition services team. We believe that providing nutritious, appetizing meals helps patients to recuperate from illness or injury, helps their families recharge, and helps our staff fulfill their promise of providing outstanding care. We hope that by serving as models of healthy behaviors, our employees will inspire others to join us in this journey. Dr. Slonim on Twitter | @RenownCEOTonyMD Interested in learning more of Dr. Slomin’s thoughts on health and healthcare? Engage with him on Twitter. Follow Tony
Read More About Beyond Jello A Healthier Approach to Hospital Food